What are styes and chalazia?
Styes and chalazia are lumps in or along the edge of an eyelid. They may be painful or annoying, but they are rarely severe. When styes and chalazion become chronic, surgery is necessary to remove the scarred tissue.
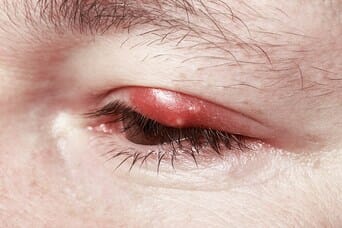
- A stye in the eyelid is an infection that causes a tender red lump on the eyelid. Most styes are along the edge of the eyelid. When a stye happens inside the eyelid, it is called an internal hordeolum.
- A chalazion is a lump in the eyelid. Chalazia (plural) may look like styes, but they are usually larger and may not hurt. A chalazion is not infectious where stye in the eyelid is.
Dry eyes and blepharitis cause Styes and chalazia because the meibomian oil glands on the eyelid become blocked or infected. At the center of this problem is inflammation of the eyelids.
What causes a stye or chalazion?
Stye
A bacterial infection causes styes in the eyelid. The bacteria grow in the root of an eyelash. An infection in one of the tiny meibomian oil glands inside the eyelid results in an internal hordeolum. Meibomian oil glands secrete lubricants that thicken the tear, making your eyes comfortable.
A chalazion happens when an oil gland in the eyelid becomes blocked. If an internal hordeolum doesn’t drain and heal, it can turn into a chalazion.
Symptoms of a stye or chalazion
A stye starts as a red bump that looks like a pimple along the edge of the eyelid.
- A very painful red bump along the edge of the eyelid at the base of the eyelashes. It may make the entire eyelid swell
- usually a tiny pus spot at the center of the bump
- foreign body sensation in the eye
- eyes sensitive to light
- blepharitis – crustiness along the eyelid margin
- Watery eyes
- Most styes grow bigger for about three days before they break open and drain.
- Styes usually heal in about a week.
A chalazion starts as a firm lump under the skin of the eyelid.
- Chalazia often don’t hurt.
- Chalazia grow more slowly than styes. If a chalazion gets large enough, it may affect your vision.
- The inflammation and swelling may spread to the eyelids above the eyelashes.
- Chalazia often go away in a few months without treatment.
- A bump on the eyelid, sometimes becoming red and swollen. Occasionally it can be tender.
- rarely, an entirely swollen eyelid
- If the chalazion is large enough to press on the eyeball, you get blurry vision
Both styes and chalazion can become recurrent due to chronic dry eyes. TheraLife can help.
How is a stye or chalazion diagnosed?
Eye doctors diagnose styes or chalazion by examining the eyelid. It may be hard to tell the difference between a stye and a chalazion. If there is a hard lump inside the eyelid is mainly diagnosed as a chalazion.
How are styes and chalazion treated?
Warm compresses
Use a warm gel compress, heat it in the microwave oven and hold it to your eyelid for 10–15 minutes at a time, 3–5 times a day. For a chalazion, this warm compress helps the clogged meibomian oil gland to open and drain. Gentle massage with a clean finger can help the gland open and clear by itself.
Antibiotics
Your eye doctor will prescribe an antibiotic gel or drop for an infected stye.
Steroid shots
Your eye doctor may give you a steroid shot (cortisone) to reduce the swelling if you have a swollen chalazion.
How can Theralife help?
TheraLife treats recurring styes or chalazia from the root cause – chronic dry eyes. TheraLife has a comprehensive protocol to treat dry eyes, blepharitis, and clogged meibomian oil glands (MGD) simultaneously to get this condition under control.
Surgery for drainage
If your stye or chalazion affects vision or does not go away, you may need to have it surgically drained. The eye doctor performs this surgery in the doctor’s office under local anesthesia.
If a stye or chalazion is recurring, it is primarily due to chronic dry eyes and continuous inflammation. TheraLife can get dry eyes under control using the oral treatment and stop stye or chalazion recurrence.
Do not squeeze or try to pop a stye or chalazion.
Doing so could spread the infection into your eyelid. Do not wear eye makeup or contact lenses while you have a stye or chalazion.
How can you prevent styes and chalazia?
- Don’t rub your eyes. Rubbing your eyes can irritate your eyes and let in bacteria. If you must touch your eyes, clean your hands first.
- Protect your eyes from dust and air pollution. For example, wear safety glasses when you do dusty chores like raking or mowing the lawn.
- Replace eye makeup, especially mascara, at least every six months. Bacteria can grow in makeup.
- If you get styes or chalazia often, wash your eyelids regularly with an eyelid cleanser like Avenova.
- Treat any inflammation or infection of the eyelid right away.
Who Is at Risk for Chalazia and Styes?
Anyone can get a stye or chalazion. But you are even more likely to get one if you have:
- Blepharitis, a problem that affects the edge of your eyelid
- Had a stye or chalazion before
- A skin condition, such as acne rosacea or seborrheic dermatitis
- Diabetes or other medical problems
References
- Berufsverband der Augenärzte Deutschlands (BVA), Deutsche Ophthalmologische Gesellschaft (DOG). Leitlinie Nr. 10: Hordeolum / Chalazion. August 2011.
- Burk A, Burk R. Checkliste Augenheilkunde. Stuttgart: Thieme; 2017.
- Cheng K, Law A, Guo M, Wieland LS, Shen X, Lao L. Acupuncture for acute hordeolum. Cochrane Database Syst Rev 2017; (2): CD011075.
- Lindsley K, Nichols JJ, Dickersin K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst Rev 2017; (1): CD007742.
- Klinisches Wörterbuch. Berlin: De Gruyter; 2017.
- Bragg KJ, Le PH, Le JK. StatPearls [Internet]. StatPearls Publishing; Treasure Island (FL): Mar 23, 2021. Hordeolum.
- Lindsley K, Nichols JJ, Dickersin K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2017 Jan 09;1:CD007742.
- Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12.
- Amato M, Pershing S, Walvick M, Tanaka S. Trends in ophthalmic manifestations of methicillin-resistant Staphylococcus aureus (MRSA) in a northern California pediatric population. J AAPOS. 2013 Jun;17(3):243-7.
- Moriya K, Shimizu H, Handa S, Sasaki T, Sasaki Y, Takahashi H, Nakamura S, Yoshida H, Kato Y. Incidence of Ophthalmic Disorders in Patients Treated with the Antineoplastic Agent S-1. Gan To Kagaku Ryoho. 2017 Jun;44(6):501-506.
- Ansari AS, de Lusignan S, Hinton W, Munro N, McGovern A. The association between diabetes, level of glycaemic control and eye infection: Cohort database study. Prim Care Diabetes. 2017 Oct;11(5):421-429.
- Pflipsen M, Massaquoi M, Wolf S. Evaluation of the Painful Eye. Am Fam Physician. 2016 Jun 15;93(12):991-8.
- John AM, John ES, Hansberry DR, Thomas PJ, Guo S. Analysis of online patient education materials in pediatric ophthalmology. J AAPOS. 2015 Oct;19(5):430-4.
- Machalińska A, Zakrzewska A, Safranow K, Wiszniewska B, Machaliński B. Risk Factors and Symptoms of Meibomian Gland Loss in a Healthy Population. J Ophthalmol. 2016;2016:7526120.
- Hirunwiwatkul P, Wachirasereechai K. Effectiveness of combined antibiotic ophthalmic solution in the treatment of hordeolum after incision and curettage: a randomized, placebo-controlled trial: a pilot study. J Med Assoc Thai. 2005 May;88(5):647-50.