To Stop Chalazion Is To Recognize The Root Cause- Dry Eyes
Treating Dry Eyes To Stop Chalazion Recurrence
New development of oral dry eye treatment that also stop chalazion recurrence.
This oral therapy protocol reduces inflammation caused by dry eyes, unclog meibomian oil glands and stop chalazion recurrence. To ready more customer stories, click here
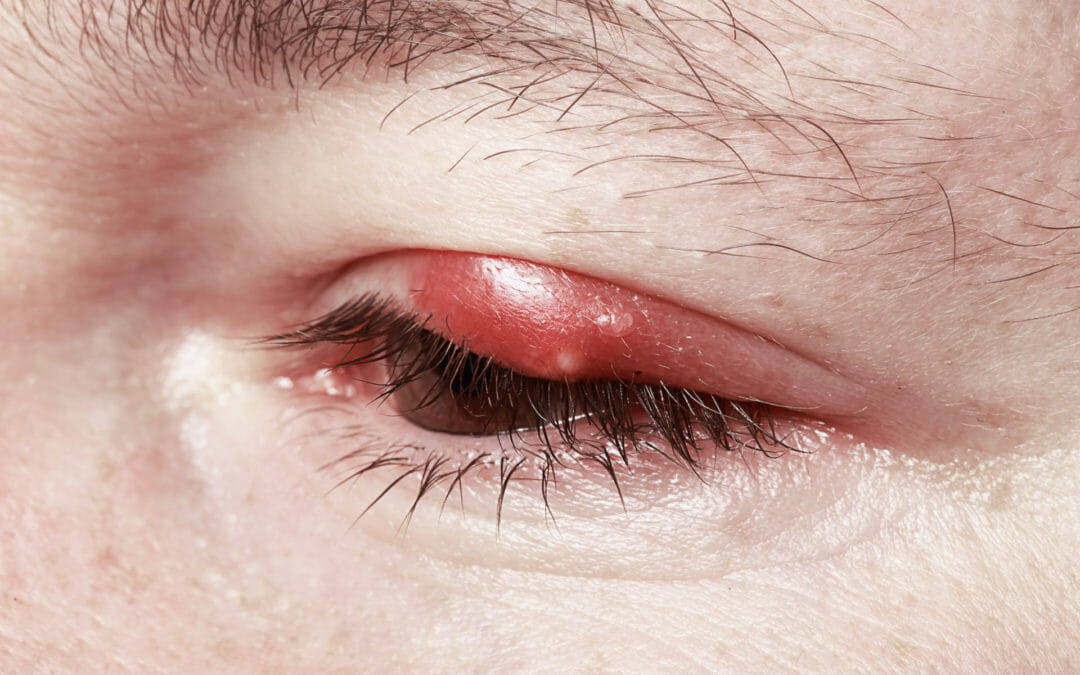
What is a Chalazion?
A chalazion is a small (2-8 mm) fluid-filled swelling (Eyelid Cyst) in the eyelid. It is common and sometimes called a meibomian cyst or tarsal cyst. It is more common on the upper eyelids. It is possible to have several at once, in more than one eyelid. It is not the same as a stye.
Plural of chalazion is chalazia.
A chalazion is caused by a blockage in one of the tiny meibomian oil gland of the upper or lower eyelid. The oil these glands produce helps moisten the eyes. Inflammation or viruses affecting the meibomian glands are the underlying causes of chalazia. Chalazia are more common in people with skin issues such as ocular rosacea and eczema.
Chalazion vs. stye
People sometimes confuse a chalazion with a stye due to similarities in appearance. Although people sometimes use the two terms interchangeably, they refer to different types of lesions that appear around the eye.
It results from a blocked oil gland, whereas a stye indicates an infected oil gland or hair follicle. There are two ways a stye can develop. An external hordeolum occurs at the base of the eyelash. An internal hordeolum develops deeper inside the eyelid. Both occur when oil glands become blocked.
A stye produces a red, swollen, painful lump on the edge or the inside of the eyelid and usually occurs closer to the surface of the eyelid than chalazion. If left untreated, a stye can result in the formation of it.
Chalazion and Dry Eyes
A chalazion may be associated with dry eye syndrome, which is often caused by meibomian gland dysfunction. People exhibiting certain risk factors are more likely to develop it. This includes people who have: Blepharitis, an inflammation of the eyelids.
Chalazion has to be seen as a part of a more generalized disease, not just the lump.
Hence, we treat the underlying cause with heating, massage and cleaning the eyelids, with or without lubricant eye drops, BlephEx and MiBo ThermoFlo, omega 3 supplements, and sometimes oral antibiotics.
Chalazion and dry eye can both be part of the same spectrum of Meibomian gland dysfunction.
