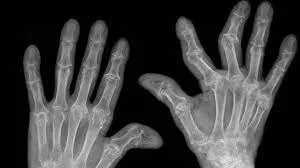
Long term effects of rheumatoid arthritis
According to Arthritis Foundation, about 1.5 million U.S. people live with R.A.
The exact cause of R.A. is not known. R.A. is an autoimmune disorder.
Rheumatism is a chronic inflammation of joints that causes joint pain, stiffness, swelling, and pain. Rheumatism is a systemic disease that involves all parts of the system and can cause significant organ problems. Fortunately, rheumatism does not cause rheumatism or other symptoms on the eyelids. The Sooner you start your medication, the higher your chances of fighting joint and bone disease and improving your health.
Inflammation
This chronic inflammatory autoimmune disease mistakenly causes your body to attack healthy joints and leads to widespread inflammation.
Heart problems. RA can increase your risk of hardened and blocked arteries and inflammation of the sac that encloses your heart. If R.A. affects your wrists, the inflammation can compress the nerve that serves most of your hand and fingers.
A rare but severe complication of R.A. is inflammation of the blood vessels ( rheumatoid vasculitis, or R.A. rash). Inflamed blood vessels weaken and expand or narrow, interfering with blood flow, leading to nerves, skin, heart, and brain problems.
Widespread inflammation
Rheumatoid arthritis is an inflammatory condition that can cause inflammation to other body parts, such as the: lungs – or lung lining, leading to pleurisy or pulmonary fibrosis. Pulmonary fibrosis can cause chest pain, a persistent cough, and shortness of breath: heart – inflammation of the tissue around the heart.
A rheumatologist is a doctor who specializes in arthritis and rheumatic diseases.
Bone loss
The autoimmune disease may also cause bone loss, and so can some medications, like steroids.
Protect Yourself From RA Complications:
Mention problems like depression, chest pain, joint pain or dry eyes to the doctor who treats your rheumatoid arthritis.
All these problems can be related to the disease. You might need different doctors and different treatments to control your R.A.
To learn more: National Institute of Arthritis and Musculoskeletal and Skin Diseases. Accessed February 9, 2021. https://www.niams.nih.gov/Health_Info/Rheumatic_Disease/default.asp.
Immune system
Your immune system is a complex structure composed of various tissues that work together in battling an infection. However, it can attack the joints, causing a problem.
R.A. can result from your body attacking healthy joints as it thinks it has invaded them.
R.A. can cause infection in many different ways.
Observational research shows that people suffering from R.A. infections are more likely than other people to die.
Taking drugs that reduce autoimmune diseases can also raise your risk of infection if they suppress your immune response.
Nervous system
R.A. affects the spinal cord and nervous system.
The 2015 review published in the journal Autoimmunity Reviews found that neurological symptoms in R.A. are widespread.
There are depression, cognitive disorders, behavior changes, spinal cord compression, and peripheral nerve damage.
The most likely causes of R.A. are nerve compression, pain, and inflammation.
Digestive System
Some RA. patients have gastrointestinal symptoms or gastrointestinal disorders.
Researchers showed that people with ra suffer more from G.I. issues than normal people.
R.A. had 70% more chance for lower G.I. problems than those without R.A. Upper GGI events include gastrointestinal ailments caused by perforations of the gastrointestinal tract.
Mucous membranes
Several tracts in the human body line the mucus membranes.
The mucus membrane includes the throat, nose, eyelid, airway, lung, stomach, intestines, and vagina.
Some people with ra develop Sjogren syndrome, which affects their mucosa.
Sjogren’s affect about 3.3 million adults in the United States which is the secondary to primary causes of R.A., the syndrome has the name Secondary Sjogrens syndrome.
A study in 2020 found that the prevalence of secondary Sjogrens in R.A. sufferers was approximately 40%. People with Sjogren’s has dry eyes, dry mouth, dry nasal passages, oral infections, swollen glands in addition to ra symptoms. Chronic dry mouth causes tooth decay.
