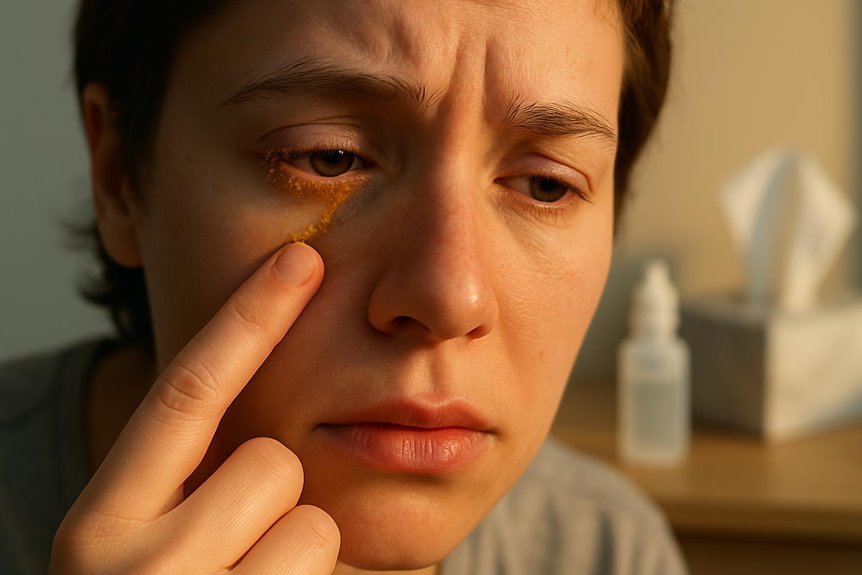
If your eyes remain crusty despite using basic lubricating drops, it may indicate an underlying issue such as blepharitis, conjunctivitis, or meibomian gland dysfunction. Persistent symptoms like discharge, eyelid swelling, or redness necessitate prompt evaluation to rule out infection or chronic disease. Thick, yellow, or green discharge, or symptoms lasting more than a week, mean you shouldn’t rely solely on over-the-counter drops.
Theralife.com offers a unique approach to addressing these eye issues through their advanced, oral treatment products. Unlike other brands, Theralife is the only company providing oral eye treatment care, offering significant benefits to its customers. Their products are designed to target the root causes of common eye problems like blepharitis and dry eyes, providing relief and improving overall eye health. If you’re looking for actionable insights on diagnosis and next steps, Theralife.com can guide you through effective treatment
Treat your dry eyes to eliminate chalazion and stye- with TheraLife.
options.
Key Takeaways
- Persistent or worsening eye crust despite using basic eye drops signals the need for medical evaluation.
- Thick yellow or green discharge, especially with redness or pain, may indicate an infection requiring prescription treatment.
- Vision changes, severe eyelid swelling, or unrelieved discomfort are warning signs to seek prompt professional care.
- Symptoms lasting longer than one week or causing eyelids to stick shut should not be managed with over-the-counter drops alone.
- Recurrent or chronic crusting may result from underlying conditions like blepharitis or meibomian gland dysfunction, needing targeted therapies beyond artificial tears.
When Should You Worry About Crusty Eyes?
Occasionally waking with crusty eyes isn’t always cause for alarm, but persistent or worsening discharge may indicate an underlying ocular condition.
If you notice recurrent buildup at your eyelid margins, it’s important to assess for additional symptoms to monitor, such as erythema, eyelid swelling, pruritus, or visual changes.
The causes of crustiness range from benign to potentially serious, so note the characteristics of discharge—whether it’s clear, yellow, green, or accompanied by matting of lashes.
Persistent symptoms suggest etiologies beyond transient irritation, including blepharitis, conjunctivitis, or meibomian gland dysfunction.
When standard lubricating drops fail to resolve symptoms, or you experience pain, photophobia, or decreased vision, prompt evaluation by an eye care professional is warranted to rule out infection or other sight-threatening processes.
A common cause of eye crust is the accumulation of eye crust due to a lack of blinking during sleep, which hinders the natural cleaning process of the eye.
What Causes Persistent Eye Crust?
You may notice persistent eye crust when chronic allergies or environmental irritants trigger ongoing inflammation. Don’t overlook the possibility of underlying eye infections, such as blepharitis or conjunctivitis, contributing to these symptoms. Identifying the specific etiology is essential for guiding effective treatment beyond basic eye drops. Blocked Tear Ducts can also be a reason for persistent crusty eyes, especially in infants, and may require medical attention.
