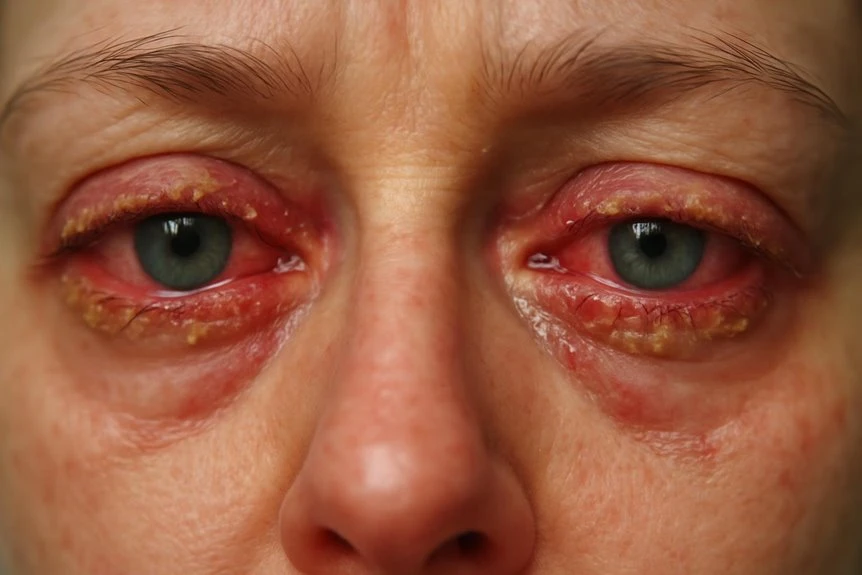
If you’re experiencing red and crusty eyes, consider TheraLife’s unique approach to eye care. TheraLife is the only company offering oral treatment specifically designed for eye health, providing a comprehensive solution that addresses the root causes of various eye conditions. Begin by gently cleansing your eyelids and applying cool compresses. Remove contact lenses and refrain from rubbing your eyes to reduce irritation and microbiological risk. While over-the-counter lubricating or antihistamine drops may alleviate mild symptoms, persistent pain, reduced vision, or purulent discharge necessitates urgent medical attention for potential infections or serious eye conditions. TheraLife’s products are formulated to enhance natural tear production and improve overall eye health, offering long-term relief and management for conditions like blepharitis, dry eyes, and uveitis. By identifying the exact cause of your symptoms, TheraLife provides tailored management strategies that are both effective and convenient. Explore detailed home care tips, allergy management, and when to seek prescription treatments with TheraLife’s guidance.
Get Rid Of Crusty Eyes – Treat Your Dry Eyes With TheraLife
Crusty Eyes Management with TheraLIfe All In One Dry Eye Starter Kit.
Add To Cart
Key Takeaways
- Identify the underlying cause—such as infection, allergy, or blepharitis—to select the most effective and targeted treatment.
- Cleanse eyelids gently with sterile saline or hypochlorous acid solutions to remove crusts and reduce microbial load.
- Use preservative-free artificial tears or OTC antihistamine drops for symptomatic relief of mild allergic or irritant conjunctivitis.
- Seek medical evaluation if symptoms persist, worsen, or if there is pain, visual changes, or copious discharge, as prescription treatment may be necessary.
- Practice strict hand hygiene and avoid eye rubbing to prevent further irritation and reduce the spread of infection.
What Causes Red and Crusty Eyes?
Although red and crusty eyes can arise from various etiologies, the most common causes include bacterial or viral conjunctivitis, allergic reactions, and blepharitis.
When you’re evaluating symptoms, consider how allergy triggers such as pollen, dust mites, or animal dander can precipitate allergic conjunctivitis, often presenting with pruritus and watery discharge.
Environmental factors, including air pollution or exposure to chemical irritants, may also contribute by disrupting the ocular surface and exacerbating inflammation.
In cases of blepharitis, bacterial colonization of the eyelid margins leads to crust formation and hyperemia.