Musculoskeletal System
Skeletal System.
Your musculoskeletal system provides movement and support.
The human body has two systems: the muscular and the skeletal systems.
Generally, skeletal systems include bone. The bones join at the joint and provide stability to the skeleton. Critical structural components surround the bones and joints, such as bone and muscle. Articular cartilage is white tissue covering bones’ ends at their intersection and joints.
In most cases, people with ra have symptoms occur in the same joints on both sides of your body.
About 40% of people with ra also experience signs and symptoms that don’t involve the joints.
Typically, the bone tissue that’s broken down gets replaced.
Still, as we age, the resorption rate exceeds the rate of new bone growth, reducing bone mass and setting the stage for osteoporosis.
R.A. makes it harder for bones to keep pace. The hip, forearm, and pelvis are specific sites where breaks can occur, although breaks are more likely near the joints where the R.A. is active.
Your mouth
Research reveals that people with RA may be more susceptible to developing periodontitis.
If you have a dry mouth, making it possible to create tooth loss.
Poor oral hygiene may contribute to a worsening RA. and losing teeth.
Inflammation in the mouth could trigger the body to make anti-inflammatory recombinations to the disease making it worse.
Eyes:
People with ra results in dry eye syndrome or episcleritis due to inflammation around the retina.
Your eye is composed of a central ocular system. It also causes eye problems like scleritis, keratoconjunctivitis, and uveitis.
Scleritis is an eye condition that causes deep sclerosis to develop. Untreated, sclerosis may result in vision loss—uveitis caused by inflamed eyelids- resulting in floaters, blurred vision, or pain.
Learn how TheraLife can help you relieve RA dry eyes
Blood vessels
Inflammation of the blood vessels, known as vasculitis, is the thickening, weakening, narrowing, and scarring of blood vessel walls. It can affect blood flow to your body’s organs and tissues and be life-threatening in severe cases.
Kidney Function
You need to avoid overdosing on nonsteroidal anti-inflammatory pain relievers (NSAIDs) for kidney health. For screening for Amyloidosis, a doctor can monitor the kidneys regularly for several reasons. Abnormal kidney function caused by the abnormal accumulation in protein -often associated with R.A. The symptoms could be mild, like pain or swelling or a weakened stomach or digestive problems.
Hands and feet
Up to 20% of people with RA develop rheumatoid nodules near the joints and pressure points.
Since R.A. affects a joint, it also affects the hands and feet.
A few symptoms affecting hand muscles include lock joints; ulnar drift; weakening of tendons & muscles, which can turn fingers towards pinkies;
Swan necks. This effect may hinder basic life tasks like completing a letter, lifting objects, or unwrapping lids.
R.A. can lead to further damage if DMARDs are not used early.
The inflammation can be so severe that it affects how the joints and other parts of the body look and function.
On the hand, R.A. may cause deformities in the fingers’ joints, making moving your hands difficult.
Lumps may form anywhere in the body. These are small, firm bumps caused by inflammatory tissue. These problems sometimes need to be treated with surgery to prevent loss of function in the affected joints.
Chronic inflammation of the wrists can lead to carpal tunnel syndrome, making it difficult to use your wrists and hands. Weakened or damaged bones in the neck or cervical spine can cause chronic pain.
If rheumatoid arthritis affects your wrists, the inflammation can compress the nerve that serves most of your hand and fingers resulting in carpal tunnel syndrome.
Brain and mood.
The fears associated with surviving a chronic illness like rheumatoid arthritis ra, the difficulty of everyday pain or mobility can affect emotional health.
Your Heart?
The risk of rheumatic arthritis increases if the patient has a heart attack or stroke.
The risk of a cardiovascular system heart attack is double in people with a systemically inflammatory disease like R.A.
Skin
Rashes, Ulcers, and Bumps:
Scaly skin and ulceration are common among patients with rheumatism.
Some 30 percent of R.A. patients develop inflammation-causing rheumatoid nodules in their skin near joints. Usually found in elbows, hands, and feet, Treat RA by intravenous injection. All skin ailments can be managed using DMARD.
