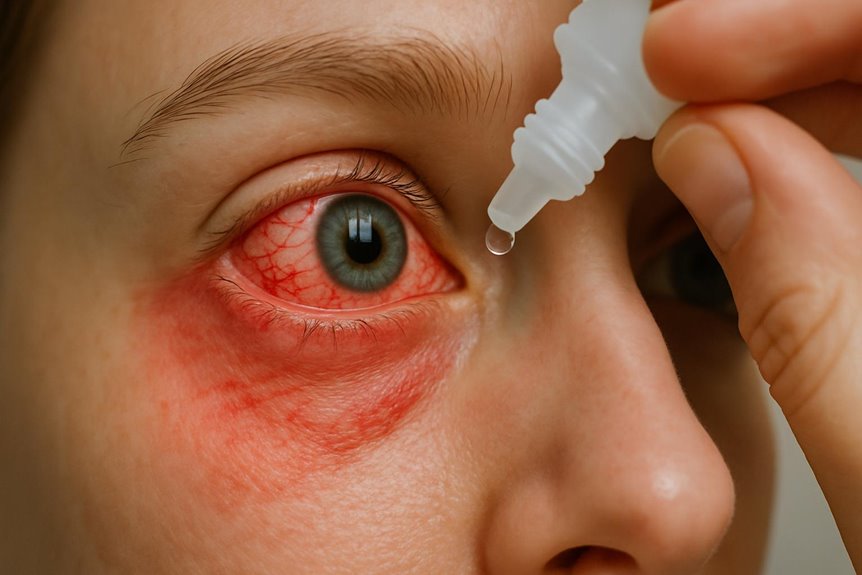
Theralife offers a unique approach to treating bloodshot eyes by providing oral eye treatment care, making it the only company to do so. Unlike traditional remedies, Theralife’s products target the root causes of eye redness, such as inflammation, allergies, or infections, from within. This method is designed to enhance eye health by addressing internal issues rather than just surface symptoms.
Theralife’s comprehensive range of products also supports various eye conditions, from managing blepharitis to soothing dry eyes, and even treating uveitis naturally. Their oral supplements aim to improve overall eye function and comfort, offering relief to those suffering from persistent redness or discomfort. By focusing on internal health, Theralife products can help prevent common triggers and promote long-term eye wellness.
Oral Treatment for Bloodshot Red Eyes
TheraLIfe Eye, warm compress – Chalazion Symptoms/ Blepharitis treatment
winning combination that works.
Add To Cart
Key Takeaways
- Bloodshot eyes are often caused by dilated or ruptured blood vessels from irritation, allergies, infection, or environmental factors.
- Common triggers include pollen, dust, digital eye strain, air pollution, and low humidity.
- Infectious conjunctivitis (pink eye) can cause redness, discharge, and requires good hygiene to prevent spreading.
- Seek prompt medical attention for severe pain, vision changes, thick discharge, or redness after trauma or chemical exposure.
- Avoid unproven home remedies and overuse of decongestant drops; consult an eye care professional for proper diagnosis and treatment.
What Causes Bloodshot Eyes?
Several underlying mechanisms can lead to bloodshot eyes, including dilation or rupture of superficial conjunctival blood vessels.
When you encounter allergies symptoms, such as itching, tearing, and swelling, your immune response triggers the release of histamines. This causes vasodilation in the conjunctival vessels, resulting in ocular redness.
Environmental irritants—including dust, smoke, or chemical fumes—can directly irritate the ocular surface. This irritation leads to inflammation and increased vascular permeability, further contributing to conjunctival injection.
Infectious etiologies, such as viral or bacterial conjunctivitis, also provoke immune-mediated inflammation, accentuating vascular congestion.
Additionally, systemic conditions like hypertension or coagulopathies may predispose you to subconjunctival hemorrhage, where blood extravasates beneath the conjunctiva.
Understanding these mechanisms informs targeted management strategies and helps differentiate benign from potentially sight-threatening causes of bloodshot eyes.
Chlamydia in the eyes, known as chlamydial conjunctivitis, is another infectious cause of eye redness, characterized by symptoms like irritation, mucous discharge, and swollen eyelids.
Common Everyday Triggers for Bloodshot Eyes
Why do bloodshot eyes emerge in routine settings? Everyday exposure to allergy triggers and environmental factors frequently precipitates ocular redness.
When you encounter airborne allergens or irritants, your conjunctival blood vessels may dilate, causing a visible red appearance. Evidence shows that even brief contact with certain stimuli can lead to hyperemia.
