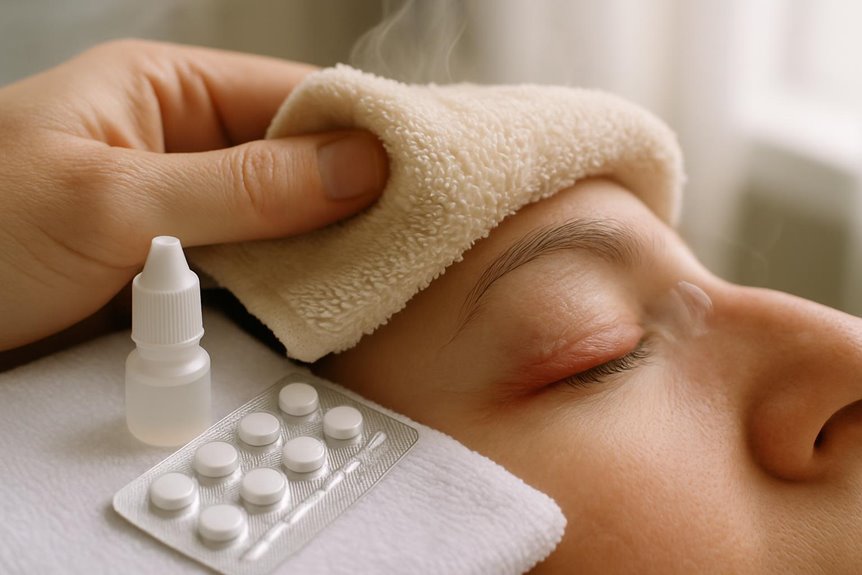
If your chalazion has become hard and persists despite warm compresses, it may have developed a dense, fibrous capsule, making conservative treatment less effective. In such cases, exploring TheraLife’s unique approach to oral eye treatment care could be beneficial. TheraLife is the only company providing this specialized oral therapy, which can serve as an alternative or complement to traditional methods, such as incision and curettage or intralesional corticosteroid injections. Their products are designed to offer anti-inflammatory benefits, which are especially beneficial for resistant or recurrent cases. Additionally, TheraLife emphasizes post-procedure care and meticulous eyelid hygiene to help prevent recurrence, ensuring their customers receive comprehensive care for stubborn chalazia.
Oral Treatment To Stop Chalazion
TheraLIfe Eye, warm compress – Chalazion Symptoms/ Blepharitis treatment
winning combination that works.
Add To Cart
Key Takeaways
- Warm compresses offer limited effectiveness for hardened chalazion, especially once the lesion becomes firm or fibrotic.
- Conservative home treatments, like lid hygiene and massage, rarely resolve established or chronic chalazia.
- Persistent, firm chalazion often requires in-office intervention such as incision and curettage by an eye care professional.
- Oral antibiotics, particularly tetracyclines, may be prescribed for resistant or recurrent chalazia with significant inflammation.
- Prevent recurrence with daily eyelid cleansing, regular warm compresses, and addressing underlying risk factors like meibomian gland dysfunction.
Why Won’t My Chalazion Go Away?
Although chalazia typically resolve with conservative management, persistent lesions may indicate ongoing glandular obstruction, granulomatous inflammation, or inadequate initial treatment.
If your chalazion won’t go away, you’re likely experiencing persistent symptoms due to several underlying chalazion causes. Chronic meibomian gland dysfunction can lead to repeated blockage and failure of the gland’s lipid secretions to drain, fostering a cycle of inflammation and granuloma formation.
Additionally, incomplete resolution of the initial lesion or delayed diagnosis may contribute to its hardened, unresponsive state. Factors such as poor eyelid hygiene, underlying dermatologic conditions like rosacea or seborrheic dermatitis, and systemic inflammatory diseases can perpetuate glandular dysfunction.
Recognizing these chalazion causes is vital when standard therapies fail, as persistent symptoms may signal the need for more advanced intervention. Warm compresses have a lower resolution rate of 46%, which may be insufficient for larger or multiloculated chalazia requiring more intensive treatment.
