A Leader in Chronic Dry Eye Relief
COVID-19 Note: We are Still Open and Continuing to Ship!
TheraLife® targets the root cause of dry eyes – underactive tear productions. TheraLife® provides natural chronic dry eye relief by restoring and reviving the underactive cellular functions intra-cellularly to produce your own body’s healing tears. TheraLife EyeR is an oral capsule, not an eye drop.
TheraLife Eye capsules have proven clinically to work in people with dry eyes in 6 separate – 12-week clinical studies. TheraLife was shown to reduce symptoms of eye dryness in all six studies with improved tear production and corneal staining. Read more.
Dry eye syndrome often leads to severe complications such as blepharitis; meibomian gland dysfunction; ocular rosacea, watery eyes; chalazion; stye; and cornea abrasion. Using TheraLife Eye capsules to address the underlying issues of chronic dry eyes has proven to be effective in the eradication of blepharitis and the support normal functions of meibomian oil glands; stop tear over production in watery dry eyes, prevent recurrence of chalazion/styes from clogged oil glands; and reduce inflammation to ocular rosacea.
Crusty eye discharge is one of the most troublesome consequences of chronic dry eys. There are many reasons why eyes produce discharges. Conjunctivities ( pink eye) caused by bacterial or viral infections being the most common. Discharge from conjunctivitis is often white and can be yellowish.
Blepharitis, chronic inflammation of the eyelids, and meibomian gland dysfunction (MGD) clogging of the oil glands located on the eyelids can both give you greenish yellowish eye discharges. These eye discharges can be foamy, crusty, sticky, and painful. Blepharitis and MGD can be chronic because they are most often associated with chronic dry eyes.
After TheraLife®, you will once again have a natural ability to make balanced tears, eliminating painful inflammation and dryness. End your reliance on eye drops and restore your comfortable vision. TheraLife® can end pain and help you get your life back. Don’t waste time with treatments that don’t work. Try TheraLife® today!
 TheraLife® Eye Enhanced
TheraLife® Eye Enhanced
Doctor recommended and clinically proven to provide chronic dry eye relief in 80% of first time users. Our all natural formula provides chronic dry eye relief by restoring your eyes’ own natural ability to produce tears. Learn more | Buy Now
 TheraLife® Eye Autoimmune
TheraLife® Eye Autoimmune
Specifically formulated for individuals who suffer from dry eyes related to autoimmune diseases. Provides dry eye relief, dry mouth, joint pain, and fatigue from Sjogren’s Syndrome, Rheumatoid Arthritis, Graves’ Disease, and other conditions. Learn more | Buy Now
 TheraLife® Eye Enhanced Starter Kit
TheraLife® Eye Enhanced Starter Kit
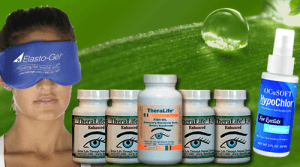
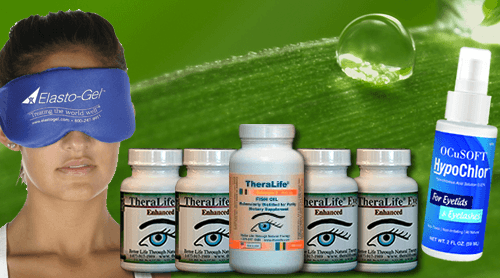
Everything you need for dry eye relief. Save money with our starter kit! Includes: 4 bottles TheraLife® Eye Enhanced, 1 bottle Omega-3 Fish Oil, 1 Eye Lid Cleanser, and 1 Hot Compress. TheraLife® especially recommends this starter kit to Blepharitis/MGD dry eye sufferers because it includes all of the elements that are essential for getting lasting dry eye relief, collected for you into one conveniently packaged solution. Learn more | Buy Now
 TheraLife® Autoimmune Starter Kit
TheraLife® Autoimmune Starter Kit
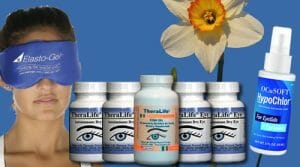
Everything you need to start treating chronic dry eyes related to autoimmune conditions. Includes: 4 bottles TheraLife® Eye Autoimmune, 1 bottle Omega-3 Fish Oil, 1 Eye Lid Cleanser, and 1 Hot Compress. TheraLife especially recommends this start kit for dry eyes from Sjogren’s Syndrome, Rheumatoid Arthritis, Ocular Rosacea, Graves’ disease, Raynaud’s, Lupus, Graft Versus Host disease, and other automimmune conditions. Learn more | Buy Now