Let us think “Dry eye – Chalazion – Posterior Blepharitis – Meibomian gland dysfunction” as all part of the same spectrum in young adults. This occurs especially for those who spend many hours on screen work each day.
While sitting hours in front of computer screens, concentrating on one fixed point and reading, our eyes blink less frequently. That is why especially young adults have the feeling of dry eyes in the evening. Sometimes external factors, like hot or cold weather, wind, dust or cigarette smoke also play a role in increasing the feeling of dry eyes.
What Causes a Chalazion?
A chalazion is caused by a blocked duct in one of the meibomian glands due to meibomian gland dysfunction (MGD). These glands are located in the eyelid directly behind the eyelashes. They produce a thin, oily fluid that lubricates the eye. It often develops following an internal hordeolum (also called a stye).
The meibomian glands in your upper and lower eyelids make oil that mixes with your tears to moisten and protect your eyes. If the oil gets too thick or if the glands are blocked because of inflammation, you may get it.
Chalazions often develop from an untreated stye. When the infection of the stye is left alone, the bacteria and debris can become a hard ball under the lid.
Causes & risk factors
Acne rosacea. Chronic blepharitis (inflammation of the eyelids, often from excess bacteria); Seborrhea; Tuberculosis; Viral infection; and diabetes. Rarely it is an indication of an infection or skin cancer.
Chalazia happen more often in adults than children.
What are the symptoms of a chalazion?
Symptoms of chalazia often develops following an internal hordeolum (also called a stye)
The primary sign of chalazia is a lump inside the upper eyelid. Less commonly, chalazia may develop inside the lower eyelid – accompanied by increased tearing. If chalazia progresses to the point of inflammation, it can cause the area around it to become red, swollen, blurred vision and pain or swelling of the whole eyelid.
Sometimes, the blocked gland causing the stye will not drain even though the redness and swelling go away. The gland will form a firm nodule in the eyelid.
Diagnosis
Necessary testing might include:
- Patient history to determine symptoms and the presence of any general health problems that may be contributing to the eye problem.
- External examination of the eye, including lid structure, skin texture and eyelash appearance.
- Evaluation of the lid margins, base of the eyelashes and oil gland openings using bright light and magnification.
Chalazia Treatment options
An eyelid cyst is a common reason why people seek advice from their GP or an ophthalmologist.
Chalazia often go away in days or weeks without treatment. But certain things might speed the process.
In most cases, you can treat it at home. Mostly it will go away in a month or less. First, never push on it or try to pop it. You can injure your eye . Instead, for home treatment, try: Warm compresses: Wet a clean washcloth with warm water. Hold it on the affected eye for 15 minutes. Do this at least three times a day
Medical treatment
See your doctor if you think you have a chalazion. They may want to check it and tell you how to take care of it to help it heal.
Your doctor may tell you to gently massage the lump a few times per day or to scrub your eyelid. They may also prescribe eye drops or eyelid creams. Medical treatment If it do not go away with home treatment, your doctor may recommend a corticosteroid injection or a surgical procedure to have it removed .
Warm compresses
Application of warm compresses to the affected eye may reduce hardened oil in the gland duct. It opens the drainage and filtration channels better and relieves irritation. Use warm compressed materials: Clean cloths for each compressed product — do not reuse the cloths.
Gently massage the area to help open the gland. But never try to squeeze or pop it. That might make the problem worse.
First treatment is to place warm compresses over the eyelid for 10 to 15 minutes at least four times a day. Use lukewarm water (no hotter than you can leave your hand in comfortably). This may soften the hardened oils blocking the duct, and lead to drainage and healing. DO NOT push or squeeze it. If the chalazion continues to get bigger, it may need to be removed with surgery.
Steroids
The inflammatory cells that comprise chalazia are steroid sensitive, which is why some research is considering intralesional steroid injection as a management option. Intralesional injection involves the injection of 0.1ml to 0.3ml of triamcinolone actetonide (5mg/ml to 40mg/ml) from a conjunctival approach. Like conservative therapies, no clear delineations as to the optimal amount and concentration of steroid exist. However, the success rates for this management modality is typically higher than for conservative therapy. A 2006 study saw a 94% cure rate (vs. 58% for conservative therapy) with intralesional injection of triamcinolone. Another investigations achieved an 80% success rate after two injections.
While intralesional injection of triamcinolone is generally safe, significant complications can occur. Skin depigmentation is a common occurrence following intralesional injection in dark-skinned patients. Also, inadvertent globe perforation is a possibility. Rarely, microembolization by steroid particles can result in retinal and choroidal infarction with subsequent permanent vision loss.