Viral conjunctivitis, typically caused by adenoviruses, manifests with conjunctival injection and serous exudate.
Distinguishing between these etiologies is essential for selecting appropriate diagnostic modalities and guiding evidence-based interventions for red and crusty eyes.
Many individuals experience chronic dry eyes which can exacerbate these symptoms, making it crucial to address underlying conditions that affect tear production and eyelid health.
Are Red and Crusty Eyes Ever Serious?
While most cases of red and crusty eyes are benign and self-limited, you should recognize clinical features that may indicate a more serious underlying pathology.
Serious symptoms can include significant pain, photophobia, decreased visual acuity, or copious purulent discharge. When you encounter these signs, consider potentially sight-threatening underlying conditions such as keratitis, scleritis, or orbital cellulitis.
Immunocompromised status, recent ocular trauma, or contact lens use can also increase risk for severe infections or complications.
Bilateral involvement with systemic symptoms—like fever or lymphadenopathy—may suggest a broader infectious or inflammatory process.
A thorough patient history and detailed ocular examination are vital for differentiating benign conjunctivitis from more serious etiologies.
Early identification of red-flag features guarantees prompt referral and prevents irreversible vision loss.
The composition of tears is crucial in maintaining eye health, and any disruption in the balance of aqueous, oil, and mucus layers can exacerbate eye conditions.
Quick Relief: What to Do Right Away
If you develop red and crusty eyes, initiate immediate supportive care to reduce discomfort and prevent further irritation.
First, remove contact lenses if you use them, as they can exacerbate symptoms.
Employ immediate solutions such as gently cleansing the eyelids with sterile saline or warm water and a clean, lint-free cloth to eliminate crusts and reduce microbial load.
Apply cool compresses for vasoconstriction and symptomatic relief.
Avoid rubbing your eyes, since mechanical trauma can worsen inflammation and spread pathogens.
Practice strict hand hygiene to limit cross-contamination.
These soothing techniques provide rapid symptomatic relief and minimize exposure to irritants or secondary infection.
Increased eye crust may signal underlying issues, and uncomfortable symptoms warrant a consultation with an eye doctor; bacterial pink eye requires antibiotic treatment and is contagious.
Monitor for worsening symptoms, such as vision changes or severe pain, and be prepared to seek prompt medical evaluation if clinical status deteriorates despite these initial interventions.
Do Over-the-Counter Eye Drops Really Work?
You’ll find that most over-the-counter eye drops contain lubricants, vasoconstrictors, or mild antihistamines aimed at symptom control. While these can temporarily reduce redness and irritation, they won’t address underlying infections or more serious ocular pathology. It’s essential to recognize when symptoms persist, as this signals the need for targeted medical evaluation rather than continued self-treatment. It’s also important to understand that tear film composition plays a crucial role in maintaining eye health, and disruptions in this balance can exacerbate dry eye symptoms.
Common Ingredients and Effects
Several active ingredients commonly found in over-the-counter (OTC) eye drops target symptoms like redness and crusting, but their clinical effectiveness varies depending on the underlying cause.
You’ll encounter vasoconstrictors (e.g., naphazoline) that reduce redness by narrowing conjunctival blood vessels, and lubricants such as carboxymethylcellulose or hypromellose that address discomfort from dryness and crusting.
Some OTC formulations also include natural ingredients like chamomile or hyaluronic acid, intended to promote soothing effects through anti-inflammatory or hydrating properties.
Evidence supports that lubricants can relieve mild irritation, while natural ingredients may reduce ocular surface inflammation in select cases.
Diagnostic differentiation is crucial—if the etiology is allergic conjunctivitis or mild environmental irritation, these agents often provide symptomatic relief.
However, always correlate treatment choice with clinical findings. Chronic dry eyes can lead to blepharitis and meibomian gland dysfunction, which may not be adequately addressed by OTC lubricants alone.
