Petrygium and Dry Eyes
Petrygium often causes dry eyes which result in much discomfort and frustration. We are documenting a dry eye treatment for Petrygium that avoids the use of surgery.
What is Petrygium
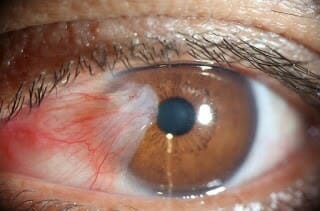
Pterygium is a growth of thin tissue on the conjunctiva that covers your eyeball. This growth can be slow and extends to cover part of the cornea. This condition is called Pterygium, also referred to as “Surfer’s Eye” because it is caused by extensive exposure to sunlight. In addition, pterygium is often started as a Pinguecula.
What is Pinguecula
Pinguecula is a yellow spot or bump on the corner of your eye that looks like a yellow fat deposit.
A pinguecula often gets bigger and develops into a pterygium. When this happens, the friction between your eyelid and the pterygium tissue causes inflammation and result in dry eyes. Dry eye symptoms such as itchy, foreign body sensation and red eyes are common.
Therefore, this causes much pain and suffering.
How Do Eye Doctors Treat Pterygium?
Eye doctors often recommend eye drops, and steroid drops for symptom relief. Depending on how severe the dry eye symptoms are, however, eye drops may not work. In addition, steroid drops are known to cause side effects such as increased intraocular pressure resulting in Glaucoma, or damages to the liver and kidney.
When the Pterygium growth becomes extensive and large, eye doctors often recommend surgery. However, eye surgeries tend to result in dry eyes afterward due to the invasive nature of the procedure.
What is more, other complications after Pterygium surgery has been documented2. Therefore, avoid surgery would be highly desirable if there are other non-invasive alternatives. TheraLife presents a dry eye treatment opportunity for Pterygium without the use of surgery.
What Are Chronic Dry Eyes?
Chronic dry eyes happens when one do not produce enough tears (tear insufficiency), or tear is too thin resulting in evaporative dry eye. The causes for dry eyes include but not limited to computer over use, contact lens wear, menopause, aging, and autoimmune diseases.
The symptoms of chronic dry eyes include blurry vision, foreign body sensation, light sensitivity, red irritated eyes, puffy eye lids, and eye pain. Besides, chronic dry eyes also lead to complications of Blepharitis, Meibomian Gland Dysfunction (MGD), cornea abrasions and more. What is more, chronic dry eyes left untreated could lead to blindness.
All these symptoms can be involved in people with Pterygium.
How Does TheraLife Treat Dry Eyes Cause by Pterygium?
TheraLife Eye capsules are an effective and powerful treatment for chronic dry eyes, including the symptoms caused by pterygium.
TheraLife Eye capsules increases tear production, reduce inflammation, and ease eye pain caused by surfer’s eye. It restores tear productions from inside out. Better yet, it is 100% natural, suitable for vegans.
Learn more how TheraLife Eye works.
A personal story from one of TheraLife’s customers
“I developed pterygium (surfer’s eye) in both eyes in 2006 due to dry eyes. I also started menopause – the hormone imbalance makes dry eye symptoms worse. My Tear Breakup Test was only 1 sec. Normal is between 10-15. I also had MGD (meibomian gland dysfunction) where my oil glands are clogged.
I started taking Theralife Eye capsules, krill and fish oil; hot compresses daily, and a healthy smoothie to fortify nutrients for the eyes. I used a gel compress over my eyes to keep my eyelids closed. I had a high-stress job for years which makes dry eye symptoms worse. My cholesterol level is now normal- hopefully, this will prevent further clogging of the Meibomian oil glands.
There are many factors to affect dry eyes. However, since I started the TheraLife protocol, it is making a difference. I am making more of my own natural tears, and pterygium stopped being a problem.
I am grateful to have found TheraLife.”