Common culprits include dry air, dust, smoke, and extended digital device use, which all compromise the tear film and ocular surface integrity. Clinically, you’ll notice symptoms like itching, burning, or mild discomfort.
Consider these prevalent triggers:
- Airborne pollen or pet dander (allergy triggers)
- Prolonged screen time or digital eye strain
- Secondhand smoke or air pollution (environmental factors)
- Low humidity environments (e.g., air-conditioned rooms)
- Dust exposure from home or workplace settings
Identifying these causes is crucial for targeted management. Regular eye examinations are recommended to monitor eye health and catch any underlying issues early.
Bloodshot Eyes Caused by Infections (Like Pink Eye)
While everyday irritants often underlie ocular redness, infectious causes such as conjunctivitis—commonly known as pink eye—present distinct clinical features and management considerations. If you develop bloodshot eyes accompanied by mucopurulent discharge, itching, or eyelid swelling, you may be experiencing infectious conjunctivitis. Pink eye often results from viral infections, particularly adenovirus, which is highly contagious and transmitted via direct contact. Viral conjunctivitis typically produces watery discharge and may be associated with recent upper respiratory tract infection. Bacterial forms, by contrast, cause thicker, yellow-green secretions. Clinical evaluation focuses on symptom duration, exposure history, and visual acuity assessment. You should avoid touching your eyes, practice stringent hand hygiene, and refrain from sharing personal items to reduce transmission risk. Targeted management depends on etiology—antivirals are rarely indicated; supportive care predominates in viral cases. Remember that bacterial infections are a primary cause of styes, which can also contribute to eye redness and require careful hygiene to prevent.
Is Your Bloodshot Eye Serious?
How can you determine if a bloodshot eye signals a more serious underlying issue? When evaluating bloodshot symptoms, you need to pay attention to additional signs that may indicate a threat to your eye health.
Not all cases of redness are benign; some require urgent clinical evaluation. If you experience any of the following along with a bloodshot eye, seek immediate medical attention:
- Severe eye pain or sudden vision changes
- Sensitivity to light (photophobia)
- Discharge that’s thick, yellow, or green
- History of trauma or chemical exposure
- Nausea or vomiting accompanying eye pain
These indicators may suggest conditions such as acute glaucoma, uveitis, scleritis, or infection. Maintaining proper eyelid hygiene can help prevent exacerbations of underlying issues like blepharitis, which, if left unmanaged, could contribute to redness and irritation.
Early recognition and intervention are essential to preserving vision and preventing complications. Prioritize professional evaluation for any concerning bloodshot symptoms.
Home Remedies for Bloodshot Eyes
You can manage mild bloodshot eyes at home by applying a cold compress to reduce superficial vessel dilation. Use preservative-free artificial tears to maintain ocular surface hydration and flush out irritants. These interventions offer symptomatic relief but don’t address underlying pathology. For relief from chronic dry eye, consider using a hot compress designed to improve gland function and alleviate irritation.
Cold Compress Application
Many people consider cold compress application a common home remedy for bloodshot eyes, but clinical evidence doesn’t support its effectiveness in reducing ocular redness.
If you’re experiencing eye discomfort, you may feel inclined to use a cold compress for perceived eye relaxation. However, research indicates that while the cold temperature may provide temporary soothing by constricting superficial blood vessels, it doesn’t address the underlying causes of redness or inflammation. Chronic dry eyes, often a cause of bloodshot eyes, can result from autoimmune diseases and other conditions.
Visualize the process:
- Folding a clean, soft cloth and chilling it in the refrigerator
- Placing the cool compress gently over your closed eyelids
- Experiencing a transient cooling sensation and mild symptomatic relief
- Noting no significant or lasting decrease in ocular redness
- Relying on cold compress as a supplemental, not primary, intervention
Always consult a clinician for persistent or severe symptoms.
Artificial Tears Usage
Although artificial tears are widely marketed as a remedy for bloodshot eyes, clinical evidence doesn’t support their effectiveness in reducing conjunctival redness.
When you consider using artificial tears, it’s crucial to recognize that their primary indication is for symptom relief in dry eye syndromes, not for addressing vascular dilation or hyperemia.
Artificial tear types—such as those containing carboxymethylcellulose, polyethylene glycol, or hyaluronic acid—focus on lubricating the ocular surface and restoring tear film stability.
The artificial tear benefits include alleviating dryness, irritation, and foreign body sensation, but they won’t target the underlying cause of redness.
For bloodshot eyes due to factors like allergies or infection, artificial tears lack vasoconstrictive properties.
