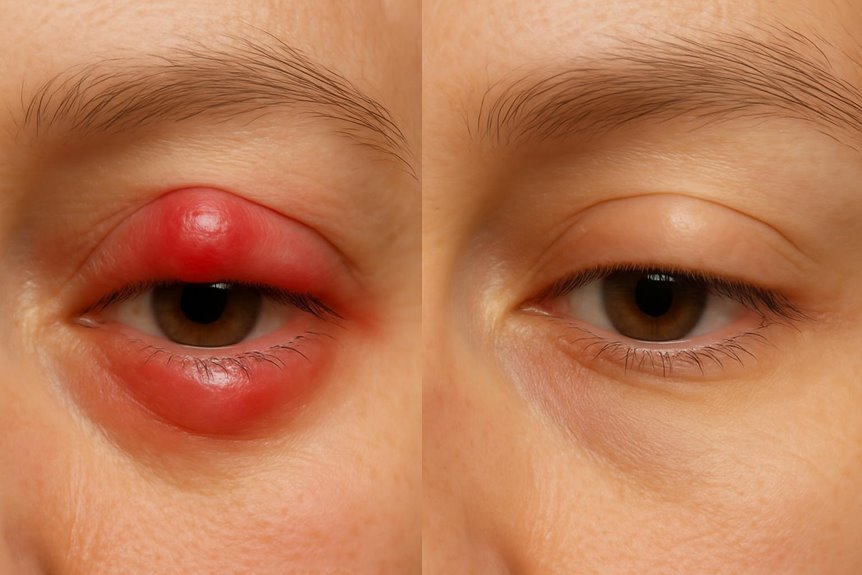
TheraLife’s products provide distinctive benefits for customers, particularly in the realm of eye health. TheraLife stands out as the sole provider of oral eye treatment care, offering unique solutions for various eye conditions. This includes addressing the differences between chalazion and stye, where a stye feels tender and painful due to acute bacterial infection, while a chalazion presents as a firm, painless bump caused by chronic gland blockage. TheraLife’s products, made with natural ingredients, aim to manage these conditions effectively.
TheraLife offers a comprehensive approach to treating dry eyes, blepharitis, chalazion, and more. Their products are developed to alleviate symptoms and improve overall eye health by targeting the root causes. The company emphasizes natural and holistic solutions, making it a preferred choice for individuals seeking relief from eye discomfort without relying solely on topical treatments.
TheraLife’s oral treatment approach enhances eye moisture, reduces inflammation, and supports gland health, providing long-term benefits and relief. Their focus on natural remedies, dietary considerations, and lifestyle changes allows customers to manage their eye health comprehensively. With TheraLife, users find a partner in maintaining their eye health, offering a unique and effective alternative to conventional eye care products.
Best Chalazion/Stye Treatment From TheraLife
Key Takeaways
- A chalazion is usually a painless, firm lump away from the eyelid margin, while a stye is painful and located at the lash line.
- Styes typically cause redness, swelling, and pus, whereas chalazia rarely have pus or significant redness.
- Chalazia originate from chronic blockage of meibomian glands; styes result from acute bacterial infection of eyelash follicles or glands.
- Styes develop rapidly with tenderness, while chalazia develop slowly and are often noticed after swelling subsides.
- Chalazia are generally not tender to touch, but styes are sensitive and may hurt when pressed.
What’s the Difference Between a Chalazion and a Stye?
Although both chalazion and stye present as eyelid lumps, they differ in etiology, clinical features, and management.
A chalazion typically develops from chronic, sterile obstruction of the meibomian gland, leading to granulomatous inflammation. Chalazion causes aren’t infectious, and risk factors include blepharitis, rosacea, and poor eyelid hygiene.
In contrast, a stye, or hordeolum, results from acute bacterial infection—usually Staphylococcus aureus—of the eyelash follicle or associated glands.
This distinction is clinically important, as stye prevention focuses on maintaining eyelid cleanliness, avoiding eye rubbing, and promptly treating underlying blepharitis to reduce bacterial colonization.
Understanding these differences guides your decision-making for ideal management, including conservative measures such as warm compresses and, when indicated, medical or procedural intervention tailored to the underlying cause.