A. Lurenci- California, USA
References
1.Long Term and Intensive Use of Ophthalmic Topical Corticosteroids and the Risk of Positive Doping Test in Athletes: A Case Report https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4594141/
2.Serious corneoscleral complications after pterygium excision with mitomycin C– Br J Ophthalmol. 2002 Mar; 86(3): 357–358.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1771048/
1. ROSENTHAL JW. Chronology of pterygium therapy. Am J Ophthalmol. 1953 Nov;36(11):1601-16.
- 2.
- Moran DJ, Hollows FC. Pterygium and ultraviolet radiation: a positive correlation. Br J Ophthalmol. 1984 May;68(5):343-6.
- 3.
- Ang LP, Chua JL, Tan DT. Current concepts and techniques in pterygium treatment. Curr Opin Ophthalmol. 2007 Jul;18(4):308-13. [
- 4.
- Nangia V, Jonas JB, Nair D, Saini N, Nangia P, Panda-Jonas S. Prevalence and associated factors for pterygium in rural agrarian central India. The central India eye and medical study. PLoS One. 2013;8(12):e82439.
- 5.
- Luthra R, Nemesure BB, Wu SY, Xie SH, Leske MC., Barbados Eye Studies Group. Frequency and risk factors for pterygium in the Barbados Eye Study. Arch Ophthalmol. 2001 Dec;119(12):1827-32.
- 6.
- Ang M, Li X, Wong W, Zheng Y, Chua D, Rahman A, Saw SM, Tan DT, Wong TY. Prevalence of and racial differences in pterygium: a multiethnic population study in Asians. Ophthalmology. 2012 Aug;119(8):1509-15.
- 7.
- Shiroma H, Higa A, Sawaguchi S, Iwase A, Tomidokoro A, Amano S, Araie M. Prevalence and risk factors of pterygium in a southwestern island of Japan: the Kumejima Study. Am J Ophthalmol. 2009 Nov;148(5):766-771.e1.
- 8.
- Lu P, Chen X, Kang Y, Ke L, Wei X, Zhang W. Pterygium in Tibetans: a population-based study in China. Clin Exp Ophthalmol. 2007 Dec;35(9):828-33. [
- 9.
- Lu J, Wang Z, Lu P, Chen X, Zhang W, Shi K, Kang Y, Ke L, Chen R. Pterygium in an aged Mongolian population: a population-based study in China. Eye (Lond). 2009 Feb;23(2):421-7. [
- 10.
- Liu L, Wu J, Geng J, Yuan Z, Huang D. Geographical prevalence and risk factors for pterygium: a systematic review and meta-analysis. BMJ Open. 2013 Nov 19;3(11):e003787.
- 11.
- Di Girolamo N, Chui J, Coroneo MT, Wakefield D. Pathogenesis of pterygia: role of cytokines, growth factors, and matrix metalloproteinases. Prog Retin Eye Res. 2004 Mar;23(2):195-228.
- 12.
- Hamed-Azzam S, Edison N, Briscoe D, Mukari A, Elmalah I. Identification of human papillomavirus in pterygium. Acta Ophthalmol. 2016 May;94(3):e195-7.
- 13.
- Reid TW, Dushku N. Does human papillomavirus cause pterygium? Br J Ophthalmol. 2003 Jul;87(7):806-8. [PMC free article] [
- 14.
- Li DQ, Lee SB, Gunja-Smith Z, Liu Y, Solomon A, Meller D, Tseng SC. Overexpression of collagenase (MMP-1) and stromelysin (MMP-3) by pterygium head fibroblasts. Arch Ophthalmol. 2001 Jan;119(1):71-80.
- 15.
- Di Girolamo N, McCluskey P, Lloyd A, Coroneo MT, Wakefield D. Expression of MMPs and TIMPs in human pterygia and cultured pterygium epithelial cells. Invest Ophthalmol Vis Sci. 2000 Mar;41(3):671-9.
- 16.
- Zeng W, Liu Z, Dai H, Yan M, Luo H, Ke M, Cai X. Anti-fibrotic, anti-VEGF or radiotherapy treatments as adjuvants for pterygium excision: a systematic review and network meta-analysis. BMC Ophthalmol. 2017 Nov 25;17(1):211.