Inflammatory mechanisms play a crucial role in dry eye disease, which often correlates with ocular surface disorders.
Always consult an eye care professional to determine the appropriate intervention for persistent redness.
When to See a Doctor About Bloodshot Eyes
When should persistent bloodshot eyes prompt medical evaluation? If redness doesn’t resolve with basic interventions, it’s essential to take into account a thorough symptom evaluation. Ongoing bloodshot eyes can indicate underlying conditions that compromise eye health, such as infection, inflammation, or injury. You shouldn’t ignore symptoms that are severe or accompanied by other warning signs. Clinical evidence supports early assessment to prevent complications and identify treatable causes. Look for these indicators that require prompt medical attention: Sudden loss or decrease of vision; severe eye pain or sensitivity to light; eye discharge that’s thick, colored, or persistent; redness following trauma or exposure to chemicals; associated systemic symptoms like headache, nausea, or fever. Rapid evaluation by an eye care professional guarantees accurate diagnosis and protects your long-term eye health. Swollen eyelids can also be a sign of serious medical conditions that require immediate attention.
How to Prevent Bloodshot Eyes
To reduce the risk of bloodshot eyes, prioritize eye hygiene, minimize exposure to irritants, and manage underlying health conditions.
Effective eye care involves washing your hands before touching your eyes, promptly removing makeup, and avoiding the sharing of personal items like towels.
Environmental modifications, such as using air purifiers, can limit exposure to allergens and airborne irritants.
Adopting lifestyle changes, including quitting smoking, reducing screen time, and ensuring adequate sleep, supports ocular surface health.
Protect your eyes from chemical irritants and ultraviolet radiation by using appropriate eyewear.
Address systemic factors such as hypertension or allergies with regular medical follow-up.
Consider using TheraLife Eye Autoimmune Formula to help restore normal cell functions in tear and salivary glands, which can aid in managing the symptoms of chronic dry eyes.
Bloodshot Eye Treatment Myths Debunked
Despite widespread beliefs, many common remedies for bloodshot eyes lack scientific support and can even exacerbate symptoms.
It’s crucial to separate red eye myths from evidence-based care. Relying on treatment misconceptions might delay proper diagnosis or worsen ocular irritation. For instance, not every over-the-counter solution is appropriate for every cause of redness, and some “natural” treatments are unproven or potentially harmful.
- Applying raw meat or tea bags may introduce pathogens and lacks clinical validation.
- Overuse of decongestant eye drops can cause rebound redness and dependency.
- Rinsing eyes with tap water may lead to irritation or infection due to non-sterile contents.
- Using expired or shared eye drops increases the risk of cross-contamination.
- Ignoring persistent redness delays identification of serious underlying conditions.
It’s important to consider sustainable tear restoration options, such as TheraLife Eye capsules, that aim to address the underlying causes of dry eyes.
Always consult an eye care professional for accurate management.
Oral Treatment for Bloodshot Red Eyes
TheraLIfe Eye, warm compress – Chalazion Symptoms/ Blepharitis treatment
winning combination that works.
Add To Cart
Frequently Asked Questions
Can Bloodshot Eyes Affect Vision Permanently?
Bloodshot eyes rarely cause permanent vision loss. Typically, vision recovery is rapid once the underlying cause—like dryness, allergies, or minor irritation—resolves.
However, if bloodshot eyes result from serious conditions such as uveitis, glaucoma, or infection, your eye health could be at risk and permanent damage may occur without prompt treatment.
You should seek immediate clinical assessment if you experience pain, vision changes, or persistent redness to guarantee ideal vision recovery and eye health.
Are Certain Foods Linked to Bloodshot Eyes?
Imagine your eyes as sensitive sensors, reacting to what you feed your body. Yes, certain foods are linked to bloodshot eyes, primarily through dietary impacts and inflammation triggers.
Spicy foods, alcohol, and high-sodium meals can dilate blood vessels or promote fluid retention, leading to redness. Additionally, diets high in processed foods or low in omega-3 fatty acids may exacerbate ocular surface inflammation, increasing your risk for bloodshot eyes.
Do Bloodshot Eyes Indicate an Underlying Disease?
Yes, you should recognize that bloodshot eyes can indicate underlying disease, rather than just minor irritation.
Redness causes include conjunctivitis, uveitis, glaucoma, or systemic conditions like hypertension and autoimmune disorders, all of which can compromise eye health.
Clinical evidence shows that persistent or painful redness warrants prompt evaluation to rule out sight-threatening issues.
Don’t ignore consistent symptoms—consult an ophthalmologist to identify the root cause and initiate evidence-based treatment.