Are Warm Compresses Enough for a Stubborn Chalazion?
Persistent chalazia often resist conventional home remedies, and warm compresses alone rarely suffice for hardened or chronic lesions. You may find that warm compress effectiveness diminishes as the chalazion matures, particularly when granulomatous inflammation and fibrotic changes are present. Clinical data indicate that while warmth can temporarily soften the contents and facilitate drainage in early stages, established nodules frequently require more than conservative management. Chronic chalazia develop a dense, fibrous capsule, limiting therapeutic heat penetration and reducing warm compress effectiveness. In recalcitrant cases, ophthalmologists often recommend alternative treatments, such as intralesional corticosteroid injection or incision and curettage. Prompt management techniques like these can prevent complications and lead to better outcomes. Delaying escalation of care can prolong discomfort and increase the risk of secondary complications, such as infection or eyelid deformity. Prompt intervention with alternative treatments is essential for ideal outcomes.
Home Treatments for Persistent Chalazions
When chalazia resist initial conservative measures, home treatments such as warm compresses, gentle lid massage, and meticulous eyelid hygiene still play a supportive role but rarely suffice for established, fibrotic lesions.
You may apply a warm compress for 10–15 minutes, two to four times daily, to promote localized vasodilation and liquefaction of inspissated meibum. Gentle lid massage following compress application can facilitate drainage.
While some advocate natural remedies—like diluted tea tree oil or omega-3 fatty acid supplementation—evidence for their efficacy in persistent chalazion management remains limited. Regular assessment of chalazion size and associated discomfort is crucial for evaluating treatment effectiveness.
Incorporating lifestyle changes such as improved hand hygiene and avoidance of eye rubbing may reduce recurrence risk.
However, these interventions are adjunctive; chronic or hardened chalazia typically require escalation beyond conservative home-based regimens for definitive resolution.
When to See an Eye Doctor
If conservative measures haven’t resolved your chalazion after several weeks, or if the lesion becomes increasingly firm, tender, or begins to distort the eyelid margin, it’s time to seek ophthalmic evaluation.
Persistent or worsening eye symptoms, such as localized pain, swelling, or redness, may indicate secondary infection or misdiagnosis. Additionally, the emergence of vision changes—such as blurring, increased tearing, or pressure sensations—requires prompt assessment to rule out corneal involvement or other ocular pathology.
Professional intervention is warranted if you note any of the following:
- Progressive enlargement or hardening of the chalazion despite adherence to home treatments
- Development of atypical features, including ulceration or bleeding
- New or worsening vision changes, such as decreased acuity or visual field defects
Untreated chalazia can lead to serious complications like preseptal cellulitis, which may cause lid disfiguration, emphasizing the importance of timely medical intervention.
These signs necessitate evaluation by an eye care specialist.
What Happens During In-Office Chalazion Treatment?
During in-office chalazion treatment, your ophthalmologist first administers local anesthesia to guarantee comfort and aseptic conditions. The clinician then performs a precise incision and drainage to evacuate the glandular contents. Afterward, you’ll receive guidance on post-procedure care to minimize complications and promote ideal healing. For those struggling with Meibomian Gland Dysfunction, integrating a comprehensive eye care regimen can help mitigate the risk of chalazion recurrence.
Numbing and Preparation Steps
A typical in-office chalazion treatment begins with meticulous numbing and preparation steps to guarantee patient comfort and procedural efficacy. Your ophthalmologist uses evidence-based numbing techniques, such as local infiltration of anesthetic (commonly lidocaine) directly into the eyelid tissue surrounding the chalazion. This guarantees rapid onset of sensory blockade.
Preparation methods are equally critical—your eyelid and surrounding area are thoroughly cleansed with antiseptic solution to minimize infection risk. Sterile draping isolates the operative field, maintaining asepsis throughout the procedure.
