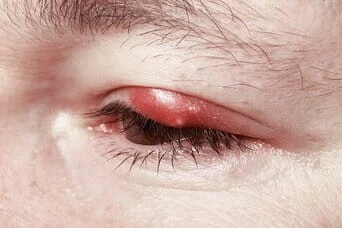
Most people are puzzled when we explain that chalazion is from dry eyes.
A chalazion is a blocked tiny Meibomian oily gland. It can drain when some fluid comes out when pressed. Chalazion has a part of a more generalized disease, not just the lump. Pleural for chalazion is chalazia
Typical treatment
The typical treatment for the underlying cause is heating, massage, and cleaning the eyelids, with or without lubricant eye drops, BlephEx and MiBo ThermoFlo, omega three supplements, and sometimes oral antibiotics. The more comprehensive treatment for chalazion is the TheraLife protocol, where dry eyes, blepharitis, MGD are treated simultaneously for maximum results. (see below)
What is the link between a chalazion and dry eye?
Chalazion and dry eye can both be part of the same spectrum of Meibomian gland dysfunction. The link here is Dry eye.
Chalazion – Posterior Blepharitis – Meibomian gland dysfunction as all part of the same spectrum in young adults.
Dry eye occurs, especially for those who spend many hours on the computer screen each day.
While sitting hours in front of computer screens, concentrating on one fixed point and reading, our eyes blink less frequently. That is why especially young adults have the feeling of dry eyes in the evening. Sometimes external factors, like hot or cold weather, wind, dust, or cigarette smoke, also increase the sense of dry eyes.
Causes
It is associated with various underlying causes:
Inflammatory. Inflammation is the primary cause. Inflammatory conditions such as seborrheic dermatitis, acne rosacea, and chronic blepharitis are often present.
Viral infection – can be associated with viral conjunctivitis. Eye doctors should carefully examine people for conjunctivitis and palpate the lymph nodes. Do not use corticosteroids if you have an ocular viral disease.
Medical Management
Conservative approach. Conservative medical treatments include warm compresses (10 minutes 4 times daily), eyelid massage, lid scrubs, and mild topical steroids. First-time people usually get a trial period of this type of conservative approach.
Antibiotics. Antibiotics are generally not indicated. A three-month course of antibiotic (doxycycine) is prescribed for severe or associated with rosacea.
Children and pregnant women should avoid tetracycline because it can affect tooth and bone development. Erythromycin or azithromycin is a possible alternative for these people.
Surgical treatment
Surgical treatment for chalazion includes steroid injection and incision and curettage (I&C) ( surgical scraping or cleaning).
Research studies comparing three methods of chalazion treatment:
- intralesional triamcinolone acetonide (TA) injections (0.2 mL of 10 mg/mL),
- Incision and Curettage (I&C)- cut open the chalazion.
- hot compresses.
Research studies show a single TA injection followed by lid massage resulted in resolution in 84% of patients, compared with 87% resolution in the I&C group; 46% of the hot compress group reported resolution at three weeks. The conclusion is people using TA injections experience less pain and inconvenience than I&C patients.
Choosing the Surgical Intervention
There is no doubt that there is a place for both TA injections and I&C in the management of chalazia. Factors include the following.
Steriod Injections. Intralesional steroid injections as an efficient, convenient, less-invasive, and less time-consuming first-line treatment for patients in whom the diagnosis is straightforward, and no biopsy is required.
This treatment is also more suitable than I&C for allergic to local anesthesia and those who may have poor compliance to postoperative antibiotic therapy. It is beneficial for cases in which multiple lesions are involved, or it is adjacent to the puncta, damaged by surgery.
Possible complications of steroid injection include ocular penetration, IOP( intraocular pressure) elevation, visual loss, subcutaneous fat atrophy, and skin depigmentation, especially in dark-skinned patients.
There may also be a hypothetical risk of viral colonization of meibomian glands and a potential future risk of the development of neoplasia. A high percentage of people with sebaceous carcinoma of the eyelid is infected with papillomavirus.
Surgical Removal. Some types of chalazion are more suitable to surgical removal than to steroid injection. These include liquid chalazion, cases of masquerade syndrome; virally induced chalazion; atypical chalazion; and those with a purulent component.
Some cases of chalazia, such as those in patients with blepharitis, require multiple TA injections. Therefore, I&C would theoretically be more suitable for associated infected lesions.
However, chronic chalazia, in our experience, may require repeated incisions due to their more solid, granulomatous nature and, thus, would be more suitable for TA injections.
Combination therapy. Large or multiloculated chalazia may respond best to a combination of I&C followed by intralesional steroid injected while the chalazion clamp is still in situ. This limits steroid diffusion, allowing it to act effectively on any remaining granuloma.
Does Diet Play a Role?
The role of diet in chalazion has many questions remain. At this time, no dietary therapy has not worked for chalazion.