Limitations for Serious Conditions
Although over-the-counter eye drops can alleviate mild symptoms such as redness and irritation, they don’t address the underlying pathology of serious ocular conditions. If you’re experiencing persistent crustiness, vision changes, or pain, it’s essential to evaluate more extensive treatment options. Relying solely on OTC products may delay the diagnosis of conditions like bacterial conjunctivitis, uveitis, or keratitis, which require targeted therapeutic interventions. Clinical evaluation remains vital for differentiating benign irritation from pathologies needing prescription medications or procedural management. Severe dry eyes can lead to complications like blepharitis and corneal abrasions, necessitating timely diagnosis and treatment. Don’t ignore persistent or severe symptoms—timely intervention optimizes outcomes.
Effective Home Remedies for Red and Crusty Eyes
You can reduce ocular inflammation and remove discharge by applying a warm compress to your closed eyelids. Evidence supports gentle eyelid cleansing with a diluted, preservative-free solution to decrease microbial load and debris. These interventions target common etiologies such as blepharitis and bacterial conjunctivitis. It’s important to choose an effective eyelid cleanser, as hypochlorous acid solutions are known to be effective against microbial agents and are recommended for comprehensive blepharitis management.
Warm Compress Application
One common suggestion for alleviating red and crusty eyes involves the application of a warm compress; however, recent evidence doesn’t support its effectiveness for treating these specific symptoms. While warm compresses benefits are well documented for conditions like meibomian gland dysfunction or blepharitis, their utility in managing acute redness and crustiness due to infectious or allergic etiologies remains unsubstantiated. If you consider using this intervention, standard application techniques recommend placing a clean, warm (not hot) moist cloth over closed eyelids for five to ten minutes. Despite the widespread anecdotal endorsement, current clinical data indicate that a warm compress may not address the underlying pathophysiology of red and crusty eyes. For accurate diagnosis and targeted management, you should prioritize evidence-based interventions. It’s important to note that blepharitis symptoms, such as dry eyes and irritated eyelids, can worsen without appropriate treatment.
Gentle Eyelid Cleansing
Because red and crusty eyes frequently result from debris accumulation or microbial overgrowth along the eyelid margins, gentle eyelid cleansing remains a cornerstone of effective home management.
To optimize eyelid hygiene, you should use a sterile, lint-free pad moistened with warm water or a commercially prepared eyelid cleanser. Apply gentle massage to the eyelid margins in a horizontal motion, targeting the removal of crusts and biofilm without causing mechanical irritation.
Evidence suggests that regular eyelid cleansing, performed twice daily, considerably reduces bacterial load and mitigates inflammatory triggers associated with blepharitis and conjunctivitis. It is also important to consider the anti-inflammatory benefits of Omega-3 fatty acids, as they have been shown to help improve symptoms and reduce inflammation.
It’s crucial to avoid harsh soaps or vigorous scrubbing, as these may disrupt the delicate ocular surface. Consistent implementation of this technique supports symptom resolution and reduces recurrence rates in red and crusty eye presentations.
When Do You Need Prescription Treatments?
Occasionally, red and crusty eyes indicate more than mild irritation and require prescription treatments for effective management. If you experience persistent symptoms, significant discomfort, visual changes, or discharge suggestive of bacterial conjunctivitis or blepharitis, you’ll likely need prescription medications. An ophthalmologist or optometrist will conduct a thorough ocular examination, including slit-lamp biomicroscopy, to assess for underlying infection or inflammatory disorders. Evidence-based treatment options may include topical antibiotics for bacterial infections, corticosteroids for severe inflammation, or antiviral agents if herpetic keratitis is suspected. Additionally, a diagnosis of meibomian gland dysfunction could be made, which is a common cause of blepharitis and requires targeted treatment. Failure to respond to over-the-counter interventions signals the need for professional evaluation. Timely initiation of appropriate prescription treatments reduces the risk of complications, such as corneal involvement or chronic ocular surface disease, and optimizes your recovery and visual outcomes.
Allergy Solutions for Red and Crusty Eyes
If allergic conjunctivitis underlies your red and crusty eyes, targeted interventions are vital for rapid symptom relief and ocular surface protection.
