A chalazion is an oil gland in the eyelid that becomes blocked which is a common issue in people with dry eyes. Dry eyes cause blepharitis and clogged oil glands called meibomian gland dysfunction(MGD). Treating dry eyes, blepharitis, and MGD with TheraLife will stop the recurrence of chalazion.
Definition?
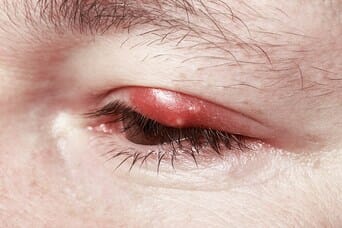
A chalazion, also known as a meibomian cyst, is a fluid-filled bump on the upper or lower eyelid. It should disappear over time. Surgery may be necessary if there is scar tissue.
Chalazia (plural of chalazion) is sometimes confused with styes.
A chalazion is a firm, painless lump that develops within the eyelid when an oil gland becomes obstructed or blocked. A stye is an abscess of the eyelid. It typically occurs when an oil gland at the edge of the eyelid becomes infected with bacteria or mites, resulting in a pus-filled lump or pimple that can hurt.
Signs and Symptoms
The primary sign is a lump inside the upper eyelid.
Less commonly, chalazia may develop inside the lower eyelid. It can cause increased tearing.
Suppose it progresses to the point of inflammation. In that case, it can cause the area around it to become red, swollen, and painful. ,
Causes ?
Clogged Meibomian glands cause chalazion. Meibomian glands are on the eyelids near the lashes. They produce a thin, oily lubricant that prevents evaporation of the tear and protects the cornea.
Inside the oil in the meibomian gland becomes thick and forms a bump. Research shows that the cholesterol in your blood is related to the thickness of your meibomian oils.
Both chalazia and stye are often a complication of blepharitis, a chronic inflammation of the eyelids. Blepharitis can be caused either by bacteria or mites (Demodex). Acne rosacea can cause meibomian gland secretions to become unusually thick and develop into a chalazion.
Risk factors
The following conditions or factors are associated with an increased risk : (5)
- A prior chalazion
- Demodicosis (demodex mite infestation)
- Low vitamin A levels in the blood
- Gastrointestinal inflammation
- Smoking
Diagnoses
Diagnosis involves a comprehensive eye exam. Your eye doctor will start by obtaining your medical history, symptoms, and any health problems that could lead to your eyelid issues.
Your doctor will then examine your eyes, looking at your eyelid structure, skin texture, and the appearance of your eyelashes. Your doctor can take a sample of your eyelashes, look under the microscope and see if bacteria or mites are present. Usually, this is enough information to make a clinical diagnosis, though rarely will the doctor obtain a fluid sample for lab testing.
Prognosis
Chalazia typically heal on their own. The prognosis with treatment is excellent in most cases. If there are still scar tissues left after healing, surgery may be necessary.
Duration
As long as there is no infection, typically duration only lasts a few weeks, especially when the treatment is appropriate.
To help the cysts heal, doctors recommend applying warm compresses to the affected eyelid for 10 to 15 minutes, 3 to 5 times a day, followed by eyelid cleansing. “The warm compresses melt the oil and allow it to drain through.
You can also try to help drain by gently massaging the eyelid for several minutes a day, but never try to push, squeeze, or “pop” the cyst.
A warm compress is helpful, but chalazion will recur if dry eyes persist.
Medication Options
Doctors do not typically treat with systemic medication, like oral antibiotics. But sometimes, can prompt an inflammatory reaction or become infected. Depending on the diagnosis, we will treat it with a topical steroid or antibiotic or an antibiotic/steroid combination ointment or drops.
Alternative and Complementary Therapies
The best treatment fis a clean, warm, moist hot compress placed over the closed eyes a few times a day. Some people use warm tea bags.
Treatment Protocol from TheraLife
Theralite developed a protocol to treat recurring chalazion by treating dry eyes, blepharitis, and MGD simultaneously and getting to the root cause of chalazion, which is blocked oil glands.
Prevention
Good hygiene can help reduce your chances,
- Wash your hands often, especially before touching your face and eyes.