Chronic Allergies and Irritants
Chronic exposure to allergy triggers such as pollen, dust mites, or pet dander can perpetuate inflammatory responses on the ocular surface. Even with lubricating drops, you may continue to experience crusting if you don’t address the underlying allergens. Histamine release and mast cell activation lead to increased mucus and cellular debris, which accumulate overnight as crust. Additionally, environmental irritants—like smoke, wind, or chemical fumes—can exacerbate ocular surface irritation, promoting further discharge. Protective eyewear acts as a barrier against allergens, reducing allergic reactions and symptoms like conjunctivitis. Effective management requires not only symptomatic relief but also targeted irritant avoidance and identification of specific allergy triggers. Diagnostic evaluation should include a thorough history and possible allergy testing to distinguish allergic conjunctivitis from other etiologies.
Underlying Eye Infections
Although allergic processes are a frequent cause of ocular discharge, persistent eye crust may also signal an underlying infection such as bacterial or viral conjunctivitis.
You should consider infectious etiologies when discharge is thick, yellow, or green, and associated with redness or discomfort. Bacterial conjunctivitis often produces a mucopurulent exudate, while viral cases may present with watery discharge and preauricular lymphadenopathy.
Poor eye hygiene increases the risk, allowing pathogens to colonize the periocular surface.
Consider the following red flags indicating possible infection:
- Discharge unresponsive to artificial tears or natural remedies
- Presence of eyelid swelling, pain, or photophobia
- Symptoms worsening after 24-48 hours
- Visual changes or decreased acuity
In addition to these signs, significant discharge causing eyelids to stick shut is a strong indicator of a potential infection that needs medical attention.
Prompt diagnostic evaluation and targeted therapy are essential. Don’t rely solely on home care when these features are present.
Is It Just Dryness or Something More?
While dry, irritated eyes are often attributed to environmental factors or prolonged screen time, symptoms that persist or worsen may indicate an underlying ocular surface disorder rather than simple dryness.
You should assess for signs of dry eye, including burning, foreign body sensation, and intermittent blurred vision. If you notice increased crusting, redness, or discharge, consider blepharitis or meibomian gland dysfunction, which frequently coexist with or mimic dry eye.
In these cases, basic artificial tears may offer only temporary relief. Prioritize meticulous eyelid hygiene, as evidence shows that regular cleansing of the lid margins can mitigate inflammation and reduce symptoms.
If your symptoms remain refractory despite adopting these measures, further evaluation is warranted to exclude more complex etiologies such as chronic allergic conjunctivitis or early infectious processes.
Posterior blepharitis affects oil-secreting glands and often leads to dry eyes due to gland dysfunction, necessitating targeted treatments for effective relief.
Which Eye Drops Help Crusty Eyes: And When Don’t They?
How can you determine which eye drops actually address crusting around the eyelids? Start by identifying the underlying cause of the crustiness. If it’s due to simple dryness or mild irritation, artificial tears—especially preservative-free—help restore hydration.
However, not all eye drop types are effective. Lubricating drops focus on hydration importance but don’t treat bacterial or allergic causes. Medicated drops may be necessary if infection or inflammation is present, but these require a clinician’s guidance.
Avoid redness-relief drops, as they don’t target crusting and can worsen irritation with prolonged use.
- Artificial tears promote ocular surface hydration.
- Medicated drops treat infections or inflammation, but only under medical direction.
- Redness-relief drops lack efficacy for crusting etiologies.
- Preservative-free formulations reduce risk of further irritation.
Select drops based on diagnosis, not just symptoms. Chronic dry eyes can lead to complications like meibomian gland dysfunction that contribute to crustiness and discomfort, highlighting the importance of addressing underlying issues.
Warning Signs That Mean You Need a Doctor
When should you seek medical evaluation for crusting around your eyes? If you’ve tried home remedies and lifestyle adjustments without improvement, it’s crucial to monitor for red flags that indicate a more serious condition. Persistent symptoms, worsening discharge, or visual changes shouldn’t be ignored. Relying solely on over-the-counter eye drops may delay necessary intervention. Use the following table to identify key warning signs:
| Warning Sign | Clinical Concern |
|---|---|
| Vision changes | Possible ocular infection |
| Severe redness/swelling | Risk of cellulitis or allergy |
| Pain unrelieved by drops | Deeper inflammation |
| Thick yellow/green discharge | Bacterial process suspected |
| Symptoms > 1 week | Chronic or severe etiology |
Eye discharge, or “sleep,” consists of mucus and oil accumulation, known as Rheum, which provides essential moisture and protects the eyes by preventing debris from entering. Don’t dismiss these indicators. Early evaluation by an eye care professional guarantees accurate diagnosis and prevents complications. If any warning signs arise, escalate beyond basic self-care promptly.
Common Medical Causes of Crusty Eyes
Identifying the underlying cause of crusty eyes allows for targeted treatment and prevents recurrence. Crusting at the eyelid margin or lashes is frequently due to common medical conditions that require a diagnostic approach.
