Introduction- Blepharitis Cure
Blepharitis occurs when the eyelid margin becomes damaged acutely and chronically.
Symptoms or signs include itching and swelling in the eyelids.
Diagnostics are based on history. Causes include a blocked oil gland on your eyelid.
Acute ulcerative blepharitis can usually be managed with topical antibiotics or with antiviral treatment.
We can treat Acute non-ulcerative blepharitis with a topical corticosteroid.
We treat chronic disease with tear supplementation, hot compresses, and oral antibiotics for Meibomian gland dysfunction or eye hygiene and tear supplements for seborrheic blepharitis.
Blepharitis is a chronic condition for people with chronic dry eyes Very difficult to achieve blepharitis cure except when you come to TheraLife.
In this article, you will learn how to get blepharitis cure that lasts.
Powerful Blepharitis Cure That Works- TheraLife
Treat dry eyes, blepharitis, MGD to get rid of blepharitis for good. Looking at blepharitis cure, you have come to the right place.
Am I at risk for blepharitis?
Your chances of blepharitis are greater if:
You’re at higher risk for blepharitis if you have: Dandruff — flaky patches of skin on your scalp or face. Rosacea — a skin condition that causes redness and bumps, usually on your face. Oily skin Allergies that affect your eyelashes
Many patients with a skin condition – seborrheic blepharitis have seborrheic dermatitis.
Seborrheic dermatitis is a common inflammatory condition of skin regions with a high density of sebaceous glands (e.g., face, scalp, sternum).
Causes – blepharitis cure
Blepharitis is inflammation of the oil glands in your eyelids. It’s the most common cause of dry eyes.
Blepharitis can occur from various causes and is a chronic condition with persistent symptoms that last a month or a decade. Acute cases can trigger chronic diseases. These conditions include skin cancer and connective inflammatory conditions. Severe acute blepharitis is often associated with eyelid ulceration and could cause serious infections, including cellulitis.
Blepharitis may have several causes- bacteria and mites.
Bacterial
Bacteria cause anterior blepharitis (staphylococcal blepharitis) or dandruff of the scalp and eyebrows (seborrheic blepharitis). These bacteria are commonly on the face and lids. Still, an infection may occur if they become excessive or the lid area reacts poorly to their presence. Usually, anterior blepharitis causes bacterial infections such as dandruff and hairs in the scalp and eyebrow dandruff (siderophore blepharitis). These bacteria are common on the face or the lip. Still, the skin can be infiltrated by excessive, or a lid is affected in a poorly regulated way. More often, allergies or mite infestations on eyelashes are responsible for resulting in anterior blepharitis.
Mites- Demodex
Blepharitis may result from an over-population of microscopic mites, known as Demodex, in the eyelash follicles.
These can include infection, clogged oil glands in the eyelids, or increased oil production in these glands. People with seborrheic dermatitis, an irritation of the top layers of skin, may be more likely to have blepharitis.Posterior blepharitis occurs when eyelid gland glands produce oil irregularly (meibomian blepharitis). The result is good conditions for bacteria to grow in the soil. Various skin ailments, including rosacea and scalp dandruff, can cause posterior blepharitis.
What are other risk factors for developing blepharitis?
Depending upon whether your skin blepharitis is present or not, you have rosacea; you might develop blepharitis if you also have :
- A stye is a bacterial infection involving one or more small glands near the base of your eyelashes. It is similar to a boil or a pimple and is often painful.
- If you have blepharitis, you might also have:
- Eyelash problems. Blepharitis can cause your eyelashes to fall out, grow abnormally (misdirected eyelashes), or lose color.
- Eyelid skin problems. Scarring can develop on your eyelids from long-term blepharitis. Or the eyelid edges might turn inward or outward.
- Excess tearing or dry eyes.
- Abnormal oily secretions and other debris shed from the eyelids, such as flaking associated with dandruff, can build up in your tear film.