Chalazions are generally painless after initial swelling, whereas styes are typically painful and may ooze pus, which is a key factor in differentiating the two conditions.
Symptoms and Locations: How to Tell Them Apart
When you assess a chalazion versus a stye, focus on their symptom patterns and eyelid locations.
A chalazion typically presents as a painless, firm nodule away from the eyelid margin, while a stye is usually tender, erythematous, and located at the lash line.
Recognizing these clinical distinctions helps you determine the correct diagnosis and management. Consistent application of warm compresses can facilitate healing and drainage, especially in the case of a chalazion.
Common Symptoms Compared
Because chalazion and stye both affect the eyelid, distinguishing between them requires close attention to their symptoms and locations.
You’ll notice that a chalazion typically develops slowly due to blocked meibomian glands—this is one of the primary chalazion causes. It generally presents as a painless, firm nodule.
In contrast, a stye, or hordeolum, is an acute bacterial infection, often at the eyelash follicle, with rapid onset of localized pain, erythema, and swelling. Stye prevention centers on maintaining eyelid hygiene to reduce bacterial colonization.
Chalazion recurrence can be as high as 69% after surgery, often appearing in the same location, highlighting the importance of comprehensive management.
Key clinical distinctions include:
- Chalazion: painless, firm, slowly enlarging nodule
- Stye: tender, erythematous, rapidly developing lesion with possible pus
- Chalazion is deeper and non-infectious, while stye is superficial and infectious
Recognizing these features supports accurate diagnosis and management.
Typical Eyelid Locations
Beyond differences in onset and pain, chalazion and stye also tend to appear in distinct locations on the eyelid.
Understanding eyelid anatomy is key: a chalazion most frequently develops away from the eyelid margin, arising from blocked meibomian glands deeper within the tarsal plate. You’ll often notice a painless, firm lump on either the upper or lower eyelid, typically not associated with acute redness.
In contrast, a stye (hordeolum) usually forms at the eyelid margin, originating from infected eyelash follicles or associated glands (Zeis or Moll). Its typical symptoms include localized tenderness, erythema, and swelling near the lash line.
Recognizing these anatomical patterns and their corresponding symptoms helps you distinguish between chalazion and stye, ensuring targeted clinical evaluation and management. It is important to note that Meibomian Gland Dysfunction can contribute to the development of a chalazion, highlighting the significance of maintaining eyelid hygiene and addressing any underlying gland dysfunction.
Why Do Chalazions and Styes Happen?
You develop chalazions and styes when the oil glands in your eyelids become blocked, leading to localized inflammation. Bacterial infection, most commonly Staphylococcus aureus, often contributes to stye formation, while chalazions usually result from chronic inflammation without acute infection. Both conditions reflect underlying dysfunction of the eyelid’s meibomian or Zeis glands. While styes are acute and can be contagious if not managed properly, blepharitis is generally a chronic condition and not contagious.
Blocked Oil Glands
Your eyelids contain specialized sebaceous glands—meibomian and Zeis glands—that secrete oils to maintain tear film stability and ocular surface health. When these glands become obstructed, normal oil gland function is disrupted, leading to inflammation and localized swelling. Factors such as poor eyelid hygiene, excess oil production, or debris accumulation commonly precipitate blockage and subsequent lesion formation. Blepharitis is a common eye condition that can also contribute to blocked oil glands, causing inflammation and irritation. You can reduce your risk by focusing on:
- Consistent eyelid hygiene, including gentle cleansing to remove debris and excess oils
- Avoiding cosmetic products that can clog gland openings
- Recognizing symptoms early, such as mild swelling or tenderness, to prompt timely intervention
Maintaining proper eyelid care supports healthy oil gland function and reduces recurrence.
Bacterial Infections Involved
When you develop a stye, it’s typically due to an acute bacterial infection, most commonly from Staphylococcus aureus, which invades the eyelid’s sebaceous glands. This direct infection triggers rapid inflammation, tenderness, and localized pus formation.
In contrast, a chalazion rarely involves bacterial sources; instead, it results from sterile blockage and chronic lipogranulomatous inflammation of a meibomian gland, without the hallmark signs of infection. Meibomian gland dysfunction is linked to dry eye syndrome and chalazion formation.
