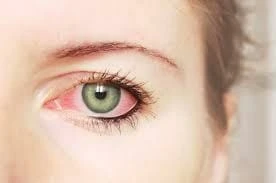
Why glaucoma result in dry eyes?Dry eye is one of the most common (if not the number one) unwanted side effects of eye drop glaucoma therapy. The topical medications can directly damage the ocular surface and/or the meibomian glands. This can be a complex side effect to manage in a person with a potentially progressive optic neuropathy from their glaucoma. With newer medication options on the market and an increasing number of less-invasive interventions, there are more tools now that we can utilize for those with glaucoma. It’s only in the last 10 years or so that the relationship between dry eye disease (DED) and glaucoma has been considered necessary. To learn more, click here. What is Dry Eye Disease (DED)DED affects millions of Americans. It has become one of the main reasons people see an eye doctor. They will often have burning or itching eyes that typically is associated with some form of dry eye. Glaucoma is a multi-faceted disease. Many of these glaucoma drops have preservatives in them that cause dry eye symptoms. , These glaucoma drops are made and compounded in different preparations. As a result, there is a lot of variability between the concentrations. The preservatives used and the variability can create toxic reactions that cause inflammatory mediators on the eye’s surface. The conjunctiva is typically a significant source of irritation from glaucoma drops and is bothered by inflammation. These drugs serve their purpose but, unfortunately, have unintended effects. So, while they lower the pressure, they cause secondary problems such as the dry eye. How to manage dry eyes and glaucomaAs dry eye has exploded, we’ve looked at how interrelated it is with glaucoma, and we’re determining how to combat this problem. Dry eye disease affects at least half of all people with glaucoma. Clogged oil glands ( MGD) are seen in upwards of 92% of people using prostaglandin analogs. This dry eye disease problem increases with each additional glaucoma drop. Therefore,, it is a genuine issue. Using multiple glaucoma drops can be disruptive to people due to the discomfort. People live longer, and they would never have known they had glaucoma. No less getting severe end-stage glaucoma using two, three, or even four eye drops. Some people are not surgical candidates. They won’t tolerate going under surgical therapy. Complicating things further is that our surgical treatment is not perfect. So we are forced into topical drop therapy. When Surgery Is Not an OptionThree topical glaucoma medications utterly free of preservatives are available in the United States: Zioptan (tafluprost ophthalmic solution 0.0015%; Akorn), Cosopt PF (dorzolamide-timolol ophthalmic solution 2%/0.5%; Akorn), and Timoptic in Ocudose (timolol maleate ophthalmic solution 0.25% and 0.5%; Valeant Pharmaceuticals). Regarding “friendlier” ocular surface options, BAK-free medications like Xelpros (latanoprost 0.005% ophthalmic emulsion, Sun Pharmaceuticals) can serve as an excellent alternative for preserved topical medications. Surgeries for GlaucomaSelective laser trabeculoplasty (SLT) is an in-office procedure that reduces intraocular pressure in patients with glaucoma. SLT is a first-line treatment in many facilities today. SLT is repeatable, and a micropulse CPC laser is an excellent option for non-true incisional therapy. Lastly, options for drops don’t have to be single therapy. Recently, OSRX came out with multiple treatment therapies with many different formulations placed in the same bottle. Their “AM Formula” has timolol, brimonidine tartrate, and dorzolamide, all in the same bottle. The “PM Formula” has all of that plus latanoprost. Imprimis Pharmaceuticals also has many formulations for patients desiring to not have multiple different bottles of medications at their homes. All of these therapies are great options, but some people simply need even better treatment plans. And this is when MIGS can take over. Combining MIGS and Cataract ProceduresWith the development of minimally invasive glaucoma surgery – minimally invasive glaucoma surgeries, or MIGS (MIGS), we’ve had what some people call a paradigm shift in glaucoma. We used to use as many drops as we could, but now we’ve shifted a bit to intervene at the time of cataract surgery. We can place a stent, strip some of the trabecular meshwork, or dilate the canals. Whatever we can try to get the outflow of the eye better to avoid so many topical therapies. If a person is on two or three drops, and you can do a MIGS procedure at the time of cataract surgery with no increase in the risk of the surgery., The issue with glaucoma and dry eye is that the topical therapy burden is the only non-surgical option to get the pressure down. Otherwise, it’s lasers, MIGS, and surgery. The majority of people are using drops, the first line. The drops lead to the cyclical process of the inflammatory cascade. A topical steroid to calm the inflammation down but will increase eye pressure. What we want to do is reduce toxicity by removing the drops. The sooner you can get off of multiple therapies, the quieter your eye will become. So even though glaucoma is the leading cause of their problem, or a cataract at the same time, the sooner we can get them off these glaucoma therapies, the better for the surface of the eye. It doesn’t really matter what we do for the dry eye; if we keep using toxic preserved medicines, it keeps causing the problem. To complicate things further, as people live longer, more people get glaucoma, and more people are also getting dry eyes because their eyes and their meibomian glands are drying up. It is a double-edged sword that’s very difficult to combat in our clinics. With a consistent message from ophthalmologists to their patients about reducing drop burden, we can overcome these two difficult pathologies. . Why TheraLife?Oral dry eye treatment from TheraLife help you restore and revive your own tear production naturally. No more drops To learn more
|
REFERENCES
- Schiffman RM, Walt JG, Jacobsen G, et al. Utility assessment among patients with dry eye disease. Ophthalmology2003; 110:1412–1419.
