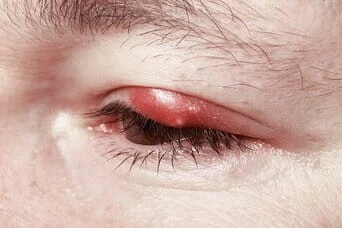
Do you have recurring chalazion?
Do you have recurring chalazion? This bump on your eyelids that hurts? You may even have had surgeries to remove the scar tissue. Are you aware that this is caused by dry eyes and clogged oil glands (MGD?
Yes, you can get rid of your chalazion by treating your dry eyes and MGD. This is the approach TheraLife takes. To learn more, click here.
What is it?
A chalazion is a clog in your eyelid (called the meibomian glands ) that looks like a small bump and cause eyelid swelling. Each of your eyelids has oil glands called meibomian glands near the eyelashes, which produce lubricates to thicken your tears. When these glands do not release their oil because they are blocked, the oil backs up and causes a bump.
It is not the result of an infection, although it can follow an infection. An infection of the gland is called a stye, which may look like a chalazion but is usually painful and tender. A chalazion can grow to the size of a marble in extreme circumstances.
People have recurring chalazion or styes. This is a chronic condition that requires treatment. TheraLife has the perfect solution.
Causes
Each of the oil glands produces oil that flows out of the gland opening into the tears to make the tears thicker. There are about 30 to 40 of these glands within each of the upper and lower lids. The oil comes out from each gland through a tiny circular opening just behind the eyelashes of the upper and lower lids of both eyes.
It is caused by the oil in the gland becoming too thick to come out of the gland or obstructed gland opening. The oil builds up inside the gland and forms a lump or type of cyst in the eyelid. The gland wall may break, releasing the oil into the eyelid tissue, causing inflammation and sometimes scar tissue. This is when surgery is needed.
Chalazion vs Stye
Although a stye is also a lump in the eyelid caused by an oil gland’s obstruction, a chalazion is not a stye. A stye is an acute infection of the gland. A chalazion is not infectious but is an inflammation of the eyelid. Inflammation causes swelling, redness, pain, or warmth. A stye is usually more painful than a chalazion and may appear infected.
Risk Factors
Risk factors include a prior history of a chalazion, acne rosacea, and oily skin. Working in a dirty environment can also cause chalazion or stye.
Symptoms and Signs
- Swelling of the upper or lower eyelid. More often on the upper lid.
- A chalazion appears as a localized hard lump that may grow as large as 1/8 of an inch.
- Occasionally, one may feel pain, and the eyelid may be red. A chalazion on the lower eyelid may be more visible.
Precautions should be taken if you experience any of the following.
- Fever
- Headache
- Any visual changes (for example, blurred vision, decreased ability to see)
- Eye pain and/or drainage
- Extensive swelling or redness
Diagnosis
Your eye doctor will take a medical history and perform a physical examination. The examination includes vision testing of each eye and an inspection of the face, eyelids, and the eye itself. In addition to examining the eyelids’ skin, an eye doctor may look inside the upper eyelid if the lump is in the upper lid.
- Hot compress for 5 to 10 minutes, 4 times a day to reduce swelling and bring the chalazion into a white head. We recommend a gel type of hot compress that heats up in the microwave oven, which retains heat well.
- Anti-biotics – A prescription for antibiotic eye drops or ointments if a bacterial infection is suspected.
- Steroid Injection – in the area of the lump to help decrease the inflammation and promote healing.
- Surgery – If scar tissues form due to chalazia, it may need to be surgically removed.
Recurrence
Chronic dry eyes, acne rosacea, oily skin, or chalazion history are more likely to result in recurring chalazia.
For recurrence- treating dry eyes, blepharitis, and MGD (blocked oil glands) must be done simultaneously. Doxycycline is often used to change the consistency of the oils produced by the glands. Using hot compresses before sleep and cleaning the eye lid margins using an eye lid cleanser should be a routine procedure.