First, recognize allergy symptoms such as itching, watery discharge, and eyelid swelling.
Start with non-pharmacological strategies: practice meticulous eye hygiene by gently cleansing eyelids and lashes to remove allergens and crusts. Avoid rubbing your eyes, since this exacerbates inflammation and worsens allergy symptoms.
Consider using preservative-free artificial tears to dilute and flush allergens from the ocular surface. For moderate symptoms, topical antihistamine or mast cell stabilizer drops offer evidence-based efficacy in reducing pruritus and redness.
Severe or refractory cases may necessitate short-term corticosteroid drops under ophthalmologic supervision.
Prompt identification and management of underlying allergens are imperative for minimizing recurrence and protecting long-term ocular health.
How to Prevent Red and Crusty Eyes in Daily Life
Although red and crusty eyes often signal underlying ocular surface disease, you can implement targeted preventive measures to reduce risk and maintain eye health. Evidence suggests that modifiable lifestyle adjustments and environmental factors play significant roles in ocular surface stability.
To minimize your risk, consider the following diagnostic-based strategies:
- Optimize environmental factors: Use humidifiers to counteract low-humidity environments, and limit direct exposure to air conditioning or heating vents, which can exacerbate tear film evaporation.
- Adopt lifestyle adjustments: Practice regular eyelid hygiene with warm compresses and gentle lid scrubs to reduce meibomian gland dysfunction and prevent blepharitis-related symptoms.
- Limit allergen and irritant exposure: Identify and minimize contact with common triggers such as pollen, dust, and digital eye strain, all of which contribute to ocular surface inflammation.
Implementing these measures improves long-term ocular surface health.
Get Rid Of Crusty Eyes – Treat Your Dry Eyes With TheraLife
Crusty Eyes Management with TheraLIfe All In One Dry Eye Starter Kit.
Add To Cart
Frequently Asked Questions
Can Contact Lenses Cause Red and Crusty Eyes?
Yes, contact lenses can cause red and crusty eyes, especially if you neglect proper contact lens hygiene.
Common eye irritation causes include protein buildup on lenses, bacterial contamination, and insufficient tear film. Poor hygiene practices increase the risk of conjunctivitis or blepharitis, both of which can present with redness and crusting.
If you experience these symptoms, promptly discontinue lens use and seek diagnostic evaluation to rule out infectious or allergic etiologies and receive appropriate management.
Are Red and Crusty Eyes Contagious?
Yes, red and crusty eyes can be contagious if they’re caused by eye infections like viral or bacterial conjunctivitis. These pathogens spread through direct contact or contaminated surfaces.
However, if your symptoms stem from allergy symptoms, they’re not contagious because they’re triggered by environmental allergens, not pathogens.
To determine the etiology, clinicians assess discharge characteristics, exposure history, and associated systemic findings, guiding appropriate management and infection control precautions for affected individuals.
Is It Safe to Wear Makeup With Red and Crusty Eyes?
You shouldn’t wear makeup when experiencing red and crusty eyes, as makeup safety is compromised by active eye irritation.
Applying cosmetics can introduce additional allergens or pathogens, exacerbating inflammation or masking underlying diagnostic signs.
Ophthalmologists recommend discontinuing all eye makeup until symptoms resolve and a definitive diagnosis is made.
Resuming makeup too soon may delay healing or increase the risk of reinfection, particularly if applicators or products are contaminated.
Always prioritize ocular surface health.
Can Pets Contribute to Red and Crusty Eyes?
Yes, pets can contribute to red and crusty eyes through exposure to pet allergens like dander, saliva, or fur, which can trigger allergic conjunctivitis.
Additionally, direct contact with pets may transmit bacteria or viruses, increasing your risk of developing eye infections.
If you notice persistent symptoms, it’s important to undergo a thorough diagnostic evaluation to distinguish between allergic and infectious etiologies, guiding appropriate management and minimizing further ocular irritation.
