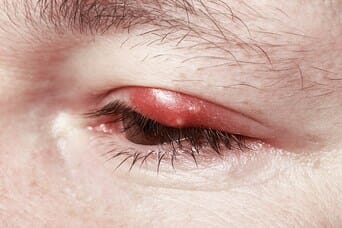
What is a stye?
A stye is an acute bacterial infection of the eyelid margin. 90% to 95% of cases of styes are due to Staphylococcus aureus, with Staphylococcus epidermidis being the second most common cause. An external stye represents a localized abscess (puss) formation of the follicle of an eyelash. In contrast, an internal hordeolum is an acute bacterial infection of the meibomian glands of the eyelid.
Infection by the bacteria staphylococcus causes styes. A stye is painful inflammation and swelling of the eyelid with an accumulation of pus. With appropriate treatment, it resolves without any complications.
What are the types?
There are two main types: stye and chalazion. They have different causes and treatments.
- Stye: It occurs due to blockage of the sweat gland (meibomian glands) found in the skin of the eyelid at the base of the eyelashes or a small sebaceous gland present at the bottom of the eyelashes. Sebaceous glands secrete sebum, a waxy, oily substance that provides moisture and protection to the skin and hair. In this case, sebum makes the tear thicker to reduce evaporation.
- A chalazion occurs due to blockage of a meibomian gland, a special sebaceous gland present only in the eyelid. It is located inside the eyelid and opens at the rim of the eyelid behind the lashes.
What are the signs and symptoms ?
After symptoms appear, a small pimple will develop in the affected area. Typically stye is accompanied by swollen eyes. Sometimes just the immediate area is swollen; at other times, the entire eyelid swells. Other symptoms include:
- It appears as a swollen, red bump over the upper or lower eyelid. Multiple swellings may be present
- Puffiness of the eyes
- Pain and tenderness
- Increased warmth over the affected area
- Increased pressure over the eyes
- The heaviness of the eye
- Epiphora (watering of the eyes)
- Crusting around the eyelids and eyelashes
- Crusting may cause the eyelids to stick to each other
- Itching
- Pus discharge that may or may not have blood
- Fever
What is a chalazion?
A chalazion is not infectious.
A chalazion is an acute or chronic inflammation of the eyelid secondary to obstruction of oil glands (meibomian gland). Processes that block the normal drainage of sebaceous glands, such as hordeolum, acne rosacea, and blepharitis, can contribute to the development of chalazia (plural of chalazion).
Causes
The root cause of styes stems from chronic dry eyes, which results in blepharitis and MGD ( clogged meibomian oil glands). All three conditions are related- creating a vicious cycle of inflammation at the center of dry eye disease.
Chronic dry eyes result in inflammation which shuts down cellular functions of the tear production.
Blepharitis is a related condition that involves inflammation of the eyelid margin characterized by:
- erythematous,
- pruritic eyelids,
- conjunctival injection,
- crusting or matting of the eyelids
- occasionally flaking of the eyelid skin.
Blepharitis and Stye
Blepharitis should not have a discrete nodule within the eyelid. Stye and chalazion have nodules. Treatment of blepharitis involves:
warm compresses, gentle washing of the eyelids with warm water, or diluted baby shampoo if these attempts are unsuccessful, a topical antibiotic such as erythromycin.
Meibomian Gland Dysfunction (MGD) – clogged oil glands located on both upper and lower eyelids. 86% of all dry eye cases have MGD. Clogged oil glands allow bacteria to fester, resulting in styes.
How to stop recurrence
TheraLife – complete protocol to stop recurrence.
TheraLife treats dry eyes, blepharitis, MGD simultaneously to get the best results to stop recurring styes. Since TheraLife is an oral dry eye treatment, it works internally to normalize and balance cellular functions to relieve dry eyes.
To learn more- click here
Home remedies
It is usually not possible to get rid of a stye entirely overnight. Several ways can fasten the healing include:
- Avoiding makeup, over the counter beauty products, masks, or contact lenses
- Protecting the eyes from dust and pollution
- Warm compression and massaging: Use a clean washcloth dipped in warm water and gently placing it over the affected eye for 5-15 minutes. You can use a warm compress several times a day. A hot washcloth does not work – it gets cool too quickly—gentle massaging with a warm compress. Warm compression reduces pain, and swelling moves the pus to the surface, dissolves pus, and removes crusts.
- Applying a warm tea bag: Using a warm tea bag as a warm compress reduces inflammation, infection, and pain. Use warm tea bags several times a day to speed up healing.
- Gentle cleansing: Gentle cleansing of the eyes using a mild antibacterial soap removes crusts, reduces infection, and maintains hygiene.
Medical treatments
- Painkillers
- Oral antibiotics, antibiotic ointments, or eye drops prescribed by a physician help quick healing.
- Injection of steroids into the affected area to reduce inflammation
- Surgical treatment: In case of a chalazion that does not resolve – it may need minor surgery to drain the lesion and prevent a recurrence.
Can you pop a stye?
Because a stye may sometimes be similar in appearance to a pimple, it should not be touched repeatedly or popped. Popping a stye can be very painful, leading to worsening of infection and recurrence or scarring.
How to speed up recovery
Here are eight ways to speed up the healing process.
- Use a warm compress.
- Clean your eyelid with mild soap and water.
- Use a warm tea bag.
- Take OTC pain medication.
- Avoid wearing makeup and contact lenses.