- 17.
- Verma N, Garap JA, Maris R, Kerek A. Intraoperative use of mitomycin C in the treatment of recurrent pterygium. P N G Med J. 1998 Mar;41(1):37-42. [PubMed]
- 18.
- Rong SS, Peng Y, Liang YB, Cao D, Jhanji V. Does cigarette smoking alter the risk of pterygium? A systematic review and meta-analysis. Invest Ophthalmol Vis Sci. 2014 Sep 04;55(10):6235-43.
- 19.
- Hirst LW, Sebban A, Chant D. Pterygium recurrence time. Ophthalmology. 1994 Apr;101(4):755-8.
- 20.
- Prabhasawat P, Barton K, Burkett G, Tseng SC. Comparison of conjunctival autografts, amniotic membrane grafts, and primary closure for pterygium excision. Ophthalmology. 1997 Jun;104(6):974-85.
- 21.
- Hirst LW. Cosmesis after pterygium extended removal followed by extended conjunctival transplant as assessed by a new, web-based grading system. Ophthalmology. 2011 Sep;118(9):1739-46.
- 22.
- Zolli CL. Experience with the avulsion technique in pterygium surgery. Ann Ophthalmol. 1979 Oct;11(10):1569-76. [
- 23.
- GIBSON JB. Brisbane survey of pterygium. Trans Ophthalmol Soc Aust. 1956;16:125-34.
- 24.
- Youngson RM. Recurrence of pterygium after excision. Br J Ophthalmol. 1972 Feb;56(2):120-5.
- 25.
- Krag S, Ehlers N. Excimer laser treatment of pterygium. Acta Ophthalmol (Copenh). 1992 Aug;70(4):530-3.
- 26.
- D’Ombrain A. THE SURGICAL TREATMENT OF PTERYGIUM. Br J Ophthalmol. 1948 Feb;32(2):65-71.
- 27.
- Alpay A, Uğurbaş SH, Erdoğan B. Comparing techniques for pterygium surgery. Clin Ophthalmol. 2009;3:69-74.
- 28.
- Kareem AA, Farhood QK, Alhammami HA. The use of antimetabolites as adjunctive therapy in the surgical treatment of pterygium. Clin Ophthalmol. 2012;6:1849-54.
- 29.
- Yanyali AC, Talu H, Alp BN, Karabas L, Ay GM, Caglar Y. Intraoperative mitomycin C in the treatment of pterygium. Cornea. 2000 Jul;19(4):471-3.
- 30.
- Demirok A, Simsek S, Cinal A, Yasar T. Intraoperative application of mitomycin C in the surgical treatment of pterygium. Eur J Ophthalmol. 1998 Jul-Sep;8(3):153-6. [
- 31.
- Anduze AL. Merest sclera technique for primary pterygium surgery. Ophthalmic Surg. 1989 Dec;20(12):892-4. [PubMed]
- 32.
- Staz L. A MODIFICATION AND EXTENSION OF THE McREYNOLDS’ OPERATION FOR PTERYGIUM*. Br J Ophthalmol. 1945 Apr;29(4):193-6.
- 33.
- Wilson SE, Bourne WM. Conjunctival Z-plasty in the treatment of pterygium. Am J Ophthalmol. 1988 Sep 15;106(3):355-7. [PubMed]
- 34.
- Lewallen S. A randomized trial of conjunctival autografting for pterygium in the tropics. Ophthalmology. 1989 Nov;96(11):1612-4. [
- 35.
- Ti SE, Chee SP, Dear KB, Tan DT. Analysis of variation in success rates in conjunctival autografting for primary and recurrent pterygium. Br J Ophthalmol. 2000 Apr;84(4):385-9.
- 36.
- Kenyon KR, Wagoner MD, Hettinger ME. Conjunctival autograft transplantation for advanced and recurrent pterygium. Ophthalmology. 1985 Nov;92(11):1461-70.