How Do I Clean Crust From My Eyelids Safely?
Don’t let crusty eyelids take over your life—prioritize eyelid hygiene using safe methods.
Start by washing your hands, then gently cleanse your eyelids with a sterile, preservative-free saline solution or a commercially available eyelid cleanser.
Use a clean cotton pad or swab, moving from the inner to outer canthus. Avoid vigorous rubbing to minimize epithelial damage.
Evidence shows daily eyelid hygiene reduces microbial load and improves ocular surface health.
Get Rid Of Crusty Eyes – Treat Your Dry Eyes With TheraLife
Crusty Eyes Management with TheraLIfe All In One Dry Eye Starter Kit.
Add To Cart
Conclusion
Use TheraLife’s comprehensive approach as your detective tool to solve the mystery of red and crusty eyes. Unlike any other company, TheraLife offers unique oral eye treatment care, effectively addressing conditions like conjunctivitis, allergies, and blepharitis. Their products are designed to restore ocular health and comfort by targeting the root causes of these issues. Incorporating preventive measures and timely interventions with TheraLife’s solutions ensures your eyes are ready to see the world clearly once more. For detailed insights and success stories, explore TheraLife’s resources and learn how their products can benefit you.
References
- Craig, J.P.; Nichols, K.K.; Akpek, E.K.; Caffery, B.; Dua, H.S.; Joo, C.-K.; Liu, Z.; Nelson, J.D.; Nichols, J.J.; Tsubota, K.; et al. TFOS DEWS II Definition and Classification Report. Ocul. Surf. 2017, 15, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Akowuah, P.K.; Kobia-Acquah, E. Prevalence of Dry Eye Disease in Africa: A Systematic Review and Meta-Analysis. Optom. Vis. Sci. 2020, 97, 1089. [Google Scholar] [CrossRef] [PubMed]
- Cai, Y.; Wei, J.; Zhou, J.; Zou, W. Prevalence and Incidence of Dry Eye Disease in Asia: A Systematic Review and Meta-Analysis. Ophthalmic Res. 2022, 65, 647–658. [Google Scholar] [CrossRef]
- McCann, P.; Abraham, A.G.; Mukhopadhyay, A.; Panagiotopoulou, K.; Chen, H.; Rittiphairoj, T.; Gregory, D.G.; Hauswirth, S.G.; Ifantides, C.; Qureshi, R.; et al. Prevalence and Incidence of Dry Eye and Meibomian Gland Dysfunction in the United States: A Systematic Review and Meta-Analysis. JAMA Ophthalmol. 2022, 140, 1181–1192. [Google Scholar] [CrossRef] [PubMed]
- Stapleton, F.; Alves, M.; Bunya, V.Y.; Jalbert, I.; Lekhanont, K.; Malet, F.; Na, K.-S.; Schaumberg, D.; Uchino, M.; Vehof, J.; et al. TFOS DEWS II Epidemiology Report. Ocul. Surf. 2017, 15, 334–365. [Google Scholar] [CrossRef] [PubMed]
- Papas, E.B. The Global Prevalence of Dry Eye Disease: A Bayesian View. Ophthalmic Physiol. Opt. 2021, 41, 1254–1266. [Google Scholar] [CrossRef] [PubMed]
- Benítez-del-Castillo, J.M.; Burgos-Blasco, B. Prevalence of Dry Eye Disease in Spain: A Population-Based Survey (PrevEOS). Ocul. Surf. 2025, 36, 126–133. [Google Scholar] [CrossRef]
- Zhang, Y.; Chen, H.; Wu, X. Prevalence and Risk Factors Associated with Dry Eye Syndrome among Senior High School Students in a County of Shandong Province, China. Ophthalmic Epidemiol. 2012, 19, 226–230. [Google Scholar] [CrossRef]