- If you wear contact lenses, wash your hands before and after removing them. Follow the recommended procedures for cleaning your lenses. If you wear daily- or weekly-use lenses, discard them on the schedule recommended by your eye doctor.
- Wash your face every night before bed.
- Throw away old makeup and replace eye makeup every 2 to 3 months. Don’t share or use another person’s eye makeup.
Complications of
If a chalazion doesn’t drain on its own after treatment with compresses, sometimes an incision is made to drain the bump and let the thickened oil come out.
A doctor should evaluate if it doesn’t go away within a few weeks. Possibilities of the correct treatment and ensure that the bump isn’t something else. Not all lumps on the eyelid are the same, so it’s essential to make sure that it’s not another type of nodule.
A chalazion that becomes very large can cause blurred vision if it presses against the eyeball.
How Common Are Chalazia and Who Tends to Get Them?
Chalazia are the most prevalent type of inflammatory lesions of the eyelid. They account for approximately 13 percent of all benign (not cancerous) lid lesions. Adults are more likely to develop a chalazion than children are, with these cysts occurring most frequently in people between the ages of 30 and 50.
Related Conditions that can cause Chalazia
A stye (hordeolum) is an acute bacterial infection of the oil gland. “That’s different from a chalazion, which is more of a sterile inflammation of the gland and not an infection,”
Blepharitis is a type of eyelid inflammation that usually affects both eyes along the edges of the eyelids. It often occurs when the tiny oil glands near the base of the eyelashes become clogged. The irritation and redness caused by blepharitis can be painful. Still, it doesn’t cause permanent damage to eyesight, and it’s not contagious.
Call and talk to a doctor toll-free 1-877-917-1989. Send email to [email protected]
References
1.Jin KW, Shin YJ, Hyon JY. Effects of chalazia on corneal astigmatism : Large-sized chalazia in middle upper eyelids compress the cornea and induce the corneal astigmatism. BMC Ophthalmol. 2017 Mar 31;17(1):36.
2.Fukuoka S, Arita R, Shirakawa R, Morishige N. Changes in meibomian gland morphology and ocular higher-order aberrations in eyes with chalazion. Clin Ophthalmol. 2017;11:1031-1038. [
3.Mittal R, Tripathy D, Sharma S, Balne PK. Tuberculosis of eyelid presenting as a chalazion. Ophthalmology. 2013 May;120(5):1103.e1-4.
4.Hanafi Y, Oubaaz A. [Leishmaniasis of the eyelid masquerading as a chalazion: Case report]. J Fr Ophtalmol. 2018 Jan;41(1):e31-e33.
5.Wu AY, Gervasio KA, Gergoudis KN, Wei C, Oestreicher JH, Harvey JT. Conservative therapy for chalazia: is it really effective? Acta Ophthalmol. 2018 Jun;96(4):e503-e509.
6.Chang M, Park J, Kyung SE. Extratarsal presentation of chalazion. Int Ophthalmol. 2017 Dec;37(6):1365-1367.
7.Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12.
8.Ozer PA, Gurkan A, Kurtul BE, Kabatas EU, Beken S. Comparative Clinical Outcomes of Pediatric Patients Presenting With Eyelid Nodules of Idiopathic Facial Aseptic Granuloma, Hordeola, and Chalazia. J Pediatr Ophthalmol Strabismus. 2016 Jul 01;53(4):206-11.
9.Aycinena AR, Achiron A, Paul M, Burgansky-Eliash Z. Incision and Curettage Versus Steroid Injection for the Treatment of Chalazia: A Meta-Analysis. Ophthalmic Plast Reconstr Surg. 2016 May-Jun;32(3):220-4.
10.Park YM, Lee JS. The effects of chalazion excision on corneal surface aberrations. Cont Lens Anterior Eye. 2014 Oct;37(5):342-5.
11.Arbabi EM, Kelly RJ, Carrim ZI. Chalazion. BMJ. 2010 Aug 10;341:c4044.
12.Görsch I, Loth C, Haritoglou C. [Chalazion – diagnosis and therapy]. MMW Fortschr Med. 2016 Jun 23;158(12):52-5. [