- 37.
- Cohen RA, McDonald MB. Fixation of conjunctival autografts with an organic tissue adhesive. Arch Ophthalmol. 1993 Sep;111(9):1167-8.
- 38.
- Kumar S, Singh R. Pterygium excision and conjunctival autograft: A comparative study of techniques. Oman J Ophthalmol. 2018 May-Aug;11(2):124-128.
- 39.
- Haider TA, Al-Amin LM, Bamashmus MA, Ali SF. Ninety degree conjunctival rotation autograft versus zero and 180 degree rotation autograft for pterygium surgery. Saudi Med J. 2009 Apr;30(4):519-23.
- 40.
- Alp BN, Yanyali A, Ay GM, Keskin O. Conjunctival rotation autograft for primary pterygium. Ophthalmologica. 2002 Sep-Oct;216(5):333-6. [PubMed]
- 41.
- Gris O, Güell JL, del Campo Z. Limbal-conjunctival autograft transplantation for the treatment of recurrent pterygium. Ophthalmology. 2000 Feb;107(2):270-3. [PubMed]
- 42.
- Malik KP, Goel R, Gutpa A, Gupta SK, Kamal S, Mallik VK, Singh S. Efficacy of sutureless and glue free limbal conjunctival autograft for primary pterygium surgery. Nepal J Ophthalmol. 2012 Jul-Dec;4(2):230-5. [PubMed]
- 43.
- Al Fayez MF. Limbal versus conjunctival autograft transplantation for advanced and recurrent pterygium. Ophthalmology. 2002 Sep;109(9):1752-5. [PubMed]
- 44.
- Masters JS, Harris DJ. Low Recurrence Rate of Pterygium After Excision With Conjunctival Limbal Autograft: A Retrospective Study With Long-Term Follow-Up. Cornea. 2015 Dec;34(12):1569-72.
- 45.
- Fernandes M, Sangwan VS, Bansal AK, Gangopadhyay N, Sridhar MS, Garg P, Aasuri MK, Nutheti R, Rao GN. Outcome of pterygium surgery: analysis over 14 years. Eye (Lond). 2005 Nov;19(11):1182-90.
- 46.
- Syam PP, Eleftheriadis H, Liu CS. Inferior conjunctival autograft for primary pterygia. Ophthalmology. 2003 Apr;110(4):806-10.
- 47.
- Essex RW, Snibson GR, Daniell M, Tole DM. Amniotic membrane grafting in the surgical management of primary pterygium. Clin Exp Ophthalmol. 2004 Oct;32(5):501-4. [
- 48.
- Ma DH, See LC, Liau SB, Tsai RJ. Amniotic membrane graft for primary pterygium: comparison with conjunctival autograft and topical mitomycin C treatment. Br J Ophthalmol. 2000 Sep;84(9):973-8.
- 49.
- Laughrea PA, Arentsen JJ. Lamellar keratoplasty in the management of recurrent pterygium. Ophthalmic Surg. 1986 Feb;17(2):106-8. [
- 50.
- Rich AM, Kietzman B, Payne T, McPherson SD. A simplified way to remove pterygia. Ann Ophthalmol. 1974 Jul;6(7):739-42. [PubMed]
- 51.
- Murakami M, Mori S, Kunitomo N. [Studies on the pterygium. V. Follow-up information of mitomycin C treatment]. Nippon Ganka Gakkai Zasshi. 1967 Apr;71(4):351-8. [PubMed]
- 52.
- Singh G, Wilson MR, Foster CS. Mitomycin eye drops as treatment for pterygium. Ophthalmology. 1988 Jun;95(6):813-21. [PubMed]
- 53.
- Rubinfeld RS, Pfister RR, Stein RM, Foster CS, Martin NF, Stoleru S, Talley AR, Speaker MG. Serious complications of topical mitomycin-C after pterygium surgery. Ophthalmology. 1992 Nov;99(11):1647-54. [PubMed]
- 54.