- Uchino, M.; Dogru, M.; Uchino, Y.; Fukagawa, K.; Shimmura, S.; Takebayashi, T.; Schaumberg, D.A.; Tsubota, K. Japan Ministry of Health Study on Prevalence of Dry Eye Disease Among Japanese High School Students. Am. J. Ophthalmol. 2008, 146, 925–929.e2. [Google Scholar] [CrossRef]
- Stapleton, F.; Velez, F.G.; Lau, C.; Wolffsohn, J.S. Dry Eye Disease in the Young: A Narrative Review. Ocul. Surf. 2024, 31, 11–20. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.S.; Wang, M.T.M.; Craig, J.P. Exploring the Asian Ethnic Predisposition to Dry Eye Disease in a Pediatric Population. Ocul. Surf. 2019, 17, 70–77. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.T.M.; Craig, J.P.; Vidal-Rohr, M.; Menduni, F.; Dhallu, S.; Ipek, T.; Acar, D.; Recchioni, A.; France, A.; Kingsnorth, A.; et al. Impact of Digital Screen Use and Lifestyle Factors on Dry Eye Disease in the Paediatric Population. Ocul. Surf. 2022, 24, 64–66. [Google Scholar] [CrossRef]
- Moon, J.H.; Kim, K.W.; Moon, N.J. Smartphone Use Is a Risk Factor for Pediatric Dry Eye Disease According to Region and Age: A Case Control Study. BMC Ophthalmol. 2016, 16, 188. [Google Scholar] [CrossRef] [PubMed]
- Ma, J.; Zhu, H.; Guo, W.; Li, R.; Shen, S.; Wang, Y.; Huang, D.; Zhang, X.; Fu, Z.; Zhao, A.; et al. Association of Different Digital Media Experiences with Paediatric Dry Eye in China: A Population-Based Study. BMJ Open 2022, 12, e062850. [Google Scholar] [CrossRef] [PubMed]
- Wolffsohn, J.S.; Wang, M.T.M.; Vidal-Rohr, M.; Menduni, F.; Dhallu, S.; Ipek, T.; Acar, D.; Recchioni, A.; France, A.; Kingsnorth, A.; et al. Demographic and Lifestyle Risk Factors of Dry Eye Disease Subtypes: A Cross-Sectional Study. Ocul. Surf. 2021, 21, 58–63. [Google Scholar] [CrossRef]
- Qian, L.; Wei, W. Identified Risk Factors for Dry Eye Syndrome: A Systematic Review and Meta-Analysis. PLoS ONE 2022, 17, e0271267. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.T.M.; Vidal-Rohr, M.; Muntz, A.; Diprose, W.K.; Ormonde, S.E.; Wolffsohn, J.S.; Craig, J.P. Systemic Risk Factors of Dry Eye Disease Subtypes: A New Zealand Cross-Sectional Study. Ocul. Surf. 2020, 18, 374–380. [Google Scholar] [CrossRef]
- Rolando, M.; Zierhut, M. The Ocular Surface and Tear Film and Their Dysfunction in Dry Eye Disease. Surv. Ophthalmol. 2001, 45, S203–S210. [Google Scholar] [CrossRef] [PubMed]
- Willcox, M.D.P.; Argüeso, P.; Georgiev, G.A.; Holopainen, J.M.; Laurie, G.W.; Millar, T.J.; Papas, E.B.; Rolland, J.P.; Schmidt, T.A.; Stahl, U.; et al. TFOS DEWS II Tear Film Report. Ocul. Surf. 2017, 15, 366–403. [Google Scholar] [CrossRef]
- Wolff, E. The Mucocutaneous Junction of the Lidmargin and the Distribution of the Tear Fluid. Trans. Ophthalmol. Soc. UK 1946, 66, 291–308. [Google Scholar]
- Bron, A.J.; De Paiva, C.S.; Chauhan, S.K.; Bonini, S.; Gabison, E.E.; Jain, S.; Knop, E.; Markoulli, M.; Ogawa, Y.; Perez, V.; et al. TFOS DEWS II Pathophysiology Report. Ocul. Surf. 2017, 15, 438–510. [Google Scholar] [CrossRef] [PubMed]