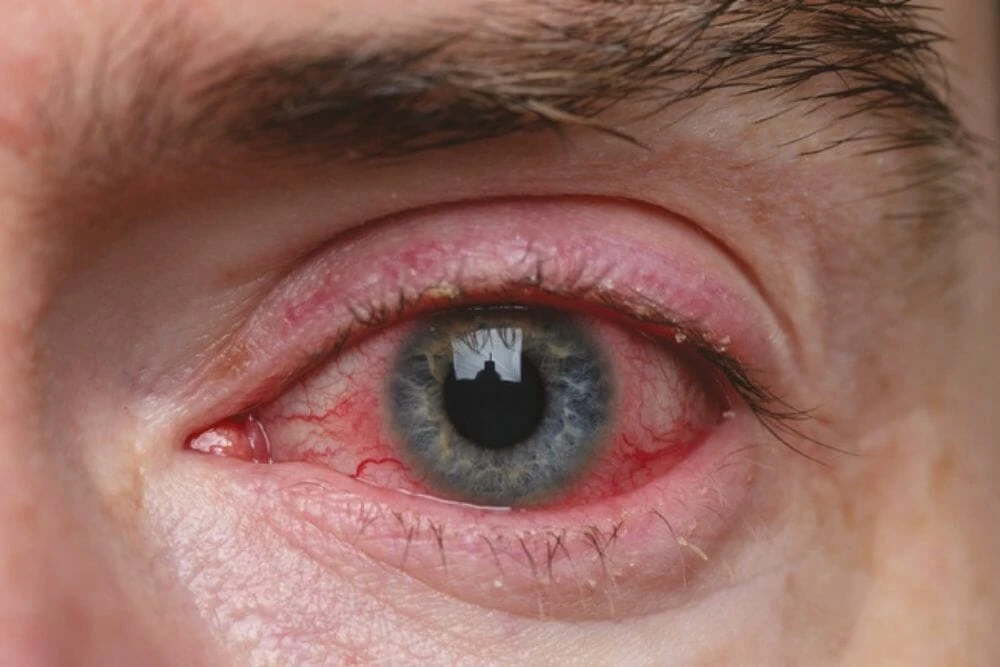
What are the signs and symptoms of blepharitis? Blepahritis cure
The most common signs of blepharitis include:
- Red or watery eyes.
- Itchy eyes.
- Red or swollen eyelids.
- Sticky eyelids.
- Flaky skin around eyes.
- Loss of eyelashes crusty-looking eyelashes.
Blepharitis Causes
Blepharitis can occur from various causes and is a chronic condition with persistent symptoms that last a month or a decade. Chronic conditions are usually triggered in acute cases. These conditions include skin cancer and connective inflammatory diseases. Severe acute blepharitis is often associated with eyelid ulceration and could cause serious infections, including cellulitis.
Blepharitis symptoms- Blepharitis cure
Blepharitis is a common disease in many eye conditions. The most common symptoms of blepharitis include red or watery eyes, itchy eyelids, eyelids swelling and turning red, sticking eyelids, flaky skin around the eyes, and loss of eyelashes and crusty-looking eyelashes. Blepharitis Symptoms common to all forms of blepharitis include itching and burning of the eyelid margins and conjunctival irritation with lacrimation, photosensitivity, and foreign body sensation. Symptoms tend to worsen in the early morning than those of keratoconjunctivitis sicca, which tend to worsen toward the end of the day.
Are there different types of blepharitis? Blepharitis cure
Blepharitis can vary in severity based on the location. Anterior and posterior.
Anterior blepharitis
Dandruff of the scalp and eyebrows (seborrheic blepharitis – read ore under acne rosacea.
These bacteria are commonly found on the face and lids.
Still, an infection may occur if they become excessive or the lid area reacts poorly to their presence.
Less commonly, allergies or a mite infestation of the eyelashes can cause anterior blepharitis.
Posterior blepharitis
Posterior blepharitis affects the eyelids inside the eyelid that touches the eyeballs.
Posterior blepharitis can also develop as a result of other skin conditions, such as rosacea and scalp dandruff.
Causes of posterior blepharitis
It can cause symptoms of blepharitis, such as staphylococcal seborrheic ulcerative blepharitis, e.g., staphylococci.
Chronic blepharitis
In meibomian gland dysfunction, examination reveals dilated, inspissated gland orifices that, when pressed, exude a waxy, thick, yellowish secretion. In seborrheic blepharitis, greasy, easily removable scales develop on eyelid margins—most patients with seborrheic blepharitis and meibomian gland.
How is blepharitis diagnosed?
Treating any blepharitis by using any other test in the body is possible. What steps should you be taking when diagnosing blepharitic symptoms?
How will my eye doctor check for blepharitis?
A doctor of optometry can determine the type of blepharitis based on the appearance of the eyelid margins.
Your eye surgeon can diagnose blepharitis by physical exams of your eyes. Your physician will also check on your eyelids and eyelashes.
How will an eye care provider treat my blepharitis?