- Tassy A, Ribe D. [Thiotepa eyedrops for prevention of pterygium recurrence: 18 years of use]. J Fr Ophtalmol. 1999 Mar;22(2):215-9. [PubMed]
- 55.
- Ngoy D, Kayembe L. [A comparative study of thio-tepa and mitomycin C in the treatment of pterygium. Preliminary results]. J Fr Ophtalmol. 1998 Feb;21(2):96-102.
- 56.
- Wu H, Chen G. [Cyclosporine A and thiotepa in prevention of postoperative recurrence of pterygium]. Yan Ke Xue Bao. 1999 Jun;15(2):91-2.
- 57.
- Bekibele CO, Baiyeroju AM, Olusanya BA, Ashaye AO, Oluleye TS. Pterygium treatment using 5-FU as adjuvant treatment compared to conjunctiva autograft. Eye (Lond). 2008 Jan;22(1):31-4.
- 58.
- Akarsu C, Taner P, Ergin A. 5-Fluorouracil as chemoadjuvant for primary pterygium surgery: preliminary report. Cornea. 2003 Aug;22(6):522-6. [PubMed]
- 59.
- Kasetsuwan N, Reinprayoon U, Satitpitakul V. Prevention of recurrent pterygium with topical bevacizumab 0.05% eye drops: a randomized controlled trial. Clin Ther. 2015 Oct 01;37(10):2347-51. [PubMed]
- 60.
- Yamada T, Mochizuki H, Ue T, Kiuchi Y, Takahashi Y, Oinaka M. Comparative study of different β-radiation doses for preventing pterygium recurrence. Int J Radiat Oncol Biol Phys. 2011 Dec 01;81(5):1394-8. [PubMed]
- 61.
- Ali AM, Thariat J, Bensadoun RJ, Thyss A, Rostom Y, El-Haddad S, Gérard JP. The role of radiotherapy in the treatment of pterygium: a review of the literature including more than 6000 treated lesions. Cancer Radiother. 2011 Apr;15(2):140-7. [PubMed]
- 62.
- Singh SK. Pterygium: epidemiology prevention and treatment. Community Eye Health. 2017;30(99):S5-S6. [PMC free article] [PubMed]
- 63.
- Solomon A, Pires RT, Tseng SC. Amniotic membrane transplantation after extensive removal of primary and recurrent pterygia. Ophthalmology. 2001 Mar;108(3):449-60. [PubMed]
- 64.
- Tan DT, Chee SP, Dear KB, Lim AS. Effect of pterygium morphology on pterygium recurrence in a controlled trial comparing conjunctival autografting with bare sclera excision. Arch Ophthalmol. 1997 Oct;115(10):1235-40. [PubMed]
- 65.
- Hirst LW, Smallcombe K. Double-Headed Pterygia Treated With P.E.R.F.E.C.T for PTERYGIUM. Cornea. 2017 Jan;36(1):98-100. [
- 66.
- Hirst LW. Recurrence and complications after 1,000 surgeries using pterygium extended removal followed by extended conjunctival transplant. Ophthalmology. 2012 Nov;119(11):2205-10.
- 67.
- Liu HY, Chen YF, Chen TC, Yeh PT, Hu FR, Chen WL. Surgical result of pterygium extended removal followed by fibrin glue-assisted amniotic membrane transplantation. J Formos Med Assoc. 2017 Jan;116(1):10-17.
- 68.
- Allam WA. Recurrence and complications of pterygium extended removal followed by extended conjunctival transplant for primary pterygia. Eur J Ophthalmol. 2016 May-Jun;26(3):203-8.
- 69.
- Cornelius CR. Recurrence Rate and Complications of Pterygium Extended Removal Followed by Extended Conjunctival Transplant. Cornea. 2017 Jan;36(1):101-103.
- 70.
- Maheshwari S. Pterygium-induced corneal refractive changes. Indian J Ophthalmol. 2007 Sep-Oct;55(5):383-6. [PubMed]