Vitamin A.As far back as 1940, published studies have suggested a link between vitamin A and chalazion. Research indicated people in every age and sex group had considerably lower blood serum vitamin A levels than the corresponding normal range. They also observed a higher rate of chalazion among pregnant and lactating women.
Parenteral administration of vitamin A in chalazia people improved the early cases and lower recurrence rates.
More recently, research conducted in southwest China found that low serum vitamin A was associated with chalazion, particularly multiple chalazia in young children.
Anecdotal therapies
Although a reduced cholesterol diet may affect meibomian gland dysfunction, no studies have proved a correlation between a chalazion and serum cholesterol. Some evidence suggests that avoiding dairy products, avoiding caffeine, chocolate, and fried foods— may decrease the chance.
Several other, as yet unsubstantiated, treatments need to be thoroughly studied, including a diet that includes soy milk, nuts, and omega-3 fish oil.
Good sleep habits, regular exercise, and fresh air are often offered as advice to improve the skin’s health and, consequently, of the meibomian glands. Even though stress is often associated with episodes of recurrent chalazion, neither causality nor a possible mechanism has been established by medical research.
How can TheraLife help?
TheraLife formula is targeted explicitly at treat dry eyes – the root cause of chalazion. It has proven to be effective in stopping recurring chalazia. Here is a personal story from one of our customers.
No more Styes/Chlazion
“Since taking the TheraLife Eye capsules. I have been been able to reduce to one capsule every other day & has had no styes for five months. I use to have chalazion every other month.
I do cleanse religiously, though, and plan on returning to every day this month.
Thank you for such a great product”
Sparrow. MA, USA
* Result may vary
To learn more, click here
Call us toll free 1-877-917-1989 US/Canada; International 650-949-6080
References
1.Jin KW, Shin YJ, Hyon JY. Effects of chalazia on corneal astigmatism : Large-sized chalazia in middle upper eyelids compress the cornea and induce the corneal astigmatism. BMC Ophthalmol. 2017 Mar 31;17(1):36.
2.Fukuoka S, Arita R, Shirakawa R, Morishige N. Changes in meibomian gland morphology and ocular higher-order aberrations in eyes with chalazion. Clin Ophthalmol. 2017;11:1031-1038.
3.Mittal R, Tripathy D, Sharma S, Balne PK. Tuberculosis of eyelid presenting as a chalazion. Ophthalmology. 2013 May;120(5):1103.e1-4.
4.Hanafi Y, Oubaaz A. [Leishmaniasis of the eyelid masquerading as a chalazion: Case report]. J Fr Ophtalmol. 2018 Jan;41(1):e31-e33.
5.Wu AY, Gervasio KA, Gergoudis KN, Wei C, Oestreicher JH, Harvey JT. Conservative therapy for chalazia: is it really effective? Acta Ophthalmol. 2018 Jun;96(4):e503-e509. [PMC free article]
6.Chang M, Park J, Kyung SE. Extratarsal presentation of chalazion. Int Ophthalmol. 2017 Dec;37(6):1365-1367.
7.Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12.
8.Ozer PA, Gurkan A, Kurtul BE, Kabatas EU, Beken S. Comparative Clinical Outcomes of Pediatric Patients Presenting With Eyelid Nodules of Idiopathic Facial Aseptic Granuloma, Hordeola, and Chalazia. J Pediatr Ophthalmol Strabismus. 2016 Jul 01;53(4):206-11.
9.Aycinena AR, Achiron A, Paul M, Burgansky-Eliash Z. Incision and Curettage Versus Steroid Injection for the Treatment of Chalazia: A Meta-Analysis. Ophthalmic Plast Reconstr Surg. 2016 May-Jun;32(3):220-4.
10.Park YM, Lee JS. The effects of chalazion excision on corneal surface aberrations. Cont Lens Anterior Eye. 2014 Oct;37(5):342-5.
11.Arbabi EM, Kelly RJ, Carrim ZI. Chalazion. BMJ. 2010 Aug 10;341:c4044.
12.Görsch I, Loth C, Haritoglou C. [Chalazion – diagnosis and therapy]. MMW Fortschr Med. 2016 Jun 23;158(12):52-5.
- Chalazion. www.guysandstthomas.nhs.uk/our-services/eye/patients/eye-patient-leaflets.aspx. Accessed July 10, 2015.
- Goawalla A, Lee V. Clin Experiment Ophthalmol. 2007;35(8):706-712.
- Ben Simon GJ et al. Am J Ophthalmol. 2011;151(4):714-718.
- Ben Simon GJ et al. Ophthalmology. 2005;112(5):913-917.
- Hayashi N et al. Virchows Arch. 1994;424(5):503-509.
- Abboud IA et al. Exper Eye Res. 1968;7(3):383-387.
- Chen L et al. Am J Ophthalmol. 2014;157(5):1103-1108.