- Buchholz P, Steeds CS, Stern LS, et al. Utility assessment to measure the impact of dry eye disease. Ocul Surf2006; 4:155–161.
- Ayaki M, Kawashima M, Negishi K, Tsubota K. High prevalence of sleep and mood disorders in dry eye patients: survey of 1,000 eye clinic visitors. Neuropsychiatr Dis Treat2015; 11:889–894.
- Kitazawa M, Sakamoto C, Yoshimura M, et al. The relationship of dry eye disease with depression and anxiety: a naturalistic observational study. Transl Vis Sci Technol2018; 7:35.
- Zheng Y, Wu X, Lin X, Lin H. The prevalence of depression and depressive symptoms among eye disease patients: a systematic review and meta-analysis. Sci Rep2017; 7:46453Published 2017 Apr 12. doi:10.1038/srep46453.
- Ayaki M, Tsubota K, Kawashima M, et al. Sleep disorders are a prevalent and serious comorbidity in dry eye. Invest Ophthalmol Vis Sci2018; 59:DES143–DES150.
- Chan CC, Crowston JG, Tan R, et al. Ocular surface disease in patients with glaucoma from Australia. Asia Pac J Ophthalmol (Phila)2013; 2:79–87.
- Patel VD, Watanabe JH, Strauss JA, Dubey AT. Work productivity loss in patients with dry eye disease: an online survey. Curr Med Res Opin2011; 27:1041–1048.
- Bulat N, Cuşnir VV, Procopciuc V, et al. Diagnosing the dry eye syndrome in modern society and among patients with glaucoma: a prospective study. Rom J Ophthalmol2020; 64:35–42.
- Ruangvaravate N, Prabhasawat P, Vachirasakchai V, Tantimala R. High prevalence of ocular surface disease among glaucoma patients in Thailand. J Ocul Pharmacol Ther2018; 34:387–394.
- Saini M, Vanathi M, Dada T, et al. Ocular surface evaluation in eyes with chronic glaucoma on long term topical antiglaucoma therapy. Int J Ophthalmol2017; 10:931–938.
- DEWS II. The epidemiology of dry eye disease: report of the International Dry Eye Workshop (DEWS II). Ocul Surf2017; 15:334–365.
- Baudouin C. Detrimental effect of preservatives in eye drops: implications for the treatment of glaucoma. Acta Ophthalmol2008; 86:716–726.
- Pisella PJ, Pouliquen P, Baudouin C. Prevalence of ocular symptoms and signs with preserved and preservative free glaucoma medication. Br J Ophthalmol2002; 86:418–423.
- Leung EW, Medeiros FA, Weinreb RN. Prevalence of ocular surface disease in glaucoma patients. J Glaucoma2008; 17:350–355.
- Rossi GC, Tinelli C, Pasinetti GM, et al. Dry eye syndrome-related quality of life in glaucoma patients. Eur J Ophthalmol2009; 4:572–579.
- Fechtner RD, Godfrey DG, Budenz D, et al. Prevalence of ocular surface complaints in patients with glaucoma using topical intraocular pressure-lowering medications. Cornea2010; 29:618–621.
- Ramli N, Supramaniam G, Samsudin A, et al. Ocular surface disease in glaucoma: effect of polypharmacy and preservatives. Optom Vis Sci2015; 92:e222–e226.
- Kumar S, Singh T, Ichhpujani P, et al. Correlation of Ocular Surface Disease and Quality of Life in Indian Glaucoma Patients: BAC-preserved versus BAC-free Travoprost. Turk J Ophthalmol2020; 50:75–81.