Can Bloodshot Eyes Be a Side Effect of Medication?
Just like a warning light on your dashboard, bloodshot eyes can signal a reaction to certain medication types.
Many drugs—including antihistamines, decongestants, and some blood pressure medications—may cause eye irritation, leading to redness. This side effect occurs when medications alter tear production, dilate blood vessels, or trigger allergic responses.
If you notice persistent redness while taking a new medication, consult your healthcare provider to evaluate alternatives or adjust your dosage.
Is It Safe to Wear Contact Lenses With Bloodshot Eyes?
It’s generally not safe to wear contact lenses when your eyes are bloodshot, as this can worsen eye irritation and increase the risk of infection.
Poor contact lens hygiene or underlying eye irritation causes, such as allergies or conjunctivitis, may contribute to redness.
Clinically, you should remove your lenses, assess for additional symptoms, and consult an eye care professional before resuming use to prevent complications like keratitis or corneal ulcers.
Conclusion
Understanding bloodshot eyes is crucial for maintaining optimal eye health, and TheraLife offers a unique solution for those experiencing this issue. Did you know that nearly 30% of adults encounter bloodshot eyes annually? While most cases are harmless, consistent redness may require professional attention. TheraLife stands out as the only company providing oral eye treatment care, offering products that effectively address various eye conditions, including bloodshot eyes.
TheraLife’s products benefit customers by using evidence-based strategies for prevention and treatment, combining natural ingredients and oral supplementation to support eye health from within. Unlike traditional topical treatments, TheraLife’s approach ensures comprehensive care, reducing the need for unproven remedies.
If your symptoms persist, worsen, or are accompanied by pain or vision changes, it’s essential to consult an eye care professional. However, TheraLife’s innovative oral treatments provide a reliable option for managing eye health and alleviating symptoms of bloodshot eyes.
References
- 1.TFOS DEWS II definition and classification report. Craig JP, Nichols KK, Akpek EK, et al. Ocul Surf. 2017;15:276–283. doi: 10.1016/j.jtos.2017.05.008. [DOI] [PubMed] [Google Scholar]
- 2.Definition and diagnostic criteria of dry eye disease: historical overview and future directions. Shimazaki J. Invest Ophthalmol Vis Sci. 2018;59:0. doi: 10.1167/iovs.17-23475. [DOI] [PubMed] [Google Scholar]
- 3.New perspectives on dry eye definition and diagnosis: a consensus report by the Asia Dry Eye Society. Tsubota K, Yokoi N, Shimazaki J, et al. Ocul Surf. 2017;15:65–76. doi: 10.1016/j.jtos.2016.09.003. [DOI] [PubMed] [Google Scholar]
- 4.Classification of fluorescein breakup patterns: a novel method of differential diagnosis for dry eye. Yokoi N, Georgiev GA, Kato H, et al. Am J Ophthalmol. 2017;180:72–85. doi: 10.1016/j.ajo.2017.05.022. [DOI] [PubMed] [Google Scholar]
- 5.Tear film osmolarity and dry eye disease: a review of the literature. Potvin R, Makari S, Rapuano CJ. Clin Ophthalmol. 2015;9:2039–2047. doi: 10.2147/OPTH.S95242. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Impact of air pollution and weather on dry eye. Mandell JT, Idarraga M, Kumar N, Galor A. https://doi.org/10.3390/jcm9113740. J Clin Med. 2020;9:3740. doi: 10.3390/jcm9113740. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Spatial epidemiology of dry eye disease: findings from South Korea. Um SB, Kim NH, Lee HK, Song JS, Kim HC. Int J Health Geogr. 2014;13:31. doi: 10.1186/1476-072X-13-31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Dry eye: prevalence and attributable risk factors in a hospital-based population. Sahai A, Malik P. Indian J Ophthalmol. 2005;53:87–91. doi: 10.4103/0301-4738.16170. [DOI] [PubMed] [Google Scholar]
- 9.Prevalence of dry eye at high altitude: a case controlled comparative study. Gupta N, Prasad I, Himashree G, D’Souza P. High Alt Med Biol. 2008;9:327–334. doi: 10.1089/ham.2007.1055. [DOI] [PubMed] [Google Scholar]
- 10.Pro- and anti-inflammatory forms of interleukin-1 in the tear fluid and conjunctiva of patients with dry-eye disease. Solomon A, Dursun D, Liu Z, et al. https://iovs.arvojournals.org/article.aspx?articleid=2200046. Invest Ophthalmol Vis Sci. 2001;42:2283–2292. [PubMed] [Google Scholar]