When RA-related inflammation of the blood vessels (called vasculitis) affects the skin, a rash of small red dots is the result. Vasculitis can cause skin ulcers on the legs or under the nails in more severe cases.
Circulatory system
R.A. can trigger anemia and fatigue
Many people living with R.A. suffer from anemia: the inadequacy of red blood cells which carries oxygen out of the bloodstream into your entire body.
If the blood is not getting enough oxygen, the organ may feel weak, tired, or unwell.
R.A. increases your risk for anemia- due to a decreased production of red blood cells. You may also have a higher risk of blocked or hardened arteries. In rare cases, R.A. can lead to inflammation of the sac around the heart (pericarditis), the heart muscle ( myocarditis ), or even congestive heart failure.
The most common type of R.A. is the autoimmune anemia.
Blood Disease
Rheumatoid arthritis or some RA. medications can also make you anemic- because you don’t have enough healthy red blood cells to carry oxygen around your body.
Anemia symptoms include: Fatigue, Rapid or uneven heartbeat, Shortness of breath Dizziness Headaches Weakness, Leg cramps, Insomnia, or sleeplessness Thrombocytosis is another complication from R.A.
Lung
Although R.A. can damage the respiratory system, not everyone has symptoms.
In around 80% of people with R.A., the disease affects the lungs.
Prolonged inflammation in the lungs can lead to pulmonary fibrosis, which can cause scarring and breathing difficulties.
The primary lung complications associated with R.A. are interstitial lung disease (ILD). The illness occurs when lung tissue becomes infected, resulting in lung tissue scarring.
In November 2020, researchers found a 62.5% prevalence of subclinical ILDs in the United Kingdom in the first quarter. Some studies show 58 percent.
Other problems include:
- Blocked airways ( bronchiolitis obliterans ).
- Fluid in the chest ( pleural effusion ).
- High blood pressure in the lungs ( pulmonary hypertension ).
- Scarring of the lungs rheumatoid nodules on the lungs.
Inflammation of the lungs or lung lining can lead to pleurisy, which can cause pain, a persistent cough, and shortness of breath. Inflammation of the tissue around the heart can lead to pericarditis, which causes pain in the chest.
RA affects your lungs -pleural effusion, which is fluid buildup between the lining of your lung and your chest cavity.
Interstitial lung diseases, which involve scarring of the lung tissue, and pulmonary hypertension, a type of high blood pressure that damages arteries in the lung and heart, can be complications of R.A.
Circulatory system
The circulatory system is the body system that provides oxygen, nutrients, nutrients, cellular nutrition, and oxygen in the body to provide nourishment. It is possible to develop R.A. by undergoing heart disease or vasculitis.
What is rheumatoid arthritis?
According to Arthritis Foundation, about 1.5 million U.S. people live with R.A.
RA is a chronic disease which may impact your life.
What are the signs and symptoms of R.A.?
Symptoms of R.A. can occur in any of the body’s joints, including your: fingers, wrists, shoulders, elbows, hips, knees, ankles, toes R.A. can also result in bunions, claws, toes, hammertoes.
As the disease progresses, cartilage and bone are damaged and destroyed. Eventually, supporting tendons, ligaments, and muscles weaken. They lead to a limited range of motion or difficulty moving the joints properly. In the long term, joints can become deformed.
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
What causes R.A.?
The exact cause of R.A. is not known. R.A. is an autoimmune disorder.
What are the risk factors for R.A.?
Researchers have studied many genetic and environmental factors to determine if they change a person’s risk of developing R.A.
Characteristics that increase risk
- Age. R.A. can begin at any age, but the likelihood increases with age. The onset of R.A. is highest among adults in their sixties.
- Sex. New cases of R.A. are typically two-to-three times higher in women than men.
- Genetics/inherited traits. People born with specific genes are more likely to develop R.A.
- Smoking. Multiple studies show that cigarette smoking increases a person’s risk of developing R.A. and worsens the disease.