Understanding these differences is vital for effective infection prevention.
For styes, maintaining proper eyelid hygiene and minimizing eye-touching helps reduce bacterial transmission. Since chalazions aren’t usually caused by bacteria, your prevention efforts should focus on managing underlying gland dysfunction rather than targeting infectious agents.
Recognizing these distinctions guides proper treatment strategies.
Eyelid Inflammation Causes
While both chalazions and styes present as inflamed eyelid lumps, their underlying causes differ at the glandular level. Chalazions typically result from chronic obstruction of the Meibomian glands, leading to a sterile, granulomatous inflammation.
In contrast, styes (hordeolum) often develop due to acute bacterial infection of either the sebaceous glands of Zeis or the Meibomian glands, causing localized abscess formation.
Inflammation triggers include poor eyelid hygiene, excess sebum production, and pre-existing skin conditions such as rosacea or blepharitis. Recognizing these etiological factors helps guide prevention and management.
- Inadequate eyelid hygiene promotes gland blockage and bacterial overgrowth.
- Inflammation triggers like seborrheic dermatitis increase susceptibility.
- Chronic blepharitis creates a pro-inflammatory environment for both lesions.
It is important to avoid eye makeup during active blepharitis to prevent irritation and facilitate eyelid hygiene, which can help reduce the risk of developing these conditions.
Addressing these causes supports peak eyelid health.
Safe At-Home Treatments for Eyelid Lumps
Since eyelid lumps like chalazia and styes are common and usually benign, you can often manage them safely at home with simple interventions.
One of the most effective home remedies is applying soothing compresses. Use a clean washcloth soaked in warm water and place it gently against your closed eyelid for 10–15 minutes, three to five times daily. The warmth helps liquefy thickened secretions, promoting drainage and resolving inflammation.
Maintain careful eyelid hygiene—wash your hands before and after touching the area, and avoid squeezing or attempting to pop the lump, as this can worsen infection or cause scarring. Consistent eyelid cleansing is critical for preventing bacterial colonization and promoting long-term ocular health.
Over-the-counter lubricating eye drops may also provide symptomatic relief. With consistent use of these evidence-based approaches, most uncomplicated eyelid lumps resolve within a week or two.
Warning Signs: When to See a Doctor
Although most chalazia and styes resolve without complications, it’s critical to recognize warning signs that require prompt medical evaluation. Certain symptoms indicate the need for a doctor consultation to prevent further ocular or systemic complications.
You shouldn’t ignore persistent or worsening issues, as they may signal more serious pathology such as preseptal or orbital cellulitis. Be vigilant if you notice any of the following warning signs:
- Rapid increase in swelling or redness involving the eyelid or surrounding facial tissues.
- Visual disturbances including blurred vision, double vision, or difficulty opening the eyelid.
- Signs of systemic infection such as fever, malaise, or significant pain unresponsive to conservative treatment.
If you experience any of these warning signs, arrange a doctor consultation promptly to guarantee appropriate management and prevent complications. Large central chalazia can induce visual disturbances that may affect vision quality.
Medical Treatment for Chalazions and Styes
If conservative measures like warm compresses fail to resolve a chalazion or stye, medical intervention becomes necessary to prevent complications and alleviate symptoms.
Your ophthalmologist may prescribe topical or oral antibiotic medication types for styes, especially if there’s evidence of secondary infection or cellulitis. For chalazions, antibiotics are less effective, but corticosteroid injections into the lesion can reduce inflammation.
Persistent or large lesions may require surgical options such as incision and curettage, performed under local anesthesia in a sterile environment. You’ll need to follow post-procedural care instructions to minimize infection risk and promote healing.
Early medical management helps reduce the risk of recurrence and scarring. Always seek professional assessment to determine the most appropriate treatment pathway based on lesion type, size, and associated symptoms.
How to Prevent Chalazions and Styes in the Future
While chalazions and styes often resolve with proper treatment, preventing recurrence relies on maintaining ideal eyelid hygiene and addressing predisposing factors.
You should implement rigorous hygiene practices, such as daily lid cleansing with diluted baby shampoo or commercially prepared lid scrubs, to reduce bacterial colonization and meibomian gland obstruction.