- Use antibiotic ointments.
- Massage the area to promote drainage.
- Get medical treatment from your doctor.
Prevention
- Taking TheraLife Eye capsules to relieve dry eyes, stop the inflammation that causes styes. Maintaining hygiene of the eye, eyelids, and eyelashes
- Avoiding harsh face products around the eyes
- Using dermatologically and ophthalmologically tested makeup and beauty products
- Consuming a healthy and nutritious diet
- Protecting the eyes from chemicals and pollution
Treatment #1: Keep Your Eyelids Clean
- Cleanse your eyelids. The first thing you should do if you develop a stye is clean your eyelids. You can use diluted tear-free baby shampoo on a cotton ball, washcloth, or makeup remover pad. Then rinse your eyelids with warm water and gently pat them dry.
- Wash your hands. Be sure to wash your hands before and after touching a stye, and don’t share your towels or washcloths with others.
- Use a cleansing pad. Pre-moistened eyelid cleansing pads are another option. You can find these non-prescription items in most drugstores.
- Pause your makeup use. It’s wise to stop wearing eye makeup temporarily when you have a stye, because covering up a stye can delay the healing process. Also, discard old makeup or applicators that could be contaminated.
- Wear your glasses, not contacts, for a bit. And if you need vision correction, wear glasses rather than contact lenses until your stye heals.
Treatment #2: Apply Warm, Moist Compresses
- Apply warm compresses. You can speed the healing of a stye by applying warm compresses for 10 to 15 minutes, three or four times a day.
- Try a tea bag or washcloth. Some people use tea bags for this purpose, but a basic clean washcloth dipped in warm (not hot) water will do the trick and is easy to prepare. Wring the cloth, so it’s not dripping, then place it over your closed eyes.
- Don’t pop a stye. This therapy aims to bring the stye to the head as you see on a pimple. But whatever you do, don’t get anxious and try to pop a stye! The warmth from the compress often will allow the stye to open, drain and heal on its own without causing trauma to the eyelid or possibly spreading infection by squeezing it.
Ease The Discomfort
- Painkillers: Over-the-counter painkillers like acetaminophen and ibuprofen won’t do much to speed healing but can ease discomfort if a stye is bothersome.
- Eye surgery: Your eye doctor also can address pain associated with styes. Sometimes, your eye doctor may choose to surgically open a large stye to relieve discomfort and prevent severe infection.
Seek Professional Help
Although these tips will help clear up fairly quickly, don’t hesitate to contact your eye doctor for additional advice. Your doctor might prescribe an ointment or other treatment to help the condition resolve more quickly.
If your stye worsens, affects your vision, or doesn’t go away within a week or so, contact your eye doctor for an in-office evaluation and treatment. In some cases, stubborn styes may require surgical treatment by your doctor, followed by the application of prescription medicine.
Preventing
Take TheraLife Eye capsules to relieve dry eyes. Eliminate the root cause of styes.
Proper eyelid hygiene can significantly reduce the risk. Clean your eyelids thoroughly before bedtime, especially if you wear eye makeup.
If you sometimes have problems with blepharitis, take steps to treat this eyelid problem for prevention.
Get help from TheraLife today. Call us toll-free at 1-877-917-1989 US/Canada. International 650-949-6080
Email to [email protected]
References
- Bragg KJ, Le PH, Le JK. StatPearls [Internet].StatPearls Publishing; Treasure Island (FL): Aug 8, 2020. Hordeolum.
- Lindsley K, Nichols JJ, Dickersin K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2017 Jan 09;1:CD007742.
- Carlisle RT, Digiovanni J. Differential Diagnosis of the Swollen Red Eyelid. Am Fam Physician. 2015 Jul 15;92(2):106-12.
- Amato M, Pershing S, Walvick M, Tanaka S. Trends in ophthalmic manifestations of methicillin-resistant Staphylococcus aureus (MRSA) in a northern California pediatric population. J AAPOS. 2013 Jun;17(3):243-7.
- Moriya K, Shimizu H, Handa S, Sasaki T, Sasaki Y, Takahashi H, Nakamura S, Yoshida H, Kato Y. Incidence of Ophthalmic Disorders in Patients Treated with the Antineoplastic Agent S-1. Gan To Kagaku Ryoho. 2017 Jun;44(6):501-506.
- Ansari AS, de Lusignan S, Hinton W, Munro N, McGovern A. The association between diabetes, level of glycaemic control and eye infection: Cohort database study. Prim Care Diabetes. 2017 Oct;11(5):421-429.
7.Pflipsen M, Massaquoi M, Wolf S. Evaluation of the Painful Eye. Am Fam Physician. 2016 Jun 15;93(12):991-8.
8.John AM, John ES, Hansberry DR, Thomas PJ, Guo S. Analysis of online patient education materials in pediatric ophthalmology. J AAPOS. 2015 Oct;19(5):430-4.
9.Machalińska A, Zakrzewska A, Safranow K, Wiszniewska B, Machaliński B. Risk Factors and Symptoms of Meibomian Gland Loss in a Healthy Population. J Ophthalmol. 2016;2016:7526120.
10.Hirunwiwatkul P, Wachirasereechai K. Effectiveness of combined antibiotic ophthalmic solution in the treatment of hordeolum after incision and curettage: a randomized, placebo-controlled trial: a pilot study. J Med Assoc Thai. 2005 May;88(5):647-50.