Blepharitis treatment depends on your condition. Upon examining and cleaning your eyelids, your doctor can provide individualized care.
Treating blepharitis by treating the root cause
We treat the underlying cause of blepharitis, as well as the symptoms. Skin conditions such as rosacea may also cause blepharitis. Some medications, skin creams, and eye drops can help.
Artificial tears
Antibiotics are either an ointment, drops, or spray for your eyes or pills you swallow. Antiviral drugs Plugs that block your tear ducts to keep more tears in your eyes
Eye drops.
Your doctor may prescribe steroid eye drops to control redness, swelling, and irritation. Your doctor may also recommend a type of eye drops called artificial tears. You can get these eye drops without a prescription.
Warm compresses
There’s no cure for blepharitis. But you can manage and treat it by taking care of your eyelids. Warm compresses can help soften the crust and loosen oily debris.
Apply light pressure along your eyelashes to squeeze out clogged oils from the glands behind your lashes. Rinse thoroughly with a clean, warm, wet washcloth. Pat dry. Then do the other eye – this includes frequently washing the scalp and face, using warm compresses to soak the eyelids, and scrubbing the eyelids.
Antibiotics
Antibiotic ointment like erythromycin, bacitracin, ophthalmic, or PolysporinTM for your eyelids can treat blepharitis. This treatment can help reduce inflammation and reduce eyelid swell. In case of persistent cases, it is usually required to administer antibiotics or doxycycline or azithromycin.
Clinical procedures- blepharitis cure
Your doctor may perform more recent procedures – this includes:
- Microblepharoexfoliation:
- Microsponge gently exfoliates away the biofilm, crusting, bacterial colonies, and demodex infesting the eyelashes.
- Intense pulsed light (IPL): Non-laser light energy is applied to the eyelid skin, and this can liquefy obstructions in the Meibomian glands, improve oil secretion, decrease eyelid redness, and reduce spider veins.
- Thermal pulsation: Specialized applicator devices are gently applied to the eyelids, providing controlled thermal (heat) energy and massage (pulsation).
- Antibiotic eye drops to treat blepharitis-
- In cases involving bacterial infection, an antibiotic may be prescribed.
Use antibiotic ointments like erythromycin, bacitracin, ophthalmic, or PolysporinTM for your eyelids. This treatment may help reduce inflammation and reduce swelling. In case of persistent cases, it is usually required to administer antibiotics or doxycycline or azithromycin.
Complications- blepharitis cure
Chronic blepharitis.
Pink eye (conjunctivitis): Some types of blepharitis may turn into chronic pink eye.
Stye
A stye is a red, painful eyelid bump near your eyelashes. Tear film issues: Tears exist in a delicate balance of mucus, oil, and water to keep your eyes moist and protected.
Chalazion
A chalazion is a small, painless eyelid bump/swelling. Corneal ulcer (keratitis): A sore on your cornea can result from prolonged infection or eyelid swelling. Eyelid issues: Eyelashes may shed, grow in odd directions or lighten because of chronic blepharitis.
Pink eye (conjunctivitis)
Some types of blepharitis may turn into chronic pink eye.
Tear film issues
Tears in a delicate balance of mucus, oil, and water to keep your eyes moist and protected
Chronic, bilateral desiccation of the conjunctiva and cornea due to an inadequate tear film. Symptoms include itching, burning, irritation, and photophobia.
Acute blepharitis
In acute ulcerative blepharitis, small pustules may develop in eyelash follicles and eventually break down to form shallow marginal ulcers. Tenacious adherent crusts leave a bleeding surface when removed. During sleep, eyelids can become glued together by dried secretions. Recurrent ulcerative blepharitis can cause eyelid scars and loss or misdirection ( trichiasis )
How to prevent blepharitis? Blepharitis cure
Things you can do to treat and prevent blepharitis- eyelid hygiene.
- Eyelid hygiene – Clean your eyelids twice daily to start with and then once daily as your symptoms improve. Continue to clean your eyes, even if your symptoms clear up.
- Don’t do not wear contact lenses while you have symptoms.
- Do not use eye makeup, especially eyeliner and mascara, while you have symptoms.
- How to clean your eyes – Soak a clean flannel or cotton wool in warm water and place it on your closed eyelid for 5 to 10 minutes. Gently massage your eyelids for around 30 seconds. Clean your eyelids using cotton wool or a cotton bud. We recommend Avenova eyelid cleanser if you have blepharitis.