- Paulsen AJ, Cruickshanks KJ, Fischer ME, et al. Dry eye in the beaver dam offspring study: prevalence, risk factors, and health-related quality of life. Am J Ophthalmol2014; 157:799e806.
- Rossi GC, Pasinetti GM, Scudeller L, Bianchi PE. Ocular surface disease and glaucoma: how to evaluate impact on quality of life. J Ocul Pharmacol Ther2013; 29:390–394.
- Enoch J, Jones L, Taylor DJ, et al. How do different lighting conditions affect the vision and quality of life of people with glaucoma? A systematic review. Eye2020; 34:138–154.
- Sagara H, Sekiryu T, Imaizumi K, et al. Impact of tear metrics on the reliability of perimetry in patients with dry eye. Plosone2019; 14:e0222467.
- Yenice O, Temel A, Orüm O. The effect of artificial tear administration on visual field testing in patients with glaucoma and dry eye. Eye (Lond)2007; 21:214–217.
- Özyol P, Özyol E, Karalezli A. Evaluation of visual field test parameters after artificial tear administration in patients with glaucoma and dry eye. Semin Ophthalmol2018; 33:320–324.
- Sun MJ, Rubin GS, Akpek EK, Ramulu PY. Impact of glaucoma and dry eye on text-based searching. Transl Vis Sci Technol2017; 6:24Published 2017 Jun 29. doi:10.1167/tvst.6.3.24.
- Nijm LM, Dunbar GE. Understanding the science behind the inflammatory cascade of dry eye disease. US Ophthalmic Review2019; 12:15–16. https://doi.org/10.17925/USOR.2019.12.1.15
- Mastropasqua R, Agnifili L, Mastropasqua L. Structural and molecular tear film changes in glaucoma. Curr Med Chem2019; 26:4225–4240.
- Roberti G, Tanga L, Manni G, et al. Tear film, conjunctival and corneal modifications induced by glaucoma treatment. Curr Med Chem2019; 26:4253–4261.
- Wong TT, Zhou L, Li J, et al. Proteomic profiling of inflammatory signaling molecules in the tears of patients on chronic glaucoma medication. Invest Ophthalmol Vis Sci2011; 52:7385–7391.
- Van Went C, Alalwani H, Brasnu E, et al. [Corneal sensitivity in patients treated medically for glaucoma or ocular hypertension]. J Fr Ophtalmol2011; 34:684–690.
- Martinez-de-la-Casa JM, Perez-Bartolome F, Urcelay E, et al. Tear cytokine profile of glaucoma patients treated with preservative-freeor preserved latanoprost. Ocul Surf 2017; 15:723–729.
- Agnifili L, Mastropasqua R, Fasanella V, et al. Meibomian gland features and conjunctival goblet cell density in glaucomatous patients controlled with prostaglandin/timolol fixed combinations: a case control, cross-sectional study. J Glaucoma2018; 27:364–370.
- Lee TH, Sung MS, Heo H, Park SW. Association between meibomian gland dysfunction and compliance of topical prostaglandin analogs in patients with normal tension glaucoma. PLoS One2018; 13:e0191398.
- Ha JY, Sung MS, Park SW. Effects of preservative on the meibomian gland in glaucoma patients treated with prostaglandin analogues. Chonnam Med J2019; 55:156–162.
- Uzunosmanoglu E, Mocan MC, Kocabeyoglu S, et al. Meibomian gland dysfunction in patients receiving long-term glaucoma medications. Cornea2016; 35:1112–1116.
- Russ HH, Nogueira-Filho PA, Barros Jde N, et al. Ocular surface evaluation in patients treated with a fixed combination of prostaglandin analogues with 0.5% timolol maleate topical monotherapy: a randomized clinical trial. Clinics (Sao Paulo)2013; 68:1318–1324.
- Benitez-Del-Castillo J, Cantu-Dibildox J, Sanz-Gonzalez SM, et al. Cytokine expression in tears of patients with glaucoma or dry eye disease: a prospective, observational cohort study. Eur J Ophthalmol2019; 29:437–443.
- Zhu W, Kong X, Xu J, Sun X. Effects of long-term antiglaucoma eye drops on conjunctival structures: an in vivo confocal microscopy study. J Ophthalmol2015; 2015:165475.
- Mastropasqua R, Agnifili L, Fasanella V, et al. In vivo distribution of corneal epithelial dendritic cells in patients with glaucoma. Invest Ophthalmol Vis Sci2016; 57:5996–6002.