- History of live births. Women who have never given birth may be at greater risk of developing R.A.
- Early Life Exposures. Some early life exposures may increase the risk of developing R.A. in adulthood. Children of lower-income parents are at increased risk of developing R.A. as adults.
- Obesity. Being obese can increase the risk of developing R.A. Studies examining the role of obesity also found that the more overweight a person was, the higher their risk of developing R.A. became.
How is Rheumatoid Arthritis treated?
People with RA. often benefit from early diagnosis and a tailored treatment plan.
R.A. is a progressive disease that usually worsens gradually, though medication can help control inflammation, slow its progress and bone damage.
Some ra drugs may be used for pain relief. Some are used to treat inflammation. Others can help to slow the disease from getting worse.
Drug effects: While many R.A. medications, including methotrexate, other DMARDs, and biologics, may reduce cardiovascular risk in people with R.A., other medications – chiefly NSAIDs – may increase the risk of cardiovascular events, including heart attack.
Some RA. medications can make the immune system less effective- making people more vulnerable to respiratory infections, including pneumonia and tuberculosis.
Some medications that treat R.A. also affect your risk of diabetes. Steroids and statins can raise your blood sugar and make you more likely to get the disease. But other R.A. drugs may protect against it, including hydroxychloroquine, abatacept ( Orencia ), and a group of medicines called TNF inhibitors.
Rarely, the drug methotrexate, which many people with R.A. take, can also cause lung problems.
Disease-modifying antirheumatic drugs (DMARDs) can treat the underlying cause of your condition and reduce inflammation. They’re given to people with autoimmune disorders, such as rheumatoid arthritis, psoriatic arthritis, and lupus. These are conditions where the immune system, which usually fights infection, attacks the body’s healthy tissues.
DMARDs can improve symptoms such as pain, stiffness, and swelling, but they may take a few weeks or even months to entirely.
Athough DMARDs help many people with R.A., they may not work well enough for you.
For more information about the treatment of R.A., review the Clinical Practice Guidelines for the Treatment of Rheumatoid Arthritisexternal icon from the American College of Rheumatology (ACR) or the ACR’s
Going forward
Join a self-management education class.
Participants with arthritis (including R.A.) gain confidence in learning how to control their symptoms, live well with arthritis, and how arthritis affects their lives. Learn more about the proven self-management education programs that CDC recommends.
Get help from Arthritis Foundation Aquatic Program (AFAP), Arthritis Foundation Exercise Program (AFEP), Active Living Every Day (ALED)
Tools & Resources R.A. Symptoms, Causes, and More Simple Definitions for Common R.A. Term Why Are My Joints So Stiff? Is Your R.A. Progressing? Joint-Friendly Workouts
the effects of rheumatoid arthritis can reach far beyond the joints. By Meryl Davids Landau and Tula Karras Medically Reviewed by Alexa Meara, MD Reviewed: August 5, 2021, Facebook Pinterest Copy Link Medically Reviewed An inflammatory and systemic disease, rheumatoid arthritis can progress to various parts of the body if it is not treated. Content is reviewed before publication and upon substantial updates. Learn more. By Anita C. Chandrasekaran, MD, MPH Medically reviewed by Anita C. Chandrasekaran, MD, MPH LinkedIn Anita Chandrasekaran, MD, MPH, is board-certified in internal medicine and rheumatology and currently works as a rheumatologist at Hartford Healthcare Medical Group in Connecticut.
Does Rheumatoid arthritis affect the ankles? Medically reviewed by Nancy Carteron, M.D., FACR
Rheumatoid Arthritis Reference Menu Rheumatoid Arthritis (R.A.) Complications Medically Reviewed by David Zelman, MD, on November 6, 2020
FEEDBACK: Medically reviewed by Debra Sullivan, Ph.D., MSN, R.N., CNE, COI — Written by Kristeen Cherney — Updated on November 26, 2019
When should I call my healthcare provider?
Tell your healthcare provider if your symptoms worsen or you have new symptoms.