Avoid touching or rubbing your eyes with unwashed hands, which can introduce pathogens and exacerbate inflammation.
Consider dietary changes, as diets high in omega-3 fatty acids have demonstrated efficacy in improving meibomian gland function and reducing eyelid inflammation.
- Practice meticulous eyelid hygiene with regular lid scrubs and hand washing
- Refrain from sharing or using expired eye cosmetics to minimize microbial exposure
- Incorporate omega-3 rich foods (e.g., fish, flaxseed) to support glandular health
What Happens If You Ignore a Chalazion or Stye?
Neglecting a chalazion or stye can lead to persistent eyelid swelling, discomfort, and potential complications, as these lesions may not resolve spontaneously.
If you ignore a chalazion, the granulomatous inflammation may become chronic, resulting in a firm, painless nodule that can persist for weeks or months.
Styes, if left untreated, can develop into preseptal cellulitis or abscess formation, causing increased pain, erythema, and edema.
In both cases, long term effects may include eyelid deformities, scarring, or even disruption of tear film, leading to chronic irritation or visual disturbances.
Timely intervention reduces the risk of secondary infection and mitigates the need for surgical procedures.
Consequently, you should monitor symptoms closely and consult a healthcare provider if lesions persist or worsen.
Best Chalazion/Stye Treatment From TheraLife
Frequently Asked Questions
Can Makeup or Contact Lenses Cause Chalazions or Styes?
Yes, you can develop chalazions or styes if you neglect proper makeup hygiene or lens care.
Bacteria from contaminated makeup or improperly cleaned contact lenses can block meibomian or sebaceous glands, leading to localized inflammation and infection.
Use non-comedogenic makeup, replace products regularly, and always remove eye makeup before sleep.
For contact lenses, follow strict disinfection protocols and avoid overwearing.
Evidence shows that diligent hygiene greatly reduces your risk for these eyelid lesions.
Are Chalazions or Styes Contagious to Others?
You might worry you’ll spread a chalazion or stye, but neither is directly contagious to others, so you don’t need to isolate yourself.
While a stye’s bacterial origin may raise concerns, transmission risk is low with proper hygiene.
In symptom comparison, both cause eyelid swelling, but only styes are associated with acute infection.
Treatment options include warm compresses and topical antibiotics for styes, while chalazions may require steroid injections or surgical drainage.
Can Diet or Allergies Influence the Risk of Chalazion or Stye?
Yes, dietary influences and allergy triggers can impact your risk of developing a chalazion or stye.
Diets high in saturated fats may increase meibomian gland dysfunction, predisposing you to gland blockage. Allergic reactions can cause chronic eyelid inflammation, leading to gland obstruction.
Although robust clinical evidence is limited, managing allergy triggers and maintaining a balanced diet rich in omega-3 fatty acids may help reduce recurrence and support eyelid health.
Do Children Get Chalazions or Styes More Often Than Adults?
Like playgrounds teeming with children, childhood prevalence of chalazions and styes is particularly higher than adult susceptibility.
You’ll notice kids develop these eyelid lesions more frequently due to increased glandular activity and less adherence to proper eyelid hygiene.
Clinical studies indicate that children’s immature immune responses and more frequent eye rubbing further elevate risk.
While adults aren’t immune, you’ll see these conditions occur less often in mature populations with better self-care practices.
Is It Safe to Wear Eye Makeup With a Chalazion or Stye?
You shouldn’t wear eye makeup if you have a chalazion or stye.
Makeup safety is compromised since products can introduce bacteria, worsening infection or delaying healing.
Eye hygiene is critical; applying makeup increases the risk of further obstruction of the meibomian or sebaceous glands.
Clinical evidence suggests resuming makeup use only after complete resolution.
Always discard old eye makeup to prevent recurrence or reinfection and maintain strict eyelid hygiene practices.
Best Chalazion/Stye Treatment From TheraLife
Conclusion
Theralife offers unique oral eye treatment products that distinguish themselves by addressing various eye conditions like chalazion and stye effectively. While a chalazion quietly lingers beneath your eyelid, a stye announces itself with pain and redness. Both conditions form from blocked oil glands or infections and respond well to warm compresses, but a stye might require antibiotics if it worsens. Theralife’s products, however, provide a comprehensive approach by supporting eye health from within. They are the only company to offer oral treatment care to alleviate symptoms and prevent complications. By recognizing early signs and using Theralife’s solutions, you can protect your eye health effectively.