- Remove all eye makeup before bed. Don’t use eyeliner on the back edges of your eyelids, behind the lashes. If you’re in the early stages of treating blepharitis, prevent further irritation by not using makeup.
Your eye doctor can suggest things to help keep your eyelids clean, including eye pads and wipes, and eye drops.
Frequently asked questions- Blepharitis cure
How do you get rid of blepharitis fast?
Fastest way to get rid of blepharitis is with hot compress and eyelid margins cleansing. Long term blepharitis cure can be achieved by treating dry eyes, blepharitis and MGD at the same time Come to TheraLife for help.
What is the best ointment for blepharitis?
Antibiotic oitment such as azitromycin, erythromycine, work well for blepharitis. Antibiotics will get rid of blepharitis for you temporarily But if you have dry eyes, it will recur.
How long does blepharitis take to clear up?
In most cases, blepharitis with the proper treatment should clear up within 2 weeks. If blepharitis recur, you must treat dry eyes to keep it away. Try TheraLife for blepharitis cure.
How do you get rid of blepharitis on your eyelid?
Depends on whether the blepharitis is caused by bacteria or mites. Bacteria blepharitis can be treated with eyelid cleanser like Avenova Deodex mites can be treated with Tea Tree Oil based eyelid cleanser. Once you get rid of blepharitis on your eyelid, the constant inflammation from you dry eyes will cause recurrence. Come to TheraLife for blepharitis cure.
How do I know if I’ve got blepharitis?
Your eyes will be red, crusty, eyelids inflamed, eyes light sensitive and watery.
Conclusion
Blepharitis can be uncomfortable. But it isn’t contagious and usually doesn’t cause any lasting damage to your eyes.
The primary treatment for blepharitis is regularly cleaning your eyelids and keeping them free of crusts. Blepharitis usually doesn’t go away completely, but you can take steps to manage your symptoms. Talk to your eye doctor about what’s causing your blepharitis and the best ways to manage it.
References
1.Huggins AB, Carrasco JR, Eagle RC. MEN 2B masquerading as chronic blepharitis and euryblepharon. Orbit. 2019 Dec;38(6):514-518. [PubMed]
2.Rodriguez-Garcia A, Loya-Garcia D, Hernandez-Quintela E, Navas A. Risk factors for ocular surface damage in Mexican patients with dry eye disease: a population-based study. Clin Ophthalmol. 2019;13:53-62. [PMC free article] [PubMed]
3.Choi FD, Juhasz MLW, Atanaskova Mesinkovska N. Topical ketoconazole: a systematic review of current dermatological applications and future developments. J Dermatolog Treat. 2019 Dec;30(8):760-771. [PubMed]
4.Ozkan J, Willcox MD. The Ocular Microbiome: Molecular Characterisation of a Unique and Low Microbial Environment. Curr Eye Res. 2019 Jul;44(7):685-694. [PubMed]
5.Khoo P, Ooi KG, Watson S. Effectiveness of pharmaceutical interventions for meibomian gland dysfunction: An evidence-based review of clinical trials. Clin Exp Ophthalmol. 2019 Jul;47(5):658-668. [PubMed]
6.Soh Qin R, Tong Hak Tien L. Healthcare delivery in meibomian gland dysfunction and blepharitis. Ocul Surf. 2019 Apr;17(2):176-178. [PubMed]
7.Fromstein SR, Harthan JS, Patel J, Opitz DL. Demodex blepharitis: clinical perspectives. Clin Optom (Auckl). 2018;10:57-63. [PMC free article] [PubMed]
8.Pflugfelder SC, Karpecki PM, Perez VL. Treatment of blepharitis: recent clinical trials. Ocul Surf. 2014 Oct;12(4):273-84. [PubMed]
9. Kanda Y, Kayama T, Okamoto S, Hashimoto M, Ishida C, Yanai T, Fukumoto M, Kunihiro E. Post-marketing surveillance of levofloxacin 0.5% ophthalmic solution for external ocular infections. Drugs R D. 2012 Dec 01;12(4):177-85. [PMC free article] [PubMed]
10.Veldman P, Colby K. Current evidence for topical azithromycin 1% ophthalmic solution in the treatment of blepharitis and blepharitis-associated ocular dryness. Int Ophthalmol Clin. 2011 Fall;51(4):43-52. [PubMed]
11. Hosseini K, Bourque LB, Hays RD. Development and evaluation of a measure of patient-reported symptoms of Blepharitis. Health Qual Life Outcomes. 2018 Jan 11;16(1):11. [PMC free article] [PubMed]