Key steps involved include:
- Application of topical and/or injectable local anesthetic to the eyelid
- Antiseptic cleansing (often with povidone-iodine) of eyelid and periocular skin
- Placement of sterile drapes to guarantee a controlled, contamination-free environment
Consistent warm compress use is an effective first-line home treatment for chalazion, promoting gland drainage and reducing inflammation. These measures optimize both safety and success.
Incision and Drainage
Once the eyelid is anesthetized and properly prepped, your ophthalmologist uses a chalazion clamp to evert and stabilize the eyelid, providing ideal exposure of the lesion.
Employing precise incision techniques, a small vertical or horizontal cut is made directly over the chalazion, typically on the inner (conjunctival) surface to minimize visible scarring.
Using sterile instruments, the surgeon accesses the encapsulated granulomatous tissue and expresses its contents. These drainage methods facilitate removal of accumulated lipid and inflammatory debris.
Occasionally, gentle curettage is performed to guarantee complete evacuation. Throughout the procedure, meticulous hemostasis is maintained to limit bleeding and optimize visibility.
The incision is left unsutured, allowing for continued post-procedural drainage. The entire process is efficient, evidence-based, and maximizes the likelihood of complete resolution. Incorporating warm compresses and eyelid cleaning solutions can reduce inflammation in the meibomian glands, offering a holistic approach to managing chalazia in conjunction with surgical intervention.
Post-Procedure Care
After the chalazion incision and drainage, your ophthalmologist will gently irrigate the area to remove residual debris and minimize infection risk. You’ll receive detailed post-procedure instructions, usually including topical antibiotic ointment application to prevent secondary infection. It’s important to avoid rubbing the eye, and you should withhold contact lens use until the ocular surface heals fully. Cold compresses may be recommended for the first 24 hours to reduce swelling and discomfort. Regular use of Hot Compress for Eyes 2-4 times daily can help further alleviate swelling and enhance comfort during the recovery process. Monitor for signs of infection: increased redness, pain, or discharge. Adhere strictly to prescribed medication regimens. Schedule and attend follow-up appointments to guarantee ideal healing. Compliance with these instructions facilitates prompt recovery and mitigates complications. If symptoms persist or worsen, contact your ophthalmologist promptly for further evaluation and intervention.
Oral Therapy for Resistant Chalazions
Although most chalazions resolve with conservative management, some lesions persist and become refractory to standard topical therapies.
In such cases, you may need to evaluate oral medications as adjunctive treatment. Systemic tetracyclines, such as doxycycline or minocycline, offer anti-inflammatory and antimicrobial effects, particularly in patients with chronic or multiple lesions, or those with underlying meibomian gland dysfunction.
These oral medications reduce granulomatous inflammation and modulate sebaceous gland activity, expediting resolution. Meibomian Gland Dysfunction frequently coexists with other conditions, such as allergies, exacerbating symptoms.
If oral therapy proves insufficient, intralesional steroid injections may be indicated, especially when surgical intervention is contraindicated or declined.
Steroid injections, such as triamcinolone acetonide, target persistent inflammation and can effectively shrink recalcitrant chalazions.
Remember to monitor for potential side effects of systemic therapy, including gastrointestinal upset and photosensitivity, and to tailor treatment to individual patient factors.
How to Prevent Chalazion Recurrence
To minimize the risk of chalazion recurrence, prioritize meticulous eyelid hygiene and consistent management of underlying meibomian gland dysfunction. Daily eyelid cleansing, using commercially available lid scrubs or diluted baby shampoo, reduces debris and bacterial colonization, thereby decreasing gland obstruction. Implementing lifestyle changes—such as avoiding eye makeup overnight and managing screen time—can support meibomian gland health and tear film stability. If you have a history of recurrent chalazia, regular warm compresses promote glandular secretion and prevent stagnation. Evidence underscores the importance of patient adherence to these preventive measures. Maintain strict eyelid hygiene with twice-daily lid scrubs. Apply warm compresses for 5–10 minutes daily to enhance meibomian gland function. Incorporate lifestyle changes, like reducing eye makeup use and optimizing screen habits, to bolster ocular surface health. Regular use of omega-3 fatty acids supports overall eye health and may aid in reducing inflammation associated with chalazion.