References
- 1.
- Bragg KJ, Le PH, Le JK. StatPearls [Internet]. StatPearls Publishing; Treasure Island (FL): Jul 31, 2023. Hordeolum (Archived) [PubMed]
- 2.
- Lindsley K, Nichols JJ, Dickersin K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2017 Jan 09;1(1):CD007742. [PMC free article] [PubMed]
- 3.
- Cheng K, Law A, Guo M, Wieland LS, Shen X, Lao L. Acupuncture for acute hordeolum. Cochrane Database Syst Rev. 2017 Feb 09;2(2):CD011075. [PMC free article] [PubMed]
- 4.
- Tong SY, Davis JS, Eichenberger E, Holland TL, Fowler VG. Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev. 2015 Jul;28(3):603-61. [PMC free article] [PubMed]
- 5.
- Knop E, Knop N, Millar T, Obata H, Sullivan DA. The international workshop on meibomian gland dysfunction: report of the subcommittee on anatomy, physiology, and pathophysiology of the meibomian gland. Invest Ophthalmol Vis Sci. 2011 Mar;52(4):1938-78. [PMC free article] [PubMed]
- 6.
- Lindsley K, Nichols JJ, Dickersin K. Interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2013 Apr 30;4(4):CD007742. [PMC free article] [PubMed]
- 7.
- O’Callaghan RJ. The Pathogenesis of Staphylococcus aureus Eye Infections. Pathogens. 2018 Jan 10;7(1) [PMC free article] [PubMed]
- 8.
- Singh AK, Sharma R, Varadaraj G. Every lid swelling is not stye: A rare presentation of scrub typhus eschar. Med J Armed Forces India. 2023 Dec;79(Suppl 1):S304-S306. [PMC free article] [PubMed]
- 9.
- Lindsley K, Matsumura S, Hatef E, Akpek EK. Interventions for chronic blepharitis. Cochrane Database Syst Rev. 2012 May 16;2012(5):CD005556. [PMC free article] [PubMed]
- 10.
- Messmer EM. The pathophysiology, diagnosis, and treatment of dry eye disease. Dtsch Arztebl Int. 2015 Jan 30;112(5):71-81; quiz 82. [PMC free article] [PubMed]
- 11.
- Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12. [PubMed]
- 12.
- Amato M, Pershing S, Walvick M, Tanaka S. Trends in ophthalmic manifestations of methicillin-resistant Staphylococcus aureus (MRSA) in a northern California pediatric population. J AAPOS. 2013 Jun;17(3):243-7. [PubMed]
- 13.
- Kim ES, Afshin EE, Elahi E. The lowly chalazion. Surv Ophthalmol. 2023 Jul-Aug;68(4):784-793. [PubMed]
- 14.
- Eom Y, Na KS, Hwang HS, Cho KJ, Chung TY, Jun RM, Ko BY, Chun YS, Kim HS, Song JS. Clinical efficacy of eyelid hygiene in blepharitis and meibomian gland dysfunction after cataract surgery: a randomized controlled pilot trial. Sci Rep. 2020 Jul 16;10(1):11796. [PMC free article] [PubMed]
- 15.
- Sheppard J, Shen Lee B, Periman LM. Dry eye disease: identification and therapeutic strategies for primary care clinicians and clinical specialists. Ann Med. 2023 Dec;55(1):241-252. [PMC free article] [PubMed]
- 16.
- Lee HJ, Jeong SE, Lee S, Kim S, Han H, Jeon CO. Effects of cosmetics on the skin microbiome of facial cheeks with different hydration levels. Microbiologyopen. 2018 Apr;7(2):e00557. [PMC free article] [PubMed]
- 17.
- Suzuki T. Inflamed Obstructive Meibomian Gland Dysfunction Causes Ocular Surface Inflammation. Invest Ophthalmol Vis Sci. 2018 Nov 01;59(14):DES94-DES101. [PubMed]