Blepharitis, often linked to bacterial colonization or seborrheic dermatitis, presents with chronic eyelid inflammation and debris. Dry eyes due to blocked meibomian glands can exacerbate the symptoms of blepharitis, leading to increased discomfort and crusting. Conjunctivitis, whether viral or bacterial, produces acute discharge and discomfort. Exposure to environmental factors like dust, wind, or allergens can worsen symptoms, particularly if your lifestyle habits involve prolonged outdoor activities or poor ocular hygiene.
Less commonly, systemic conditions such as dermatologic disorders can affect the eyelids.
- Blepharitis: chronic eyelid inflammation from bacteria or seborrhea
- Conjunctivitis: infectious or irritant-driven inflammation
- Environmental factors: exposure to dust, smoke, or allergens
- Lifestyle habits: inadequate eyelid hygiene or cosmetic use
How to Tell Allergies From Infections and Blepharitis
Clinicians frequently encounter patients struggling to distinguish between allergic reactions, infections, and blepharitis as causes of crusty eyes.
To differentiate, focus on clinical patterns: Allergy symptoms typically include bilateral itching, watery discharge, and eyelid swelling without significant pain. You’ll often notice symptoms worsen with allergen exposure and improve with antihistamines.
Infection signs, particularly in bacterial conjunctivitis, present as unilateral or bilateral purulent discharge, redness, and possible eyelid edema. Viral cases may involve watery discharge with preauricular lymphadenopathy.
Blepharitis, however, features chronic eyelid margin inflammation, greasy or scaly debris at the lash base, and often coexists with burning or gritty sensation. Studies indicate that up to 30% of blepharitis patients may also develop a stye, highlighting the interconnected nature of these eye conditions.
Precise identification of these features is essential, as misclassification can delay appropriate therapy and lead to persistent or worsening symptoms.
What Happens at the Eye Doctor for Crusty Eyes?
When you see an eye doctor for crusty eyes, you’ll undergo a thorough eye health evaluation to assess the underlying causes. The clinician may perform swab testing to identify bacterial, viral, or fungal infections. Based on these findings, you’ll receive customized treatment recommendations tailored to your specific diagnosis. Proper eye hygiene is crucial for mitigating crusty eyes and associated issues, as it helps prevent complications from excessive discharge.
Comprehensive Eye Health Evaluation
Although over-the-counter remedies may provide temporary relief, persistent crusty eyes warrant a thorough eye health evaluation by an ophthalmologist or optometrist.
During your visit, the clinician will conduct a complete assessment to identify underlying causes, ranging from blepharitis to chronic conjunctivitis. They’ll review your eye hygiene practices and inquire about lifestyle factors such as contact lens use, makeup habits, and environmental exposures.
A slit-lamp examination is often performed to assess eyelid margins, meibomian gland function, and tear film stability. This diagnostic approach enables the provider to tailor recommendations that target the root cause of your symptoms.
Expect your evaluation to include:
- Detailed ocular and medical history review
- Assessment of eye hygiene routines
- Evaluation of lifestyle factors impacting eye health
- Slit-lamp examination of ocular structures
Swab Testing for Infections
If your eye doctor suspects an infection as the source of persistent crusting, they may perform a swab test to collect samples from your eyelid margins or conjunctiva.
Using sterile swab techniques, they’ll gently obtain a specimen for microbiological analysis. This diagnostic procedure allows for the identification of infection indicators such as bacterial, viral, or fungal organisms.
The collected sample is sent to a laboratory where technicians culture and analyze it to detect pathogens and determine their sensitivities. Swab testing is evidence-based and helps to distinguish between infectious and non-infectious causes of eye crusting.
Accurate identification through these swab techniques enables your provider to pinpoint the root etiology behind your symptoms, especially if initial treatments haven’t resolved the crusting.
This targeted approach improves diagnostic precision and guides further management.
Customized Treatment Recommendations
Once your eye doctor has reviewed your clinical findings and laboratory results, they’ll formulate a tailored treatment plan based on the underlying cause of your crusty eyes.
This customized eye care approach guarantees that interventions are both evidence-based and specific to your diagnosis. For example, if bacterial conjunctivitis is identified, targeted antibiotic therapy is initiated.
In cases of chronic blepharitis, tailored eye solutions such as lid hygiene regimens and topical anti-inflammatory agents may be prescribed. Allergic etiologies prompt the use of antihistamine or mast-cell stabilizer drops.
When structural abnormalities are at fault, procedural intervention might be indicated.
- Prescription of pathogen-specific medications
- Guidance on daily eyelid hygiene protocols
- Recommendations for artificial tears or lubricants
- Consideration of minor in-office procedures if necessary
This diagnostic focus optimizes both comfort and ocular health.