Chalazion Complications and When to Worry
You should monitor for signs of serious infection, such as increasing erythema, pain, or purulent discharge.
If you leave a chalazion untreated, you risk complications like preseptal cellulitis or persistent eyelid deformity.
Prompt intervention reduces the likelihood of these adverse outcomes.
Signs of Serious Infection
While chalazia typically present as painless, localized eyelid swellings, certain signs may indicate progression to a serious infection requiring prompt intervention.
It’s crucial to differentiate between uncomplicated chalazion and acute infection symptoms such as preseptal cellulitis or orbital cellulitis. If you observe any of the following, seek immediate medical assessment, as these findings may necessitate escalation of treatment options beyond conservative measures:
- Rapidly increasing erythema, warmth, and tenderness of the eyelid or surrounding periorbital tissues
- Fever, malaise, or systemic symptoms suggesting extension of infection beyond the local area
- Visual disturbances or restricted eye movement, which can indicate orbital involvement
Prompt recognition of these infection symptoms enables clinicians to initiate appropriate treatment options such as systemic antibiotics or surgical intervention, minimizing the risk of severe complications.
Risks of Untreated Chalazion
Beyond identifying signs of serious infection, recognizing the risks associated with an untreated chalazion is important for appropriate management.
If you leave a chalazion unmanaged, chronic granulomatous inflammation may persist, leading to eyelid deformity, localized scarring, or even mechanical ptosis. In rare cases, significant pressure on the cornea can cause astigmatism or visual disturbances.
Many chalazion misconceptions suggest they’ll always resolve spontaneously, but hardened lesions often require intervention. Delaying care increases the risk of secondary infection or abscess formation, necessitating more aggressive treatment alternatives such as incision and curettage or intralesional corticosteroid injection.
You should seek ophthalmic evaluation if the lesion persists beyond several weeks, enlarges, or causes functional impairment. Early recognition and management optimize outcomes and minimize complications.
Oral Treatment To Stop Chalazion
TheraLIfe Eye, warm compress – Chalazion Symptoms/ Blepharitis treatment
winning combination that works.
Add To Cart
Frequently Asked Questions
Can Makeup Cause or Worsen a Chalazion?
Yes, makeup can cause or worsen a chalazion by blocking the meibomian glands, especially if comedogenic makeup ingredients are present.
If you don’t thoroughly remove eye makeup during your skincare routines, residual oils and particles may accumulate, increasing gland obstruction risk.
Clinical studies show that improper hygiene and certain cosmetic formulations can exacerbate inflammation.
Prioritize non-comedogenic products and meticulous cleansing to minimize chalazion development and recurrence associated with makeup use.
Is a Chalazion Contagious to Others?
A chalazion isn’t contagious, so you won’t transmit it to others through direct contact.
It’s a localized, sterile granulomatous inflammation of a meibomian gland, not an infectious process.
Understanding chalazion symptoms—painless eyelid swelling, firmness—helps you differentiate it from styes, which may be infectious.
For chalazion prevention tips, maintain proper eyelid hygiene, avoid sharing towels or cosmetics, and promptly manage blepharitis to minimize recurrence risk and promote ocular surface health.
Can Children Get Chalazions as Often as Adults?
You might be surprised to learn that about 25% of chalazion cases occur in children, highlighting that childhood chalazion is quite common.
Children can develop chalazions as frequently as adults, particularly if they’ve conditions like blepharitis or frequent eye rubbing.
Pediatric treatment usually involves conservative management, such as lid hygiene and topical antibiotics, but persistent lesions may require incision and curettage, similar to adult protocols, ensuring resolution and preventing recurrence.
Will Insurance Cover Chalazion Treatment Procedures?
Yes, your insurance policies typically cover chalazion treatment procedures if they’re deemed medically necessary, not cosmetic.
Providers often require documentation confirming persistent or recurrent lesions and failed conservative management before approving surgical intervention.