For the most effective recurring chalazion relief, try TheraLife Chalazion Starter Kit. This kit consists of 4 bottles of Theralife Eye, 1 bottle of Fish Oil, 1 gel hot compress, and 1 Hypochlor eyelid cleanser. Keep your eyelids clean, healthy, and restore your normal tear function all in one kit.
To purchase- click here.
Read more customer testimonials here.
Call and talk to a Dr. Yang toll-free 1-877-917-1989 US/Canada. International (650) 949-=6080
Email inquiries to : [email protected]
References
- Nemet AY, Vinker S, Kaiserman I. Associated morbidity of chalazia. Cornea. 2011;30:1376–81.
- Ben Simon GJ, Huang L, Nakra T, Schwarcz RM, McCann JD, Goldberg RA. Intralesional Triamcinolone Acetonide Injection for Primary and Recurrent Chalazia: Is It Really Effective? Ophthalmology. 2005;112:913–7.
- Goawalla A, Lee V. A prospective randomized treatment study comparing three treatment options for chalazia: triamcinolone acetonide injections, incision and curettage and treatment with hot compresses. Clin Experiment Ophthalmol. 2007;35:706–12
4. Olsen T. Calculation of intraocular lens power: a review. Acta Ophthalmol Scand. 2007;85:472–85.
- Holland S, Lin DT, Tan JC. Topography-guided laser refractive surgery. Curr Opin Ophthalmol. 2013;24:302–9.
- Myrowitz EH, Chuck RS. A comparison of wavefront-optimized and wavefront-guided ablations. Curr Opin Ophthalmol. 2009;20:247–50.
- Santa Cruz CS, Culotta T, Cohen EJ, Rapuano CJ. Chalazion-induced hyperopia as a cause of decreased vision. Ophthalmic Surg Lasers. 1997;28:683–4.
- Sabermoghaddam AA, Zarei-Ghanavati S, Abrishami M. Effects of chalazion excision on ocular aberrations. Cornea. 2013;32:757–60.
- Cosar CB, Rapuano CJ, Cohen EJ, Laibson PR. Chalazion as a cause of decreased vision after LASIK. Cornea. 2001;20:890–2.
- Packer M, Fine IH, Hoffman RS. Wavefront technology in cataract surgery. Curr Opin Ophthalmol. 2004;15:56–60.
- Tang CY, Charman WN. Effects of monochromatic and chromatic oblique aberrations on visual performance during spectacle lens wear. Ophthalmic Physiol Opt. 1992;12:340–9.
- Perry HD, Serniuk RA. Conservative treatment of chalazia. Ophthalmology. 1980;87:218–21.
- Bagheri A, Hasani HR, Karimian F, Abrishami M, Yazdani S. Effect of chalazion excision on refractive error and corneal topography. Eur J Ophthalmol. 2009;19:521–6.
- Park YM, Lee JS. The effects of chalazion excision on corneal surface aberrations. Cont Lens Anterior Eye. 2014;37:342–5.
- Zeng Y, Yang J, Huang K, Lee Z, Lee X. A comparison of biomechanical properties between human and porcine cornea. J Biomech. 2001;34:533–7.
- Boote C, Dennis S, Huang Y, Quantock AJ, Meek KM. Lamellar orientation in human cornea in relation to mechanical properties. J Struct Biol. 2005;149:1–6.
- Shin TJ, Vito RP, Johnson LW, McCarey BE. The distribution of strain in the human cornea. J Biomech. 1997;30:497–503.
- Hjortdal JO. Regional elastic performance of the human cornea. J Biomech. 1996;29:931–42.
- Meek, K.M., Newton, R.H. Organization of collagen fibrils in the corneal stroma in relation to mechanical properties and surgical practice. J Refract Surg 1999;15:695-9.
- Murray IJ, Elliott SL, Pallikaris A, Werner JS, Choi S, Tahir HJ. The oblique effect has an optical component: Orientation-specific contrast thresholds after correction of high-orderaberrations. J Vis. 2010;10:10.