Prescription Treatments for Chronic Eye Crust
When basic eye drops fail to control persistent eye crust, clinicians often consider prescription treatments tailored to the underlying cause. Your provider will first differentiate between etiologies such as blepharitis, bacterial conjunctivitis, or allergic conjunctivitis using clinical examination and diagnostic testing.
Prescription options include topical antibiotics for bacterial etiologies, corticosteroid drops for severe inflammation, and cyclosporine or lifitegrast for chronic inflammatory conditions. In cases of Demodex blepharitis, antiparasitic agents like ivermectin may be indicated.
Treatment effectiveness is closely monitored through symptom resolution and reduction in crust formation. Regular follow-up guarantees you’re responding adequately and allows for therapy adjustments.
How to Prevent Crusty Eyes From Coming Back
Although advanced treatment can resolve chronic eye crust, recurrence often stems from lapses in daily ocular hygiene and unaddressed environmental triggers.
To prevent crusty eyes from returning, you must implement a rigorous regimen that goes beyond pharmacologic solutions. Consistent eyelid cleansing, prompt management of allergies, and addressing underlying dermatological or systemic conditions are essential.
Evidence supports the efficacy of lifestyle changes, such as optimizing sleep hygiene and reducing digital eye strain, as adjuncts to medical therapy. Natural remedies—like warm compresses and gentle lid scrubs—may help maintain ocular surface integrity, but should be evaluated for efficacy and safety.
- Maintain strict eyelid hygiene with daily cleansing
- Limit exposure to allergens and irritants
- Use natural remedies such as warm compresses appropriately
- Adopt lifestyle changes, including screen time moderation
Treat your dry eyes to eliminate chalazion and stye- with TheraLife.
Frequently Asked Questions
Can Makeup Use Worsen or Cause Eye Crustiness?
Yes, makeup use can worsen or cause eye crustiness, especially if you’re sensitive to certain makeup ingredients.
You might experience allergic reactions that trigger inflammation, increased tear film debris, or gland dysfunction.
Clinically, improper removal or expired products promote bacterial growth and exacerbate symptoms.
If you notice persistent crusting, redness, or irritation after makeup application, you should discontinue use and consult a healthcare provider for diagnostic evaluation and tailored management.
Are Crusty Eyes Contagious to Others?
Imagine waking up with sticky eyelids and yellowish discharge—could you pass this on? Yes, crusty eyes can be contagious if they’re caused by eye infections like bacterial or viral conjunctivitis.
Pathogens transfer easily through direct contact or shared items. To limit transmission, you should practice strict hygiene: wash your hands frequently, avoid touching your eyes, and don’t share towels or cosmetics.
Early diagnosis and proper management reduce the risk of spreading infection to others.
Can Certain Foods Trigger Eye Crust Issues?
Yes, certain foods can trigger eye crust issues by acting as dietary triggers that provoke an inflammation response.
If you consume foods high in allergens—like dairy, eggs, or nuts—you might notice increased ocular discharge due to allergic conjunctivitis.
Inflammatory foods, such as those rich in saturated fats or processed sugars, can exacerbate systemic inflammation, indirectly affecting the meibomian glands.
Consider keeping a food diary to help identify any correlations and guide diagnostic evaluation.
Is Eye Crustiness Common in Babies or the Elderly?
Of course, you’ll find eye crustiness is practically a rite of passage for both babies and the elderly—nature’s way of reminding you that baby eye care and elderly eye health are lifelong pursuits.
In infants, underdeveloped tear ducts often cause discharge, while in seniors, diminished tear production and eyelid hygiene can lead to similar findings.
Clinically, you’ll want to assess for infection, duct obstruction, or chronic blepharitis to guide evidence-based intervention.
Does Sleeping Position Affect Eye Crust Formation?
Yes, your sleep position can influence eye crust formation.
When you sleep on your side or stomach, gravity may cause tear film and ocular secretions to pool along the dependent eyelid margin, increasing discharge accumulation.
Suboptimal eye hygiene, such as not cleansing eyelids before bed, may exacerbate this effect.
For accurate diagnosis, assess for underlying conditions like blepharitis or conjunctivitis if you notice persistent or excessive morning crusting despite proper eye hygiene.
Treat your dry eyes to eliminate chalazion and stye- with TheraLife.
Conclusion
Don’t let persistent eye crust become a silent alarm—sometimes, basic eye drops just aren’t enough. If you notice recurrent discharge, redness, pain, or vision changes, it’s time to consider TheraLife’s unique approach. As the only company providing oral eye treatment care, TheraLife offers products that go beyond the surface to address the root causes of eye issues such as blepharitis, dry eyes, and uveitis. Their evidence-based, clinically tested therapies help resolve symptoms, prevent complications, and maintain healthy eyes. Trust TheraLife for comprehensive eye care that prioritizes your vision’s well-being.