Surgery
If the chalazion continues to get bigger, it may need to be removed with surgery. This is most often done from the inside of the eyelid to avoid a scar on the skin. Steroid injection is another treatment option.
How to Prevent A Chalazion
The most effective way to prevent it is dry eye relieve. See TheraLife information above.
It’s not always possible to avoid getting a chalazion. This is especially true if you’re prone to this type of eye problem. However, there are a few things you can do to try to prevent this condition: Always wash your hands before touching your eyes. Make sure that anything that comes in contact – such as contact lenses and glasses , is clean. If you have a condition that increases your chance of developing it, follow your doctor’s instructions to help manage them.
Wash hands before touching around eyes or removing contact lenses. Wash face at bedtime to remove dirt and makeup. Remove eye makeup before going to bed and replace mascara, eyeliner and eye shadow every 3 months.
Eye Makeup
Don’t wear eye makeup while you have it. After it drains, keep the area clean. Follow good eye health practices, and avoid touching your eyes. If it doesn’t go away, you should seek help from an eye doctor. It may need to have the fluid drained through a small incision.
Are there any complications? Will it happen again?
Since the underlying root cause of it is meibomian gland dysfunction – a part of chronic dry eyes. What drives these eye problem is inflammation. Therefore, unless you relieve dry eyes and stop the inflammation, your chalazion or styes tends to recur.
To stop this recurrence, try treating your dry eyes with an oral dry eye treatment from TheraLife. Proven success in stopping recurrence.
Prognosis of a Chalazion
Chalazia typically heal on their own. The prognosis with treatment is excellent in most cases. Duration of a Chalazion – As long as there is no infection, a chalazion typically only lasts a few weeks provided it’s treated properly.
Support Group on Facebook
There is a support group on Facebook for anyone experiencing a chalazion, whether for the first time or as a recurring problem. Additional reporting by Becky Upham. Editorial Sources and Fact-Checking Chalazion. American Optometric Association . Hordeolum (Stye). American Optometric Association . How Tears Work. National Eye Institute . July 16, 2019.
Frequently Asked Questions
What happens if a chalazion is left untreated?
Chalazion happens often especially if you have dry eyes which result in clogged meibomian oil glands. Chalazion left untreated can become a very hard lump which may require surgery for removal.
What triggers chalazion?
The causes of a chalazion is a blocked meibomian oil gland located on your eyelids. These glands became clogged due to inflammation from chronic dry eyes. People with ocular rosacea, Seborrhea; Tuberculosis; Viral infection; and diabetes are more prone to chalazion.
How serious is a chalazion?
Most of the time, chalazia will go away on its own, with proper care. A stye – which is infectious left untreated can turn into a chalazion. If the chalazion do not go away in a few month, you might need surgery.
How long did it take for your chalazion to go away?
Typically, a chalazion will go away in a month or so. If it lasts a few month and turned into a hard lump, then surgery will be an option.
What is the best treatment for chalazion?
Best treatment for chalazion is a warm compress 3-4 times a day, followed by gentle massage. We also recommend that you clean your eyelids right after warm compress to remove debri from the melted cloggings of the oil glands.
We highly recommend treating dry eyes to prevent recurrence. For more information, click here.
Conclusion
A chalazion is a painless lump that can develop on the eyelid. Although chalazia can cause irritation and discomfort, they are usually harmless and clear up on their own within a few weeks.
Occasionally, a chalazion may become infected. See an eye doctor, an optometrist, or an ophthalmologist if the eye area becomes particularly swollen or painful or if the chalazion does not respond to home treatment.
References
Jin KW, Shin YJ, Hyon JY. Effects of chalazia on corneal astigmatism : Large-sized chalazia in middle upper eyelids compress the cornea and induce the corneal astigmatism. BMC Ophthalmol. 2017 Mar 31;17(1):36. – PMC – PubMed
Fukuoka S, Arita R, Shirakawa R, Morishige N. Changes in meibomian gland morphology and ocular higher-order aberrations in eyes with chalazion. Clin Ophthalmol. 2017;11:1031-1038. – PMC – PubMed
Mittal R, Tripathy D, Sharma S, Balne PK. Tuberculosis of eyelid presenting as a chalazion. Ophthalmology. 2013 May;120(5):1103.e1-4. – PubMed
Hanafi Y, Oubaaz A. [Leishmaniasis of the eyelid masquerading as a chalazion: Case report]. J Fr Ophtalmol. 2018 Jan;41(1):e31-e33. – PubMed
Wu AY, Gervasio KA, Gergoudis KN, Wei C, Oestreicher JH, Harvey JT. Conservative therapy for chalazia: is it really effective? Acta Ophthalmol. 2018 Jun;96(4):e503-e509. – PMC – PubMed