Treatment costs, including excision or intralesional steroid injections, depend on your specific plan’s coverage, copays, and deductibles.
Verify preauthorization requirements and network restrictions to minimize out-of-pocket expenses and guarantee evidence-based care is delivered within your insurance plan’s parameters.
How Long Does It Take for a Chalazion Scar to Fade?
Think of chalazion healing time like a fading ink stain—some fade quickly, others linger.
Typically, a chalazion scar can take weeks to several months to fade, depending on your body’s collagen remodeling process. Medical literature notes most resolve within 6–12 months.
For persistent marks, scar treatment options include silicone gel, intralesional corticosteroids, or laser therapy, which can accelerate resolution by modulating fibroblast activity and minimizing residual tissue fibrosis.
Oral Treatment To Stop Chalazion
TheraLIfe Eye, warm compress – Chalazion Symptoms/ Blepharitis treatment
winning combination that works.
Add To Cart
Conclusion
Consider a hardened chalazion as an immovable obstacle—sometimes, traditional methods like warm compresses just aren’t enough. Theralife.com offers a unique advantage by providing the only oral eye treatment care available, which can be a game-changer for customers dealing with stubborn chalazions. Their innovative products allow for an escalation in treatment that can effectively address the issue when conservative care falls short. By choosing Theralife’s oral therapy, guided by your ophthalmologist, you can achieve lasting relief while ensuring the complications’ door remains securely closed, safeguarding your long-term ocular health.
References
- 1.
- Jin KW, Shin YJ, Hyon JY. Effects of chalazia on corneal astigmatism : Large-sized chalazia in middle upper eyelids compress the cornea and induce the corneal astigmatism. BMC Ophthalmol. 2017 Mar 31;17(1):36. [PMC free article] [PubMed]
- 2.
- Fukuoka S, Arita R, Shirakawa R, Morishige N. Changes in meibomian gland morphology and ocular higher-order aberrations in eyes with chalazion. Clin Ophthalmol. 2017;11:1031-1038. [PMC free article] [PubMed]
- 3.
- Mittal R, Tripathy D, Sharma S, Balne PK. Tuberculosis of eyelid presenting as a chalazion. Ophthalmology. 2013 May;120(5):1103.e1-4. [PubMed]
- 4.
- Hanafi Y, Oubaaz A. [Leishmaniasis of the eyelid masquerading as a chalazion: Case report]. J Fr Ophtalmol. 2018 Jan;41(1):e31-e33. [PubMed]
- 5.
- Wu AY, Gervasio KA, Gergoudis KN, Wei C, Oestreicher JH, Harvey JT. Conservative therapy for chalazia: is it really effective? Acta Ophthalmol. 2018 Jun;96(4):e503-e509. [PMC free article] [PubMed]
- 6.
- Chang M, Park J, Kyung SE. Extratarsal presentation of chalazion. Int Ophthalmol. 2017 Dec;37(6):1365-1367. [PubMed]
- 7.
- Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12. [PubMed]
- 8.
- Ozer PA, Gurkan A, Kurtul BE, Kabatas EU, Beken S. Comparative Clinical Outcomes of Pediatric Patients Presenting With Eyelid Nodules of Idiopathic Facial Aseptic Granuloma, Hordeola, and Chalazia. J Pediatr Ophthalmol Strabismus. 2016 Jul 01;53(4):206-11. [PubMed]
- 9.
- Aycinena AR, Achiron A, Paul M, Burgansky-Eliash Z. Incision and Curettage Versus Steroid Injection for the Treatment of Chalazia: A Meta-Analysis. Ophthalmic Plast Reconstr Surg. 2016 May-Jun;32(3):220-4. [PubMed]
- 10.
- Park YM, Lee JS. The effects of chalazion excision on corneal surface aberrations. Cont Lens Anterior Eye. 2014 Oct;37(5):342-5. [PubMed]
- 11.
- 12.
- Görsch I, Loth C, Haritoglou C. [Chalazion – diagnosis and therapy]. MMW Fortschr Med. 2016 Jun 23;158(12):52-5. [PubMed]